Danhong Injection and Trimetazidine Protect Cardiomyocytes and Enhance Calcium Handling after Myocardial Infarction
- PMID: 33510801
- PMCID: PMC7822665
- DOI: 10.1155/2021/2480465
Danhong Injection and Trimetazidine Protect Cardiomyocytes and Enhance Calcium Handling after Myocardial Infarction
Abstract
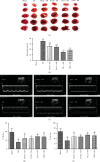
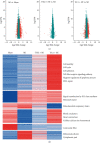
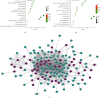
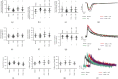
Myocardial infarction (MI) is one of the leading causes of death worldwide. However, there is no effective treatment for MI. In this study, trimetazidine (TMZ) and Danhong injection (DHI), representing western medicine and traditional Chinese medicine for MI, were used as tools to identify vital processes in alleviating MI injury. Administration of DHI and TMZ obviously decreased myocardial infarct size, improved ultrasonic heart function, and reduced creatine kinase (CK), lactate dehydrogenase (LDH), and glutamic oxaloacetic transaminase (AST) levels after MI. RNA-seq results indicated calcium ion handling and negative regulation of apoptotic process were vital processes and DHI and TMZ obviously reduced the expression of CaMK II and inhibited cleaved caspase-3 and Bax. Furthermore, DHI and TMZ increased p-S16-PLB, p-S16T17-PLB, CACNA1C, p-RyR2, and p-PKA expression but did not affect SERCA2a expression. In addition to the enhancement of cardiac myocyte shortening amplitude, maximum shortening velocity, and calcium transients, DHI and TMZ increased sarcoplasmic reticulum calcium content and enhanced SERCA2a calcium uptake capability by upregulating the phosphorylation of PLB but did not affect calcium exclusion by NCX. In conclusion, DHI and TMZ protect against MI through inhibiting apoptosis by downregulating CaMKII pathway and enhancing cardiac myocyte contractile functions possibly through the PKA signaling pathway.
Copyright © 2021 Jingjing Zhang et al.
Conflict of interest statement
The authors declare that they have no conflicts of interest.
Figures


Similar articles
-
Trimetazidine protects cardiomyocytes against hypoxia-induced injury through ameliorates calcium homeostasis.Chem Biol Interact. 2015 Jul 5;236:47-56. doi: 10.1016/j.cbi.2015.04.022. Epub 2015 May 1. Chem Biol Interact. 2015. PMID: 25937560
-
Trimetazidine protects against myocardial ischemia/reperfusion injury by inhibiting excessive autophagy.J Mol Med (Berl). 2018 Aug;96(8):791-806. doi: 10.1007/s00109-018-1664-3. Epub 2018 Jun 29. J Mol Med (Berl). 2018. PMID: 29955901
-
Insulin inhibits beta-adrenergic action in ischemic/reperfused heart: a novel mechanism of insulin in cardioprotection.Apoptosis. 2008 Feb;13(2):305-17. doi: 10.1007/s10495-007-0169-2. Apoptosis. 2008. PMID: 18165901
-
Amelioration of cardiac dysfunction and ventricular remodeling after myocardial infarction by danhong injection are critically contributed by anti-TGF-β-mediated fibrosis and angiogenesis mechanisms.J Ethnopharmacol. 2016 Dec 24;194:559-570. doi: 10.1016/j.jep.2016.10.025. Epub 2016 Oct 8. J Ethnopharmacol. 2016. PMID: 27729285
-
Danhong Injection (a Traditional Chinese Patent Medicine) for Acute Myocardial Infarction: A Systematic Review and Meta-Analysis.Evid Based Complement Alternat Med. 2015;2015:646530. doi: 10.1155/2015/646530. Epub 2015 Sep 14. Evid Based Complement Alternat Med. 2015. PMID: 26451156 Free PMC article. Review.
Cited by
-
Danhong Injection Up-regulates miR-125b in Endothelial Exosomes and Attenuates Apoptosis in Post-Infarction Myocardium.Chin J Integr Med. 2023 Dec;29(12):1099-1110. doi: 10.1007/s11655-023-3647-7. Epub 2023 Aug 18. Chin J Integr Med. 2023. PMID: 37594702
-
Trimetazidine Affects Mitochondrial Calcium Uniporter Expression to Restore Ischemic Heart Function via Reactive Oxygen Species/NFκB Pathway Inhibition.J Cardiovasc Pharmacol. 2023 Aug 1;82(2):104-116. doi: 10.1097/FJC.0000000000001434. J Cardiovasc Pharmacol. 2023. PMID: 37163369 Free PMC article.
-
Protective Effects of Allicin on Acute Myocardial Infarction in Rats via Hydrogen Sulfide-mediated Regulation of Coronary Arterial Vasomotor Function and Myocardial Calcium Transport.Front Pharmacol. 2022 Jan 3;12:752244. doi: 10.3389/fphar.2021.752244. eCollection 2021. Front Pharmacol. 2022. PMID: 35046802 Free PMC article.
-
The traditional Chinese medicines treat chronic heart failure and their main bioactive constituents and mechanisms.Acta Pharm Sin B. 2023 May;13(5):1919-1955. doi: 10.1016/j.apsb.2023.02.005. Epub 2023 Feb 11. Acta Pharm Sin B. 2023. PMID: 37250151 Free PMC article. Review.
-
Trend of Galectin-3 Levels in Patients with Non-ST-Elevation and ST-Elevation Myocardial Infarction.Medicina (Kaunas). 2022 Feb 14;58(2):286. doi: 10.3390/medicina58020286. Medicina (Kaunas). 2022. PMID: 35208606 Free PMC article.
References
-
- Reed G. W., Rossi J. E., Cannon C. P. Acute myocardial infarction. Lancet. 2016;389:p. 197. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

