Immunosuppressive Treatment in Antiphospholipid Syndrome: Is It Worth It?
- PMID: 33535377
- PMCID: PMC7911562
- DOI: 10.3390/biomedicines9020132
Immunosuppressive Treatment in Antiphospholipid Syndrome: Is It Worth It?
Abstract
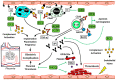
The antiphospholipid syndrome (APS) is characterized by the development of venous and/or arterial thrombosis and pregnancy morbidity in patients with persistent antiphospholipid antibodies (aPL). Catastrophic antiphospholipid syndrome (CAPS) is a life-threatening form of APS occurring in about 1% of cases. Lifelong anticoagulation with vitamin K antagonists remains the cornerstone of the therapy for thrombotic APS, but frequently the use of anticoagulation may be problematic due to the increased risk of bleeding, drug interactions, or comorbidities. Immunosuppressant drugs are widely used to treat several autoimmune conditions, in which their safety and effectiveness have been largely demonstrated. Similar evidence in the treatment of primary APS is limited to case reports or case series, and studies on a large scale lack. Immunomodulatory drugs may be an emerging tool in managing such particular situations, like refractory obstetrical complications, CAPS, or so-called APS non-criteria manifestations. In addition, immunomodulatory drugs may be useful in patients experiencing recurrent thromboembolic events despite optimized anticoagulant therapy. We did a comprehensive review of literature analyzing the possible role of immunomodulation in primary APS to provide a broad overview of potentially safe and effective target treatments for managing this devastating disease.
Keywords: anti-β2-glycoprotein I; anticardiolipin; antiphospholipid syndrome; catastrophic antiphospholipid syndrome; lupus anticoagulant.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Similar articles
-
Antiphospholipid Syndrome and Catastrophic Antiphospholipid Syndrome: A Comprehensive Review of Pathogenesis, Clinical Features, and Management Strategies.Cureus. 2024 Aug 10;16(8):e66555. doi: 10.7759/cureus.66555. eCollection 2024 Aug. Cureus. 2024. PMID: 39252716 Free PMC article. Review.
-
Intravenous immunoglobulins and antiphospholipid syndrome: How, when and why? A review of the literature.Autoimmun Rev. 2016 Mar;15(3):226-35. doi: 10.1016/j.autrev.2015.11.009. Epub 2015 Dec 1. Autoimmun Rev. 2016. PMID: 26656906 Review.
-
[Case series and clinical analysis of 14 cases of catastrophic antiphospholipid syndrome].Beijing Da Xue Xue Bao Yi Xue Ban. 2018 Dec 18;50(6):1033-1038. Beijing Da Xue Xue Bao Yi Xue Ban. 2018. PMID: 30562777 Chinese.
-
How I treat anticoagulant-refractory thrombotic antiphospholipid syndrome.Blood. 2021 Jan 21;137(3):299-309. doi: 10.1182/blood.2020004942. Blood. 2021. PMID: 32898856
-
The antiphospholipid syndrome: still an enigma.Hematology Am Soc Hematol Educ Program. 2015;2015:53-60. doi: 10.1182/asheducation-2015.1.53. Hematology Am Soc Hematol Educ Program. 2015. PMID: 26637701 Free PMC article. Review.
Cited by
-
Calcinosis Cutis and Calciphylaxis in Autoimmune Connective Tissue Diseases.Vaccines (Basel). 2023 Apr 25;11(5):898. doi: 10.3390/vaccines11050898. Vaccines (Basel). 2023. PMID: 37243003 Free PMC article. Review.
-
Biological therapy in systemic lupus erythematosus, antiphospholipid syndrome, and Sjögren's syndrome: evidence- and practice-based guidance.Front Immunol. 2023 Apr 17;14:1117699. doi: 10.3389/fimmu.2023.1117699. eCollection 2023. Front Immunol. 2023. PMID: 37138867 Free PMC article. Review.
-
Antiphospholipid syndrome, monoclonal gammopathy, and cryoglobulinemia overlap leading to recurrent cutaneous microvascular thrombosis: A case report and retrospective cohort study.EJHaem. 2024 Jul 28;5(5):971-975. doi: 10.1002/jha2.987. eCollection 2024 Oct. EJHaem. 2024. PMID: 39415921 Free PMC article.
-
Changes in Clinical Manifestations and Course of Systemic Lupus Erythematosus and Secondary Antiphospholipid Syndrome over Three Decades.Biomedicines. 2023 Apr 19;11(4):1218. doi: 10.3390/biomedicines11041218. Biomedicines. 2023. PMID: 37189836 Free PMC article.
-
Pulmonary Involvement in Systemic Lupus Erythematosus: A Potentially Overlooked Condition.Biomedicines. 2025 Jun 16;13(6):1485. doi: 10.3390/biomedicines13061485. Biomedicines. 2025. PMID: 40564204 Free PMC article. Review.
References
-
- Park S.H., Jang S., Park C.-J., Chi H.-S. Clinical Application of Revised Laboratory Classification Criteria for Antiphospholipid Antibody Syndrome: Is the Follow-Up Interval of 12 Weeks Instead of 6 Weeks Significantly Useful? BioMed Res. Int. 2016;2016:2641526. doi: 10.1155/2016/2641526. - DOI - PMC - PubMed
-
- Cervera R., Asherson R.A., Acevedo M.L., Gómez-Puerta J.A., Espinosa G., De La Red G., Gil V., Ramos-Casals M., García-Carrasco M., Ingelmo M., et al. Antiphospholipid syndrome associated with infections: Clinical and microbiological characteristics of 100 patients. Ann. Rheum. Dis. 2004;63:1312–1317. doi: 10.1136/ard.2003.014175. - DOI - PMC - PubMed
-
- Gómez-Puerta J.A., Cervera R., Aldea-Parés A., Aguiló S., Bucciarelli S., Ramos-Casals M., Ingelmo M., Asherson R.A., Font J. Antiphospholipid Antibodies Associated with Malignancies: Clinical and Pathological Characteristics of 120 Patients. Semin. Arthritis Rheum. 2006;35:322–332. doi: 10.1016/j.semarthrit.2005.07.003. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

