Effectiveness of In-Hospital Cholecalciferol Use on Clinical Outcomes in Comorbid COVID-19 Patients: A Hypothesis-Generating Study
- PMID: 33466642
- PMCID: PMC7828675
- DOI: 10.3390/nu13010219
Effectiveness of In-Hospital Cholecalciferol Use on Clinical Outcomes in Comorbid COVID-19 Patients: A Hypothesis-Generating Study
Abstract
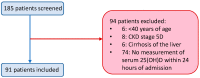
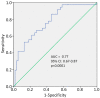
Little information is available on the beneficial effects of cholecalciferol treatment in comorbid patients hospitalized for COVID-19. The aim of this study was to retrospectively examine the clinical outcome of patients receiving in-hospital high-dose bolus cholecalciferol. Patients with a positive diagnosis of SARS-CoV-2 and overt COVID-19, hospitalized from 15 March to 20 April 2020, were considered. Based on clinical characteristics, they were supplemented (or not) with 400,000 IU bolus oral cholecalciferol (200,000 IU administered in two consecutive days) and the composite outcome (transfer to intensive care unit; ICU and/or death) was recorded. Ninety-one patients (aged 74 ± 13 years) with COVID-19 were included in this retrospective study. Fifty (54.9%) patients presented with two or more comorbid diseases. Based on the decision of the referring physician, 36 (39.6%) patients were treated with vitamin D. Receiver operating characteristic curve analysis revealed a significant predictive power of the four variables: (a) low (<50 nmol/L) 25(OH) vitamin D levels, (b) current cigarette smoking, (c) elevated D-dimer levels (d) and the presence of comorbid diseases, to explain the decision to administer vitamin D (area under the curve = 0.77, 95% CI: 0.67-0.87, p < 0.0001). Over the follow-up period (14 ± 10 days), 27 (29.7%) patients were transferred to the ICU and 22 (24.2%) died (16 prior to ICU and six in ICU). Overall, 43 (47.3%) patients experienced the combined endpoint of transfer to ICU and/or death. Logistic regression analyses revealed that the comorbidity burden significantly modified the effect of vitamin D treatment on the study outcome, both in crude (p = 0.033) and propensity score-adjusted analyses (p = 0.039), so the positive effect of high-dose cholecalciferol on the combined endpoint was significantly amplified with increasing comorbidity burden. This hypothesis-generating study warrants the formal evaluation (i.e., clinical trial) of the potential benefit that cholecalciferol can offer in these comorbid COVID-19 patients.
Keywords: COVID-19; cholecalciferol; comorbid disease; intensive care; mortality; propensity score; vitamin D.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Grasselli G., Zangrillo A., Zanella A., Antonelli M., Cabrini L., Castelli A., Cereda D., Coluccello A., Foti G., Fumagalli R., et al. Baseline Characteristics and Outcomes of 1591 Patients Infected With SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy. JAMA. 2020;323:1574–1581. doi: 10.1001/jama.2020.5394. - DOI - PMC - PubMed
-
- Richardson S., Hirsch J.S., Narasimhan M., Crawford J.M., McGinn T., Davidson K.W., Barnaby D.P., Becker L.B., Chelico J.D., Cohen S.L., et al. Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area. JAMA. 2020;323:2052–2059. doi: 10.1001/jama.2020.6775. - DOI - PMC - PubMed
-
- WHO WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19—11 March 2020. [(accessed on 21 November 2020)]; Available online: https://www.who.int/director-general/speeches/detail/who-director-genera....
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

