Timing of corticosteroids impacts mortality in hospitalized COVID-19 patients
- PMID: 33547620
- PMCID: PMC7864133
- DOI: 10.1007/s11739-021-02655-6
Timing of corticosteroids impacts mortality in hospitalized COVID-19 patients
Abstract
The optimal timing of initiating corticosteroid treatment in hospitalized patients is unknown. We aimed to assess the relationship between timing of initial corticosteroid treatment and in-hospital mortality in COVID-19 patients. In this observational study through medical record analysis, we quantified the mortality benefit of corticosteroids in two equally matched groups of hospitalized COVID-19 patients. We subsequently evaluated the timing of initiating corticosteroids and its effect on mortality in all patients receiving corticosteroids. Demographic, clinical, and laboratory variables were collected and employed for multivariable regression analyses. 1461 hospitalized patients with confirmed COVID-19 were analyzed. Of these, 760 were also matched into two equal groups based on having received corticosteroid therapy. Patients receiving corticosteroids had a lower risk of death than those who did not (HR 0.67, 95% CI 0.67-0.90; p = 0.01). Timing of corticosteroids was assessed for all 615 patients receiving corticosteroids during admission. Patients receiving first dose of corticosteroids > 72 h into hospitalization had a lower risk of death compared to patients with first dose at earlier time intervals (HR 0.56, 95% CI 0.38-0.82; p = 0.003). There was a mortality benefit in patients with > 7 days of symptom onset to initiation of corticosteroids (HR 0.56, 95% CI 0.33-0.95; p = 0.03). In patients receiving oxygen therapy, corticosteroids reduced risk of death in mechanically ventilated patients (HR 0.38, 95% CI 0.24-0.60; p < 0.001) but not in patients on high-flow or other oxygen therapy (HR 0.46, 95% CI 0.20-1.07; p = 0.07) and (HR 0.84, 95% CI 0.35-2.00; p = 0.69), respectively. Timing of corticosteroids initiation was related to in-hospital mortality for COVID-19 patients. Time from symptom onset > 7 days should trigger initiation of corticosteroids. In the absence of invasive mechanical ventilation, corticosteroids should be initiated if the patient remains hospitalized at 72 h. Hypoxia requiring supplemental oxygen therapy should not be a trigger for initiation of corticosteroids unless the timing is appropriate.
Keywords: COVID-19; Coronavirus; Corticosteroids; Mortality; Timing; Treatment.
© 2021. Società Italiana di Medicina Interna (SIMI).
Conflict of interest statement
This manuscript in part or in full has not been submitted or published anywhere. No authors have any relevant conflict of interest disclosures.
Figures
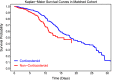


References
-
- Coronavirus disease (COVID-19). https://www.who.int/emergencies/diseases/novel-coronavirus-2019. Accessed 15 Oct 2020
-
- COVID-19 Map - Johns Hopkins Coronavirus Resource Center. https://coronavirus.jhu.edu/map.html. Accessed 15 Oct 2020
-
- Coronavirus Disease 2019 (COVID-19) | CDC. https://www.cdc.gov/coronavirus/2019-nCoV/index.html. Accessed 15 Oct 2020
-
- Q&A on coronaviruses (COVID-19). https://www.who.int/emergencies/diseases/novel-coronavirus-2019/question.... Accessed 15 Oct 2020
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

