Acute cholangitis in intensive care units: clinical, biological, microbiological spectrum and risk factors for mortality: a multicenter study
- PMID: 33549136
- PMCID: PMC7866656
- DOI: 10.1186/s13054-021-03480-1
Acute cholangitis in intensive care units: clinical, biological, microbiological spectrum and risk factors for mortality: a multicenter study
Abstract
Background: Little is known on the outcome and risk factors for mortality of patients admitted in Intensive Care units (ICUs) for Acute cholangitis (AC).
Methods: Retrospective multicenter study included adults admitted in eleven intensive care units for a proven AC from 2005 to 2018. Risk factors for in-hospital mortality were identified using multivariate analysis.
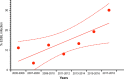
Results: Overall, 382 patients were included, in-hospital mortality was 29%. SOFA score at admission was 8 [5-11]. Biliary obstruction was mainly related to gallstone (53%) and cancer (22%). Median total bilirubin and PCT were respectively 83 µmol/L [50-147] and 19.1 µg/L [5.3-54.8]. Sixty-three percent of patients (n = 252) had positive blood culture, mainly Gram-negative bacilli (86%) and 14% produced extended spectrum beta lactamase bacteria. At ICU admission, persisting obstruction was frequent (79%) and biliary decompression was performed using therapeutic endoscopic retrograde cholangiopancreatography (76%) and percutaneous transhepatic biliary drainage (21%). Adjusted mortality significantly decreased overtime, adjusted OR for mortality per year was 0.72 [0.54-0.96] (p = 0.02). In a multivariate analysis, factors at admission associated with in-hospital mortality were: SOFA score (OR 1.14 [95% CI 1.05-1.24] by point, p = 0.001), lactate (OR 1.21 [95% CI 1.08-1.36], by 1 mmol/L, p < 0.001), total serum bilirubin (OR 1.26 [95% CI 1.12-1.41], by 50 μmol/L, p < 0.001), obstruction non-related to gallstones (p < 0.05) and AC complications (OR 2.74 [95% CI 1.45-5.17], p = 0.002). Time between ICU admission and biliary decompression > 48 h was associated with in-hospital mortality (adjusted OR 2.73 [95% CI 1.30-6.22], p = 0.02).
Conclusions: In this large retrospective multicenter study, we found that AC-associated mortality significantly decreased overtime. Severity of organ failure, cause of obstruction and local complications of AC are risk factors for mortality, as well as delayed biliary drainage > 48 h.
Keywords: Cholangitis; Intensive care unit; Microbiology; Outcome; Prognosis.
Conflict of interest statement
None.
Figures



References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

