Indirect inguinal hernia containing portosystemic shunt vessel: A case report
- PMID: 33521123
- PMCID: PMC7812899
- DOI: 10.12998/wjcc.v9.i2.509
Indirect inguinal hernia containing portosystemic shunt vessel: A case report
Abstract
Background: Inguinal hernia repair is one of the most common general surgical operations worldwide. We present a case of indirect inguinal hernia containing an expanded portosystemic shunt vessel.
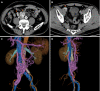
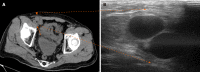
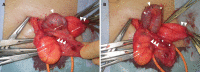
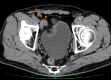
Case summary: We report a 72-year-old man who had a 4 cm × 4 cm swelling in the right inguinal region, which disappeared with light manual pressure. Abdominal-pelvic computed tomography (CT) revealed a right inguinal hernia containing an expanded portosystemic shunt vessel, which had been noted for 7 years due to liver cirrhosis. We performed Lichtenstein's herniorrhaphy and identified the hernia sac as being indirect and the shunt vessel existing in the extraperitoneal cavity through the internal inguinal ring. Then, we found two short branches between the expanded shunt vessel and testicular vein in the middle part of the inguinal canal and cut these branches to allow the shunt vessel to return to the extraperitoneal cavity of the abdomen. The hernia sac was returned as well. We encountered no intraoperative complications. After discharge, groin seroma requiring puncture at the outpatient clinic was observed.
Conclusion: If an inguinal hernia patient has portal hypertension, ultrasound should be used to determine the contents of the hernia. When atypical vessels are visualized, they may be shunt vessels and additional CT is recommended to ensure the selection of an adequate approach for safe hernia repair.
Keywords: Case report; Inguinal hernia; Lichtenstein’s herniorrhaphy; Portal hypertension; Portosystemic shunt; Shunt vessel.
©The Author(s) 2021. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: All authors declare no conflicts of interest.
Figures

Similar articles
-
Hybrid method using laparoscopy and Lichtenstein's technique for incarcerated inguinal hernia in a patient with liver cirrhosis and severe varicose veins: A case report.Int J Surg Case Rep. 2021 Aug;85:106207. doi: 10.1016/j.ijscr.2021.106207. Epub 2021 Jul 22. Int J Surg Case Rep. 2021. PMID: 34343796 Free PMC article.
-
The TREPP as alternative technique for recurrent inguinal hernia after Lichtenstein's repair: A consecutive case series.Int J Surg. 2017 Apr;40:73-77. doi: 10.1016/j.ijsu.2017.02.022. Epub 2017 Feb 20. Int J Surg. 2017. PMID: 28219816
-
Rare complication of lumboperitoneal shunt with distal catheter migration into the inguinal hernia sac in two adults: A case report.Surg Neurol Int. 2023 Nov 10;14:392. doi: 10.25259/SNI_389_2023. eCollection 2023. Surg Neurol Int. 2023. PMID: 38053705 Free PMC article.
-
Laparoscopic extraperitoneal approach to acutely incarcerated inguinal hernia.Surg Endosc. 2004 Feb;18(2):228-31. doi: 10.1007/s00464-003-8185-y. Epub 2003 Nov 26. Surg Endosc. 2004. PMID: 14639475 Review.
-
Absent external oblique musculo-aponeurotic complex during inguinal hernioplasty: a case report and review of literature.Surg Radiol Anat. 2017 Sep;39(9):1045-1048. doi: 10.1007/s00276-017-1815-1. Epub 2017 Mar 3. Surg Radiol Anat. 2017. PMID: 28255618 Review.
References
-
- Nordin P, Bartelmess P, Jansson C, Svensson C, Edlund G. Randomized trial of Lichtenstein versus Shouldice hernia repair in general surgical practice. Br J Surg. 2002;89:45–49. - PubMed
-
- Amid PK. Lichtenstein tension-free hernioplasty: its inception, evolution, and principles. Hernia. 2004;8:1–7. - PubMed
-
- Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, de Lange D, Fortelny R, Heikkinen T, Kingsnorth A, Kukleta J, Morales-Conde S, Nordin P, Schumpelick V, Smedberg S, Smietanski M, Weber G, Miserez M. European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia. 2009;13:343–403. - PMC - PubMed
-
- Wu JJ, Way JA, Eslick GD, Cox MR. Transabdominal Pre-Peritoneal Versus Open Repair for Primary Unilateral Inguinal Hernia: A Meta-analysis. World J Surg. 2018;42:1304–1311. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

