Changes in Type 2 Biomarkers After Anti-IL5 Treatment in Patients With Severe Eosinophilic Asthma
- PMID: 33474865
- PMCID: PMC7840863
- DOI: 10.4168/aair.2021.13.2.330
Changes in Type 2 Biomarkers After Anti-IL5 Treatment in Patients With Severe Eosinophilic Asthma
Abstract
Patients with severe eosinophilic asthma (SEA) suffer from frequent asthma exacerbations, where eosinophils are major effector cells in airway inflammation, and anti-interleukin (IL)-5 becomes an effective treatment modality to control eosinophilic inflammation of SEA. Fifteen patients with SEA who had been treated with anti-IL5 (reslizumab, 100 mg monthly intravenously) for 6 months at Ajou University Hospital (Suwon, Korea) were enrolled in this study. Clinical parameters, including total blood eosinophil count (TEC), FEV1%, fractional exhaled nitric oxide (FeNO) levels, and serum biomarkers such as eosinophil-derived neurotoxin (EDN), periostin (PON), and transforming growth factor-β1 (TGF-β1), were analyzed. EDN levels and TEC decreased significantly after 1 month of treatment (P < 0.05 for both), while no changes were noted in FeNO/PON/TGF-β1 levels. FEV1% increased after 2 months of treatment (P < 0.05). A positive correlation was observed between TEC and EDN levels (r = 0.60, P = 0.02). Significant negative correlations were noted between age and TEC/EDN levels (r = -0.57, P = 0.02 and r = -0.56, P = 0.03, respectively). Baseline TEC was higher in the EDN-responder group (≥75% decrease) than in the non-responder group (P = 0.06) with a positive correlation between %reduction in EDN and TEC (r = 0.67, P = 0.01). The onset age was younger and asthma duration was longer in the FEV1%-non-responder group (<12% increase) than in the FEV1%-responder group (P = 0.07 and P = 0.007, respectively). In conclusion, changes in the serum EDN level may be a potential biomarker for monitoring eosinophilic inflammation after anti-IL5 treatment in SEA, which is affected by onset age and asthma duration.
Keywords: Asthma; antibodies, monoclonal; asthma exacerbation; eosinophils; inflammation; interleukin-5.
Copyright © 2021 The Korean Academy of Asthma, Allergy and Clinical Immunology · The Korean Academy of Pediatric Allergy and Respiratory Disease.
Conflict of interest statement
There are no financial or other issues that might lead to conflict of interest.
Figures
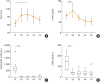

References
-
- Global Initiative for Asthma. Global strategy for asthma management and prevention. Global Initiative for Asthma; 2020. Available from: www.ginasthma.org.
-
- Wu AY, Sur S, Grant JA, Tripple JW. Interleukin-4/interleukin-13 versus interleukin-5: a comparison of molecular targets in biologic therapy for the treatment of severe asthma. Curr Opin Allergy Clin Immunol. 2019;19:30–37. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

