Gastrointestinal symptoms, pathophysiology, and treatment in COVID-19
- PMID: 33521210
- PMCID: PMC7836435
- DOI: 10.1016/j.gendis.2020.08.013
Gastrointestinal symptoms, pathophysiology, and treatment in COVID-19
Abstract
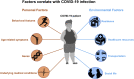
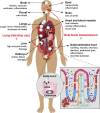
The novel coronavirus Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) has emerged and is responsible for the Coronavirus Disease 2019 global pandemic. Coronaviruses, including SARS-CoV-2, are strongly associated with respiratory symptoms during infection, but gastrointestinal symptoms, such as diarrhea, vomiting, nausea, and abdominal pain, have been identified in subsets of COVID-19 patients. This article focuses on gastrointestinal symptoms and pathophysiology in COVID-19 disease. Evidence suggests that the gastrointestinal tract could be a viral target for SARS-CoV-2 infection. Not only is the SARS-CoV-2 receptor ACE2 highly expressed in the GI tract and is associated with digestive symptoms, but bleeding and inflammation are observed in the intestine of COVID-19 patients. We further systemically summarize the correlation between COVID-19 disease, gastrointestinal symptoms and intestinal microbiota. The potential oral-fecal transmission of COVID-19 was supported by viral RNA and live virus detection in the feces of COVID-19 patients. Additionally, the viral balance in the GI tract could be disordered during SARS-CoV-2 infection which could further impact the homeostasis of the gut microbial flora. Finally, we discuss the clinical and ongoing trials of treatments/therapies, including antiviral drugs, plasma transfusion and immunoglobulins, and diet supplementations for COVID-19. By reviewing the pathogenesis of SARS-CoV-2 virus, and understanding the correlation among COVID-19, inflammation, intestinal microbiota, and lung microbiota, we provide perspective in prevention and control, as well as diagnosis and treatment of the COVID-19 disease.
Keywords: ACE-2; COVID-19; Cytokine; GI symptoms; Inflammation; Microbiota; SARS-CoV-2; Vitamin D.
Figures

References
-
- Coronavirus 2019-nCoV C Coronavirus 2019-nCoV global cases by Johns Hopkins CSSE. https://gisanddata.maps.arcgis.com/apps/opsdashboard/index.html#/bda7594... Accessed.
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

