A comparison of machine learning models versus clinical evaluation for mortality prediction in patients with sepsis
- PMID: 33465096
- PMCID: PMC7815112
- DOI: 10.1371/journal.pone.0245157
A comparison of machine learning models versus clinical evaluation for mortality prediction in patients with sepsis
Abstract
Introduction: Patients with sepsis who present to an emergency department (ED) have highly variable underlying disease severity, and can be categorized from low to high risk. Development of a risk stratification tool for these patients is important for appropriate triage and early treatment. The aim of this study was to develop machine learning models predicting 31-day mortality in patients presenting to the ED with sepsis and to compare these to internal medicine physicians and clinical risk scores.
Methods: A single-center, retrospective cohort study was conducted amongst 1,344 emergency department patients fulfilling sepsis criteria. Laboratory and clinical data that was available in the first two hours of presentation from these patients were randomly partitioned into a development (n = 1,244) and validation dataset (n = 100). Machine learning models were trained and evaluated on the development dataset and compared to internal medicine physicians and risk scores in the independent validation dataset. The primary outcome was 31-day mortality.
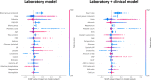
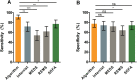
Results: A number of 1,344 patients were included of whom 174 (13.0%) died. Machine learning models trained with laboratory or a combination of laboratory + clinical data achieved an area-under-the ROC curve of 0.82 (95% CI: 0.80-0.84) and 0.84 (95% CI: 0.81-0.87) for predicting 31-day mortality, respectively. In the validation set, models outperformed internal medicine physicians and clinical risk scores in sensitivity (92% vs. 72% vs. 78%;p<0.001,all comparisons) while retaining comparable specificity (78% vs. 74% vs. 72%;p>0.02). The model had higher diagnostic accuracy with an area-under-the-ROC curve of 0.85 (95%CI: 0.78-0.92) compared to abbMEDS (0.63,0.54-0.73), mREMS (0.63,0.54-0.72) and internal medicine physicians (0.74,0.65-0.82).
Conclusion: Machine learning models outperformed internal medicine physicians and clinical risk scores in predicting 31-day mortality. These models are a promising tool to aid in risk stratification of patients presenting to the ED with sepsis.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
-
- Roest AA, Tegtmeier J, Heyligen JJ, Duijst J, Peeters A, Borggreve HF, et al. Risk stratification by abbMEDS and CURB-65 in relation to treatment and clinical disposition of the septic patient at the emergency department: a cohort study. BMC Emerg Med. 2015;15:29 Epub 2015/10/16. 10.1186/s12873-015-0056-z - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

