Comparison of clinical outcomes and spino-pelvic sagittal balance in degenerative lumbar spondylolisthesis: Minimally invasive oblique lumbar interbody fusion (OLIF) versus transforaminal lumbar interbody fusion (TLIF)
- PMID: 33545942
- PMCID: PMC7837863
- DOI: 10.1097/MD.0000000000023783
Comparison of clinical outcomes and spino-pelvic sagittal balance in degenerative lumbar spondylolisthesis: Minimally invasive oblique lumbar interbody fusion (OLIF) versus transforaminal lumbar interbody fusion (TLIF)
Abstract
Spino-pelvic sagittal parameters are closely related to the lumbar degenerative diseases. The present study aims to compare clinical results and spino-pelvic sagittal balance treated with oblique lumbar interbody fusion (OLIF) and transforaminal lumbar interbody fusion (TLIF) in patients with degenerative lumbar spondylolisthesis at single segment.We retrospectively reviewed and compared 28 patients who underwent OLIF (OLIF group) and 35 who underwent TLIF (TLIF group). Radiological results were evaluated with disc height (DH), foraminal height (FH), fused segment lordosis (FSL), lumbar lordosis (LL), pelvic tilt (PT), pelvic incidence (PI), and sacral slope (SS). Clinical results were evaluated with the Oswestry Disability Index (ODI) and VAS for back and leg pain.The OLIF group showed higher improvement of DH and FH than the TLIF group at all time points after surgery (P < .05). No significant differences were found in PT, PI, and SS between the 2 groups (P > .05). Significant restoration of spino-pelvic sagittal balance was observed in the 2 groups after surgery. Significant differences in postoperative lumbar lordosis and fused segment lordosis were found between the 2 groups (P < .05). Significant difference in the improvement of symptoms was observed between the 2 groups. The OLIF group had lower VAS scores for back pain and ODI compared after surgery (P < .05).It can be concluded that there are exactly differences in improvement of radiographic parameters between 2 approaches, which confirmed that OLIF is better in restoring spinal alignment. Besides, due to the unique minimally invasive approach, OLIF did exhibit a greater advantage in early recovery after surgery.
Copyright © 2021 the Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors have no funding and conflicts of interest to disclose.
Figures


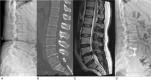
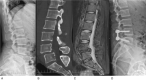
References
-
- Audat Z, Moutasem O, Yousef K. Comparison of clinical and radiological results of posterolateral fusion, posterior lumbar interbody fusion and transforaminal lumbar interbody fusion techniques in the treatment of degenerative lumbar spine. Singapore Med J 2012;53:183–7. - PubMed
-
- Chen YL, Zhu ZH, Wang YK, et al. Effects of oblique lateral interbody fusion and transforaminal lumbar interbody fusion for lordosis correction in degenerative lumbar diseases. Zhonghua Yi Xue Za Zhi 2018;98:1990–5. DOI 10.3760/cma.j.issn.0376-2491.2018.25.005. - PubMed
-
- Choi UY, Park JY, Kim KH, et al. Unilateral versus bilateral percutaneous pedicle screw fixation in minimally invasive transforaminal lumbar interbody fusion. Neurosurg Focus 2013;35:E11.DOI 10.3171/2013.2.FOCUS12398. - PubMed
-
- Cloward RB. The treatment of ruptured lumbar intervertebral discs by vertebral body fusion. I. Indications, operative technique, after care. J Neurosurg 1953;10:154–68. DOI 10.3171/jns.1953.10.2.0154. - PubMed
-
- Fujibayashi S, Hynes RA, Otsuki B, et al. Effect of indirect neural decompression through oblique lateral interbody fusion for degenerative lumbar disease. Spine 2015;40:E175–82. DOI 10.1097/BRS.0000000000000703. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

