Correlation of BODE index with quality of life in stable Chronic Obstructive Pulmonary Disease (COPD) patients - A prospective study
- PMID: 33532403
- PMCID: PMC7842444
- DOI: 10.4103/jfmpc.jfmpc_735_20
Correlation of BODE index with quality of life in stable Chronic Obstructive Pulmonary Disease (COPD) patients - A prospective study
Abstract
Background and aims: Chronic obstructive pulmonary disease (COPD) is characterized by slow progressive deterioration of respiratory function with systemic effects which have a great impact on health-related quality of life (HRQoL). The severity of airflow limitation in COPD, as reflected by forced expiratory volume in one second (FEV1) does not represent the systemic consequences of COPD. Hence, a multidimensional grading system, BODE index (Body mass index, Airflow obstruction, Dyspnea and Exercise capacity) that assessed both the pulmonary and systemic manifestations has recently been proposed to provide useful prognostic information and predict the outcome in COPD patients. The objective of this study was to evaluate the relationship between BODE index and health-related quality of life (HRQOL) in stable COPD patients and its usefulness in predicting the disease exacerbations.
Materials and methods: Sixty stable COPD patients who presented in the out-patient departments of Medicine and Pulmonology were recruited over one year period. We evaluated them by body-mass index, forced expiratory volume in one second (FEV1), Modified Medical Research Council dyspnea scale and six minute walk test (6MWT). BODE index was calculated using these variables. Disease duration, number of exacerbations and hospitalization in the previous year were recorded. We also administered the St. George's Respiratory Questionnaire (SGRQ) to assess the health related quality of life (HRQoL) in these patients. BODE scores were categorized into four quartiles, quartile one to four with scores of 0-2, 3-4, 5-6 and 7-10, respectively.
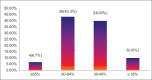
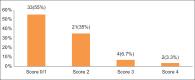
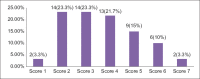
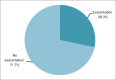
Results: According to BODE score, (16) 26.7% of patients were BODE 1, (27) 45% BODE 2, (15) 25% BODE 3 and (2) 3.3% were BODE 4. Higher BODE quartiles were associated with higher total SGRQ scores and SGRQ subscale scores (symptom, activity and impact). Very strong correlations were found between BODE quartiles and total SGRQ scores (P < 0.01). Among the components of BODE index, the decrease in the FEV1 (%predicted) and 6MWD, and the increase of MMRC dyspnea grade were associated with worsening of health status (increase in total SGRQ and SGRQ subscales). BODE index also correlated with the acute exacerbations (P < 0.0012) during one year follow-up.
Conclusion: BODE index strongly correlated with the HRQoL and also reliably predicted acute exacerbations in stable COPD patients.
Keywords: Airflow obstruction; body mass index; dyspnea; exercise capacity; quality of life; questionnaire.
Copyright: © 2020 Journal of Family Medicine and Primary Care.
Conflict of interest statement
There are no conflicts of interest. The study has received clearance from the ethical committee of Post graduate studies of Tata Main Hospital. Informed consent was taken from all the participants.
Figures



Similar articles
-
Evaluation of correlation of BODE index with health-related quality of life among patients with stable COPD attending a tertiary care hospital.Lung India. 2015 Jan-Feb;32(1):24-8. doi: 10.4103/0970-2113.148434. Lung India. 2015. PMID: 25624592 Free PMC article.
-
The cross-sectional and longitudinal association of the BODE index with quality of life in patients with chronic obstructive pulmonary disease.Chin Med J (Engl). 2009 Dec 20;122(24):2939-44. Chin Med J (Engl). 2009. PMID: 20137478
-
Behavior of Quality of Life (SGRQ) in COPD Patients According to BODE Scores.Arch Bronconeumol. 2015 Jul;51(7):315-21. doi: 10.1016/j.arbres.2014.02.017. Epub 2015 Jan 23. Arch Bronconeumol. 2015. PMID: 25622995 English, Spanish.
-
Does the multidimensional grading system (BODE) correspond to differences in health status of patients with COPD?Int J Chron Obstruct Pulmon Dis. 2006;1(1):91-6. doi: 10.2147/copd.2006.1.1.91. Int J Chron Obstruct Pulmon Dis. 2006. PMID: 18046907 Free PMC article.
-
Effect of Antioxidants in the Treatment of COPD Patients: Scoping Review.J Nutr Metab. 2021 Nov 24;2021:7463391. doi: 10.1155/2021/7463391. eCollection 2021. J Nutr Metab. 2021. PMID: 34868678 Free PMC article.
Cited by
-
Phenotypes of Exacerbations in Chronic Obstructive Pulmonary Disease.J Clin Med. 2025 Apr 30;14(9):3132. doi: 10.3390/jcm14093132. J Clin Med. 2025. PMID: 40364162 Free PMC article. Review.
-
Analysis of the Effect of Mindfulness Behavior Intervention Combined with Progressive Breathing Training on Pulmonary Function Rehabilitation in Patients with Chronic Obstructive Pulmonary Disease.Emerg Med Int. 2022 Aug 27;2022:1698918. doi: 10.1155/2022/1698918. eCollection 2022. Emerg Med Int. 2022. Retraction in: Emerg Med Int. 2023 Oct 18;2023:9831797. doi: 10.1155/2023/9831797. PMID: 36065224 Free PMC article. Retracted.
References
-
- Pauwels RA, Buist AS, Calverley PM, Jenkins CR, Hurd SS. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: NHLBI/WHO Global Initiative for Chronic Obstructive Lung Disease (GOLD) Workshop summary. Am J Respir Crit Care Med. 2001;163:1256–76. - PubMed
-
- Murray CJL, Lopez AD. Mortality by cause for eight regions of the world: Global Burden of Disease Study. Lancet. 1997;349:1269–76. - PubMed
-
- Jones PW, Wijkstra PJ. Quality of life in patients with chronic obstructive pulmonary disease in: Management of Chronic Obstructive Pulmonary Disease. Eur Respir Mon. 2006;38:375–86.
LinkOut - more resources
Full Text Sources
