Is the Proportion of Patients with "Successful" Outcomes After Two-stage Revision for Prosthetic Joint Infection Different When Applying the Musculoskeletal Infection Society Outcome Reporting Tool Compared with the Delphi-based Consensus Criteria?
- PMID: 33543876
- PMCID: PMC8208431
- DOI: 10.1097/CORR.0000000000001654
Is the Proportion of Patients with "Successful" Outcomes After Two-stage Revision for Prosthetic Joint Infection Different When Applying the Musculoskeletal Infection Society Outcome Reporting Tool Compared with the Delphi-based Consensus Criteria?
Abstract
Background: There are a variety of criteria for defining successful treatment after two-stage exchange arthroplasty for prosthetic joint infection (PJI). To accurately assess current practices and improve techniques, it is important to first establish reliable, clinically relevant, reproducible criteria for defining persistent infection and "successful" outcomes.
Question/purpose: Is the proportion of patients considered to have successful management of PJI after two-stage resection arthroplasty smaller using 2019 Musculoskeletal Infection Society Outcome Reporting Tool (MSIS ORT) criteria than when using a Delphi-based criterion?
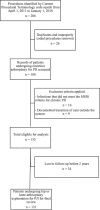
Methods: Patients were retrospectively identified by Current Procedural Technology codes for resection arthroplasty with placement of an antibiotic spacer for infected THA or TKA between April 1, 2011 and January 1, 2018 at a tertiary academic institution. The initial review identified 180 procedures during this time period. Nine patients had documented transition of care outside the system, 16 did not meet the MSIS criteria for chronic PJI, and 34 patients were excluded for lack of documented 2-year follow-up. The mean follow-up duration of the final cohort of 121 procedures in 120 patients was approximately 3.7 ± 1.7 years. Forty percent (49 of 121) of the procedures were performed on the hip and 60% (72 of 121) were performed on the knee. The mean time from primary THA or TKA to explantation was 4.6 years. The mean age of the patients at the time of explantation was 66 years. The mean time from spacer placement to replantation was 119 days. The final 121 patient records were reviewed by a single reviewer and outcomes were subsequently assigned to "successful" and "unsuccessful" outcomes based on the MSIS ORT and Delphi-based consensus criterion, two previously published and validated multidimensional definition schemes. Chi-squared and t-test analyses were performed to identify differences between "successful" and "unsuccessful" outcomes with respect to patient baseline characteristics using each outcome-reporting criterion.
Results: Overall, the MSIS ORT classified a smaller proportion of patients as having a "successful" treatment outcome after two-stage exchange arthroplasty for PJI than the Delphi-based consensus method did (MSIS: 55% [63 of 114], Delphi: 70% [71 of 102]; relative risk 0.79 [0.65-0.98]; p = 0.03). However, there were no differences when stratified by hips (MSIS: 55% [26 of 47], Delphi: 74% [29 of 39]; relative risk 0.74 [0.54-1.02]; p = 0.07) and knees (MSIS: 55% [37 of 67], Delphi: 67% [42 of 63]; relative risk 0.83 [0.63-1.09]; p = 0.19). Notably, the disease of 16% of the patients (19 of 121) was not classifiable per the Delphi method because these patients never underwent reimplantation.
Conclusion: The present study demonstrated that the MSIS criteria detect fewer instances of "successful" infection management after two-stage resection arthroplasty for PJI than the Delphi method in this cohort. Based on these findings, researchers and surgeons should aim for standardized reporting after intervention for PJI to allow for a better comparison of outcomes across different studies and ultimately allow for improved techniques and approaches to the treatment of PJI.
Level of evidence: Level III, diagnostic study.
Copyright © 2021 by the Association of Bone and Joint Surgeons.
Conflict of interest statement
Each author certifies that neither he nor she, nor any of his or her immediate family members, has funding or commercial associations (consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research® editors and board members are on file with the publication and can be viewed on request.
Figures


References
-
- Azzam KA, Seeley M, Ghanem E, Austin MS, Purtill JJ, Parvizi J. Irrigation and debridement in the management of prosthetic joint infection: traditional indications revisited. J Arthroplasty. 2010;25:1022-1027. - PubMed
-
- Bradbury T, Fehring TK, Taunton M, et al. The fate of acute methicillin-resistant Staphylococcus aureus periprosthetic knee infections treated by open debridement and retention of components. J Arthroplasty. 2009;24:101-104. - PubMed
-
- Cancienne JM, Granadillo VA, Patel KJ, Werner BC, Browne JA. Risk factors for repeat debridement, spacer retention, amputation, arthrodesis, and mortality after removal of an infected total knee arthroplasty with spacer placement. J Arthroplasty. 2018;33:515-520. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

