Sleep and mental health in athletes during COVID-19 lockdown
- PMID: 33535229
- PMCID: PMC7928674
- DOI: 10.1093/sleep/zsaa261
Sleep and mental health in athletes during COVID-19 lockdown
Abstract
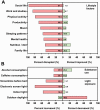
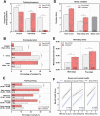
The global coronavirus 19 (COVID-19) pandemic and associated lockdown restrictions resulted in the majority of sports competitions around the world being put on hold. This includes the National Basketball Association, the UEFA Champions League, Australian Football League, the Tokyo 2020 Olympic Games, and regional competitions. The mitigation strategies in place to control the pandemic have caused disruption to daily schedules, working environments, and lifestyle factors. Athletes rely on regular access to training facilities, practitioners, and coaches to maintain physical and mental health to achieve maximal performance and optimal recovery. Furthermore, participation in sport at any level increases social engagement and promotes better mental health. It is, therefore, critical to understanding how the COVID-19 pandemic and associated lockdown measures have affected the lives of athletes. We surveyed elite and sub-elite athletes (n = 565) across multiple sports. Significant disruptions were reported for all lifestyle factors including social interactions, physical activity, sleep patterns, and mental health. We found a significant increase in total sleep time and sleep latency, as well as a delay in mid-sleep times and a decrease in social jetlag. Training frequency and duration significantly decreased. Importantly, the changes to training and sleep-related factors were associated with mental health outcomes. With spikes in COVID-19 cases rising around the world and governments reinstituting lockdowns (e.g. United Kingdom; Melbourne, Australia; California, USA) these results will inform messaging and strategies to better manage sleep and mental health in a population for whom optimal performance is critical.
Keywords: COVID-19; athletes; chronotype; elite; exercise; lockdown; mental health; pandemic; sleep; sports psychology; training.
© Sleep Research Society 2021. Published by Oxford University Press on behalf of the Sleep Research Society. All rights reserved. For permissions, please e-mail journals.permissions@oup.com.
Figures
Similar articles
-
The effects of the COVID-19 pandemic on the use of the performance-enhancing drugs.Acta Biomed. 2022 Jan 19;92(6):e2021401. doi: 10.23750/abm.v92i6.12377. Acta Biomed. 2022. PMID: 35075058 Free PMC article.
-
Sleep behavior and training load in adolescent elite basketball players during COVID-19 pandemic development.Chronobiol Int. 2022 Nov;39(11):1454-1464. doi: 10.1080/07420528.2022.2117051. Epub 2022 Aug 29. Chronobiol Int. 2022. PMID: 36036080
-
Prevalence and Risk Factors of Psychiatric Symptoms among Swiss Elite Athletes during the First Lockdown of the COVID-19 Pandemic.Int J Environ Res Public Health. 2021 Oct 14;18(20):10780. doi: 10.3390/ijerph182010780. Int J Environ Res Public Health. 2021. PMID: 34682521 Free PMC article.
-
Second Wave of COVID-19 Global Pandemic and Athletes' Confinement: Recommendations to Better Manage and Optimize the Modified Lifestyle.Int J Environ Res Public Health. 2020 Nov 12;17(22):8385. doi: 10.3390/ijerph17228385. Int J Environ Res Public Health. 2020. PMID: 33198389 Free PMC article. Review.
-
The Effect of the COVID-19 Pandemic on the Mental and Emotional Health of Athletes: A Systematic Review.Am J Sports Med. 2023 Jul;51(8):2207-2215. doi: 10.1177/03635465221087473. Epub 2022 Apr 12. Am J Sports Med. 2023. PMID: 35413208 Free PMC article.
Cited by
-
Lifestyle and eating habits before and during COVID-19 quarantine in Brazil.Public Health Nutr. 2022 Jan;25(1):65-75. doi: 10.1017/S136898002100255X. Epub 2021 Jun 10. Public Health Nutr. 2022. PMID: 34108067 Free PMC article.
-
Impact of the COVID-19 pandemic on the psychological aspects and mental health of elite soccer athletes: a systematic review.Front Psychol. 2024 Jan 25;14:1295652. doi: 10.3389/fpsyg.2023.1295652. eCollection 2023. Front Psychol. 2024. PMID: 38333426 Free PMC article.
-
Sleep health of Australian community tennis players during the COVID-19 lockdown.PeerJ. 2022 Apr 12;10:e13045. doi: 10.7717/peerj.13045. eCollection 2022. PeerJ. 2022. PMID: 35433127 Free PMC article.
-
Exploring the Perceived Impact of the COVID-19 Pandemic Social Distancing Measures on Athlete Wellbeing: A Qualitative Study Utilising Photo-Elicitation.Front Psychol. 2021 Jul 12;12:624023. doi: 10.3389/fpsyg.2021.624023. eCollection 2021. Front Psychol. 2021. PMID: 34322049 Free PMC article.
-
A Tale of Two Cities: COVID-19 and the Emotional Well-Being of Student-Athletes Using Natural Language Processing.Front Sports Act Living. 2021 Aug 25;3:710289. doi: 10.3389/fspor.2021.710289. eCollection 2021. Front Sports Act Living. 2021. PMID: 34514388 Free PMC article.
References
-
- Samuels C. Sleep, recovery, and performance: the new frontier in high-performance athletics. Phys Med Rehabil Clin N Am. 2009;20(1):149–59, ix. - PubMed
-
- Mujika I. Intense training: the key to optimal performance before and during the taper. Scand J Med Sci Spor. 2010; 20: 24–31. - PubMed
-
- Kuipers H. How much is too much? Performance aspects of overtraining. Res Q Exercise Sport. 1996; 67 (sup3): S-65–S-69. - PubMed
-
- Gabbett TJ, et al. . If overuse injury is a “training load error,” should undertraining be viewed the same way? Br J Sports Med. 2016; 50(17): 1017–1018. . - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

