Predictive factors for the medical hospitalisation of patients who visited the emergency department with suicide attempt
- PMID: 33549077
- PMCID: PMC7866662
- DOI: 10.1186/s12888-021-03089-2
Predictive factors for the medical hospitalisation of patients who visited the emergency department with suicide attempt
Abstract
Background: Suicide is a significant public health problem. Individuals are estimated to make up to 20 suicide attempts before suicide. The emergency department (ED) is the first location where individuals are brought after a suicide attempt. This study investigated the factors related to delays in the medical hospitalisation of patients who attempted suicide and aimed to provide criteria for hospitalisation decisions by physicians.
Methods: This study included patients who had deliberately self-harmed (age ≥ 19 years) and presented at the EDs of two tertiary teaching hospitals between March 2017 and April 2020. Those for whom relevant demographic and clinical information were unavailable and those admitted to the psychiatric wards were excluded.
Results: This study included 414 patients in the hospitalisation group and 1346 in the discharged group. The mean patient age was 50.3 ± 20.0 years and 40.7 ± 17.0 years in the hospitalised and discharged groups (p < 0.001), respectively. The mean ED length of stay (LOS) was 4.2 ± 12.3 and 11.4 ± 18.8 h in the hospitalised and discharged groups, respectively. In the hospitalised group, the odds ratio and confidence interval for aged 35 ~ 64 (2.222, 1.343-3.678), aged over 65 (2.788, 1.416-5.492), sex -male (2.041, 1.302-3.119), and consciousness (1.840, 1.253-2.466). The Risk-Rescue Ratio Scale (RRRS) was (1.298, 1.255-1.343). A receiver operating characteristics analysis of RRRS for the decision to hospitalise patients who attempted suicide showed a cut-off value of 42, with sensitivity, specificity, and area under the curve being 85.7, 85.5%, and 0.924, respectively.
Conclusion: The level of consciousness and the RRRS of patients who attempted suicide can be the factors to decide medical hospitalisation and reduce ED LOS and crowding.
Keywords: Emergency department; Hospitalisation; Length of stay; Suicide attempt.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
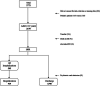

References
-
- World Health Statistics data visualizations dashboard [https://apps.who.int/gho/data/node.sdg.3-4-viz-2?lang=en] Accessed 4 June 2020.
-
- OECD data, Suicide rates [https://data.oecd.org/healthstat/suicide-rates.htm] Accessed 5 June 2020.
-
- Geulayov G, Casey D, McDonald KC, Foster P, Pritchard K, Wells C, Clements C, Kapur N, Ness J, Waters K, et al. Incidence of suicide, hospital-presenting non-fatal self-harm, and community-occurring non-fatal self-harm in adolescents in England (the iceberg model of self-harm): a retrospective study. Lancet Psychiatry. 2018;5(2):167–174. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

