A Sustainable Approach to Prepectoral Breast Reconstruction Using Meshed Acellular Dermal Matrix
- PMID: 33564601
- PMCID: PMC7861958
- DOI: 10.1097/GOX.0000000000003392
A Sustainable Approach to Prepectoral Breast Reconstruction Using Meshed Acellular Dermal Matrix
Abstract
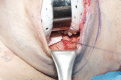
Background: Prepectoral implant-based breast reconstruction provides an alternative to submuscular reconstruction, but the increased acellular dermal matrix (ADM) required has the potential to lead to increased costs and decreased supply of this limited-resource material. We present a method for prepectoral reconstruction utilizing skin-graft meshing techniques to increase the surface area of usable ADM.
Methods: Forty-four patients underwent this technique from February 2019 to February 2020. Patient characteristics, operative details, and outcomes, including complications and patient satisfaction utilizing the BREAST-Q, were analyzed. Cost analysis relative to projected cost of nonmeshed techniques was performed.
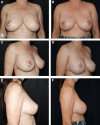
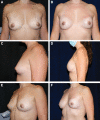
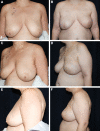
Results: There were 20 unilateral and 24 bilateral procedures, for a total of 68 breast reconstructions. Mean age was 45.9 years (32-71). Mean implant volume was 485 cm3 (265-800), and one sheet of ADM was used for each breast with an average surface area of 161 cm2. Median follow-up was 350 days (212-576). Minor complications included an infection treated with oral antibiotics. Major complications included one axillary hematoma and one delayed implant loss. One patient underwent revision for asymmetry. Mean BREAST-Q score was 47.4/60. Cost ranged from $4113 to 5025 per breast, compared with the projected $9125-18250 per breast for other techniques in the literature.
Conclusions: In contrast to previously described uses of ADM in prepectoral reconstruction, meshing maximizes resource utilization by expanding the coverage of a single sheet. Early findings demonstrate minimal complications and high patient satisfaction, suggesting the approach has potential to provide the benefits of prepectoral reconstruction while responsibly preserving product availability and tempering healthcare costs.
Copyright © 2021 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of The American Society of Plastic Surgeons.
Conflict of interest statement
Disclosure: The authors have no financial interest to declare in relation to the content of this article.
Figures



References
-
- Gabriel A, Sigalove S, Sigalove NM, et al. Prepectoral revision breast reconstruction for treatment of implant-associated animation deformity: a review of 102 reconstructions. Aesthet Surg J. 2018;38:519–526. - PubMed
-
- Sigalove S, Maxwell GP, Sigalove NM, et al. Prepectoral implant-based breast reconstruction: rationale, indications, and preliminary results. Plast Reconstr Surg. 2017;139:287–294. - PubMed
-
- Antony AK, Poirier J, Madrigrano A, et al. Evolution of the surgical technique for “breast in a day” direct-to-implant breast reconstruction: transitioning from dual-plane to prepectoral implant placement. Plast Reconstr Surg. 2019;143:1547–1556. - PubMed
-
- Sbitany H, Piper M, Lentz R. Prepectoral breast reconstruction: a safe alternative to submuscular prosthetic reconstruction following nipple-sparing mastectomy. Plast Reconstr Surg. 2017;140:432–443. - PubMed
-
- Vidya R, Iqbal FM. A guide to prepectoral breast reconstruction: a new dimension to implant-based breast reconstruction. Clin Breast Cancer. 2017;17:266–271. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
