Association of Epileptic and Nonepileptic Seizures and Changes in Circulating Plasma Proteins Linked to Neuroinflammation
- PMID: 33495377
- PMCID: PMC8055314
- DOI: 10.1212/WNL.0000000000011552
Association of Epileptic and Nonepileptic Seizures and Changes in Circulating Plasma Proteins Linked to Neuroinflammation
Abstract
Objective: To develop a diagnostic test that stratifies epileptic seizures (ES) from psychogenic nonepileptic seizures (PNES) by developing a multimodal algorithm that integrates plasma concentrations of selected immune response-associated proteins and patient clinical risk factors for seizure.
Methods: Daily blood samples were collected from patients evaluated in the epilepsy monitoring unit within 24 hours after EEG confirmed ES or PNES and plasma was isolated. Levels of 51 candidate plasma proteins were quantified using an automated, multiplexed, sandwich ELISA and then integrated and analyzed using our diagnostic algorithm.
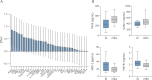
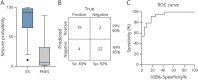
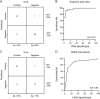
Results: A 51-protein multiplexed ELISA panel was used to determine the plasma concentrations of patients with ES, patients with PNES, and healthy controls. A combination of protein concentrations, tumor necrosis factor-related apoptosis-inducing ligand (TRAIL), intercellular adhesion molecule 1 (ICAM-1), monocyte chemoattractant protein-2 (MCP-2), and tumor necrosis factor-receptor 1 (TNF-R1) indicated a probability that a patient recently experienced a seizure, with TRAIL and ICAM-1 levels higher in PNES than ES and MCP-2 and TNF-R1 levels higher in ES than PNES. The diagnostic algorithm yielded an area under the receiver operating characteristic curve (AUC) of 0.94 ± 0.07, sensitivity of 82.6% (95% confidence interval [CI] 62.9-93.0), and specificity of 91.6% (95% CI 74.2-97.7). Expanding the diagnostic algorithm to include previously identified PNES risk factors enhanced diagnostic performance, with AUC of 0.97 ± 0.05, sensitivity of 91.3% (95% CI 73.2-97.6), and specificity of 95.8% (95% CI 79.8-99.3).
Conclusions: These 4 plasma proteins could provide a rapid, cost-effective, and accurate blood-based diagnostic test to confirm recent ES or PNES.
Classification of evidence: This study provides Class III evidence that variable levels of 4 plasma proteins, when analyzed by a diagnostic algorithm, can distinguish PNES from ES with sensitivity of 82.6% and specificity of 91.6%.
© 2021 American Academy of Neurology.
Figures

Comment in
-
A Better Blood Test to Differentiate Epileptic From Psychogenic Nonepileptic Seizures?Neurology. 2021 Mar 9;96(10):467-468. doi: 10.1212/WNL.0000000000011593. Epub 2021 Jan 25. Neurology. 2021. PMID: 33495375 No abstract available.
-
The Molecular Dichotomy Between Epileptic and Functional Seizures.Epilepsy Curr. 2021 Apr 28;21(4):258-260. doi: 10.1177/15357597211011983. eCollection 2021 Jul-Aug. Epilepsy Curr. 2021. PMID: 34690561 Free PMC article. No abstract available.
References
-
- Singh UK, Jana UK. Plasma prolactin in epilepsy and pseudoseizures. Indian Pediatr 1994;31:667–669. - PubMed
-
- Tumani H, Otto M, Gefeller O, et al. Kinetics of serum neuron-specific enolase and prolactin in patients after single epileptic seizures. Epilepsia 1999;40:713–718. - PubMed
-
- Vukmir RB. Does serum prolactin indicate the presence of seizure in the emergency department patient? J Neurol 2004;251:736–739. - PubMed
-
- Sundararajan T, Tesar GE, Jimenez XF. Biomarkers in the diagnosis and study of psychogenic nonepileptic seizures: a systematic review. Seizure 2016;35:11–22. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous
