Infrapatellar versus suprapatellar approach for intramedullary nailing of the tibia: a systematic review and meta-analysis
- PMID: 33509237
- PMCID: PMC7844899
- DOI: 10.1186/s13018-021-02249-0
Infrapatellar versus suprapatellar approach for intramedullary nailing of the tibia: a systematic review and meta-analysis
Abstract
Background: Intramedullary nailing (IMN) is a conventional technique for the treatment of tibial shaft fractures. It has been suggested that the suprapatellar (SP) approach holds advantages over the traditional infrapatellar (IP) approach. Current literature lacks adequate data to provide robust clinical recommendations. This meta-analysis aims to determine the efficacy of infrapatellar versus suprapatellar techniques for IMN.
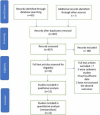
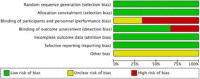
Methods: An up-to-date literature search of the Embase, Medline, and registry platform databases was performed. The search was conducted using a predesigned search strategy and all eligible literature was critically appraised for methodological quality via the Cochrane's collaboration tool. Fluoroscopy time, operative time, pain score, knee function, deep infection, non-union and secondary operation rates were all considered.
Conclusion: A total of twelve studies were included in the meta-analysis. The results of this analysis show that suprapatellar nailing is associated with reduced post-operative pain scores and improved functional outcomes. The data suggest no significant difference in terms of operative times, fluoroscopy times, rates of deep infection, non-union or secondary procedures when compared to infra-patellar techniques. Further studies are required to confirm these findings and assess long-term results.
Keywords: Fixation; Infrapatellar; Suprapatellar; Tibia fracture.
Conflict of interest statement
None
Figures

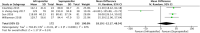
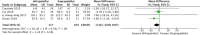
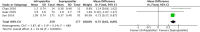


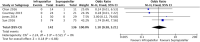
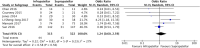
Similar articles
-
Suprapatellar versus infrapatellar approach for tibia intramedullary nailing: A meta-analysis.Int J Surg. 2018 Mar;51:133-139. doi: 10.1016/j.ijsu.2018.01.026. Epub 2018 Jan 31. Int J Surg. 2018. PMID: 29367045 Review.
-
Comparison of clinical, radiological and functional outcome between the supra-patellar and infra-patellar techniques of Tibial nailing in Indian population: A prospective, randomized controlled trial.Injury. 2025 Aug;56(8):112471. doi: 10.1016/j.injury.2025.112471. Epub 2025 Jun 5. Injury. 2025. PMID: 40532333 Clinical Trial.
-
Suprapatellar versus infrapatellar approaches in the treatment of tibia intramedullary nailing: a retrospective cohort study.BMC Musculoskelet Disord. 2019 Nov 28;20(1):573. doi: 10.1186/s12891-019-2961-x. BMC Musculoskelet Disord. 2019. PMID: 31779596 Free PMC article.
-
Suprapatellar versus infrapatellar intramedullary nailing for treatment of tibial shaft fractures in adults.Medicine (Baltimore). 2018 Aug;97(32):e11799. doi: 10.1097/MD.0000000000011799. Medicine (Baltimore). 2018. PMID: 30095643 Free PMC article.
-
The efficacy of suprapatellar, parapatellar and infrapatellar intramedullary nailing in the treatment of tibial fractures: a systematic review and meta-analysis.Arch Orthop Trauma Surg. 2024 Nov;144(11):4917-4927. doi: 10.1007/s00402-024-05584-z. Epub 2024 Sep 26. Arch Orthop Trauma Surg. 2024. PMID: 39325161
Cited by
-
A systematic review and meta-analysis comparing suprapatellar versus infrapatellar approach intramedullary nailing for tibal shaft fractures.Eur J Trauma Emerg Surg. 2024 Apr;50(2):383-394. doi: 10.1007/s00068-023-02384-9. Epub 2023 Nov 21. Eur J Trauma Emerg Surg. 2024. PMID: 37989960 Free PMC article.
-
A matched comparison of suprapatellar and infrapatellar approaches in intramedullary nailing for distal tibial fractures: a study of alignment including rotation and mid-term outcomes.Eur J Trauma Emerg Surg. 2025 Jul 21;51(1):260. doi: 10.1007/s00068-025-02938-z. Eur J Trauma Emerg Surg. 2025. PMID: 40691316 No abstract available.
-
Suprapatellar vs infrapatellar approaches for intramedullary nailing of distal tibial fractures: a systematic review and meta-analysis.J Orthop Traumatol. 2023 Apr 11;24(1):14. doi: 10.1186/s10195-023-00694-7. J Orthop Traumatol. 2023. PMID: 37041367 Free PMC article.
-
Suprapatellar intramedullary nailing of tibial shaft fractures in pregnancy. A report of two cases.BMC Pregnancy Childbirth. 2022 Jun 28;22(1):528. doi: 10.1186/s12884-022-04835-4. BMC Pregnancy Childbirth. 2022. PMID: 35765043 Free PMC article.
-
Tibial Intramedullary Nailing by Suprapatellar Approach: Is It Quicker and Safer?Cureus. 2022 Oct 4;14(10):e29915. doi: 10.7759/cureus.29915. eCollection 2022 Oct. Cureus. 2022. PMID: 36348901 Free PMC article.
References
-
- Court-Brown CM, Caesar B. Epidemiology of adult fractures: a review. Injury. 2006. 10.1016/j.injury.2006.04.130. - PubMed
-
- Bode G, Strohm PC, Südkamp NP, Hammer TO. Tibial shaft fractures - management and treatment options. A review of the current literature. Acta chirurgiae orthopaedicae et traumatologiae Cechoslovaca. 2012;79(6)499–505. - PubMed
-
- Lefaivre KA, Guy P, Chan H, Blachut PA. Long-term follow-up of tibial shaft fractures treated with intramedullary nailing. J Orthop Trauma. 2008. 10.1097/BOT.0b013e318180e646. - PubMed
-
- Väistö O, Toivanen J, Kannus P, Järvinen M. Anterior knee pain after intramedullary nailing of fractures of the tibial shaft: an eight-year follow-up of a prospective, randomized study comparing two different nail-insertion techniques. J Trauma InjInfect Crit Care. 2008. 10.1097/TA.0b013e318031cd27. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

