Development of a brain-computer interface for patients in the critical care setting
- PMID: 33481888
- PMCID: PMC7822274
- DOI: 10.1371/journal.pone.0245540
Development of a brain-computer interface for patients in the critical care setting
Abstract
Objective: Behaviorally unresponsive patients in intensive care units (ICU) are unable to consistently and effectively communicate their most fundamental physical needs. Brain-Computer Interface (BCI) technology has been established in the clinical context, but faces challenges in the critical care environment. Contrary to cue-based BCIs, which allow activation only during pre-determined periods of time, self-paced BCI systems empower patients to interact with others at any time. The study aims to develop a self-paced BCI for patients in the intensive care unit.
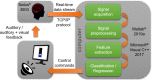
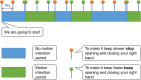
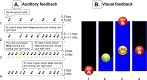
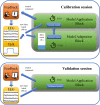
Methods: BCI experiments were conducted in 18 ICU patients and 5 healthy volunteers. The proposed self-paced BCI system analyzes EEG activity from patients while these are asked to control a beeping tone by performing a motor task (i.e., opening and closing a hand). Signal decoding is performed in real time and auditory feedback given via headphones. Performance of the BCI system was judged based on correlation between the optimal and the observed performance.
Results: All 5 healthy volunteers were able to successfully perform the BCI task, compared to chance alone (p<0.001). 5 of 14 (36%) conscious ICU patients were able to perform the BCI task. One of these 5 patients was quadriplegic and controlled the BCI system without any hand movements. None of the 4 unconscious patients were able to perform the BCI task.
Conclusions: More than one third of conscious ICU patients and all healthy volunteers were able to gain control over the self-paced BCI system. The initial 4 unconscious patients were not. Future studies will focus on studying the ability of behaviorally unresponsive patients with cognitive motor dissociation to control the self-paced BCI system.
Conflict of interest statement
Jan Claassen is a minority shareholder at iCE Neurosystems. This does not alter our adherence to PLOS ONE policies on sharing data and materials.
Figures

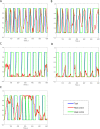
Similar articles
-
A multi-modal modified feedback self-paced BCI to control the gait of an avatar.J Neural Eng. 2021 Apr 6;18(5). doi: 10.1088/1741-2552/abee51. J Neural Eng. 2021. PMID: 33711832
-
A hybrid NIRS-EEG system for self-paced brain computer interface with online motor imagery.J Neurosci Methods. 2015 Apr 15;244:26-32. doi: 10.1016/j.jneumeth.2014.04.016. Epub 2014 May 2. J Neurosci Methods. 2015. PMID: 24797225
-
A novel Morse code-inspired method for multiclass motor imagery brain-computer interface (BCI) design.Comput Biol Med. 2015 Nov 1;66:11-9. doi: 10.1016/j.compbiomed.2015.08.011. Epub 2015 Aug 24. Comput Biol Med. 2015. PMID: 26340647
-
Brain-Computer Interfaces in Quadriplegic Patients.Neurosurg Clin N Am. 2019 Apr;30(2):275-281. doi: 10.1016/j.nec.2018.12.009. Epub 2019 Feb 18. Neurosurg Clin N Am. 2019. PMID: 30898278 Review.
-
From classic motor imagery to complex movement intention decoding: The noninvasive Graz-BCI approach.Prog Brain Res. 2016;228:39-70. doi: 10.1016/bs.pbr.2016.04.017. Epub 2016 May 31. Prog Brain Res. 2016. PMID: 27590965 Review.
Cited by
-
Electroencephalogram in the intensive care unit: a focused look at acute brain injury.Intensive Care Med. 2022 Oct;48(10):1443-1462. doi: 10.1007/s00134-022-06854-3. Epub 2022 Aug 23. Intensive Care Med. 2022. PMID: 35997792 Free PMC article. Review.
-
Cognitive Motor Dissociation: Gap Analysis and Future Directions.Neurocrit Care. 2024 Feb;40(1):81-98. doi: 10.1007/s12028-023-01769-3. Epub 2023 Jun 22. Neurocrit Care. 2024. PMID: 37349602
-
EEG-based Brain-Computer Interfaces for people with Disorders of Consciousness: Features and applications. A systematic review.Front Hum Neurosci. 2022 Dec 5;16:1040816. doi: 10.3389/fnhum.2022.1040816. eCollection 2022. Front Hum Neurosci. 2022. PMID: 36545350 Free PMC article.
-
Assessing Consciousness through Neurofeedback and Neuromodulation: Possibilities and Challenges.Life (Basel). 2023 Aug 2;13(8):1675. doi: 10.3390/life13081675. Life (Basel). 2023. PMID: 37629532 Free PMC article. Review.
-
Importance, limits and caveats of the use of "disorders of consciousness" to theorize consciousness.Neurosci Conscious. 2022 Feb 16;2021(2):niab048. doi: 10.1093/nc/niab048. eCollection 2021. Neurosci Conscious. 2022. PMID: 35369675 Free PMC article. Review.
References
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

