The association of parameters of body composition and laboratory markers with the severity of hypertriglyceridemia-induced pancreatitis
- PMID: 33573658
- PMCID: PMC7879630
- DOI: 10.1186/s12944-021-01443-7
The association of parameters of body composition and laboratory markers with the severity of hypertriglyceridemia-induced pancreatitis
Abstract
Background: Hypertriglyceridemia has arisen as the third leading cause of acute pancreatitis. This study aimed at exploring the association between the severity of hypertriglyceridemia-induced pancreatitis (HTGP) and computed tomography (CT)-based body composition parameters and laboratory markers.
Methods: Laboratory and clinical parameters were collected from 242 patients with HTGP between 2017 and 2020. Severity of HTGP was evaluated by original or modified CT severity index. Body composition parameters such as area and radiodensity of muscle, subcutaneous adipose tissue and visceral adipose tissue were calculated by CT at the level of third lumbar vertebra. Parameters were compared between mild and moderately severe to severe HTGP. Uni-variate and multi-variate Logistic regression analyses were employed to assess the risk factors of the severity of HTGP.
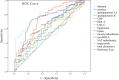
Results: Seventy patients (28.9%) presented with mild HTGP. Body mass index, waist circumference and all CT-based body composition parameters differed between male and female patients. None was associated with the severity of HTGP, neither in males nor in females. Receiver operating characteristic curves showed that areas under the curves of apolipoprotein A-I and albumin to predict the severity of HTGP were 0.786 and 0.759, respectively (all P < 0.001). Uni-variate and further multi-variate Logistic regression analysis confirmed that low serum albumin (< 35 g/L, P = 0.004, OR = 3.362, 95%CI = 1.492-8.823) and apolipoprotein A-I (< 1.1 g/L, P < 0.001, OR = 5.126, 95%CI = 2.348-11.195), as well as high C-reactive protein (> 90 mg/L, P = 0.005, OR = 3.061, 95%CI = 1.407-6.659) and lipase (P = 0.033, OR = 2.283, 95%CI = 1.070-4.873) were risk factors of moderately severe to severe HTGP. Levels of albumin, apolipoprotein A-I, C-reactive protein and lipase were also associated with the length of hospital stay (all P < 0.05). Besides, low serum albumin, low-density lipoprotein cholesterol and high radiodensity of subcutaneous adipose tissue were significant risk factors of pancreatic necrosis in patients with HTGP (all P < 0.05).
Conclusions: Low serum albumin and apolipoprotein A-I, and high C-reactive protein and lipase upon admission were associated with a more severe type of HTGP and longer hospital stay for these patients. Albumin and apolipoprotein A-I may serve as novel biomarkers for the severity of HTGP. However, none of the body composition parameters was associated with the severity of HTGP.
Keywords: Albumin; Apolipoprotein A-I; Body composition; Computed tomography; Hypertriglyceridemia-induced pancreatitis; Pancreatic necrosis; Severity.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
The modified computed tomography severity index combined with low skeletal muscle mass can better predict the severity of hypertriglyceridemia-induced pancreatitis.J Hepatobiliary Pancreat Sci. 2022 Dec;29(12):1336-1345. doi: 10.1002/jhbp.1198. Epub 2022 Jun 23. J Hepatobiliary Pancreat Sci. 2022. PMID: 35687043
-
Factors associated with the severity of hypertriglyceridemia induced acute pancreatitis.Medicine (Baltimore). 2021 May 28;100(21):e25983. doi: 10.1097/MD.0000000000025983. Medicine (Baltimore). 2021. PMID: 34032712 Free PMC article.
-
Low Serum Ionized Calcium, Elevated High-Sensitivity C-Reactive Protein, Neutrophil-Lymphocyte Ratio, and Body Mass Index (BMI) Are Risk Factors for Severe Acute Pancreatitis in Patients with Hypertriglyceridemia Pancreatitis.Med Sci Monit. 2019 Aug 15;25:6097-6103. doi: 10.12659/MSM.915526. Med Sci Monit. 2019. PMID: 31413252 Free PMC article.
-
[Hypertriglyceridemia-induced pancreatitis].Nihon Rinsho. 2013 Sep;71(9):1602-5. Nihon Rinsho. 2013. PMID: 24205721 Review. Japanese.
-
Hypertriglyceridemia-induced pancreatitis: updated review of current treatment and preventive strategies.Clin J Gastroenterol. 2018 Dec;11(6):441-448. doi: 10.1007/s12328-018-0881-1. Epub 2018 Jun 19. Clin J Gastroenterol. 2018. PMID: 29923163 Review.
Cited by
-
Impacts of body composition parameters and liver cirrhosis on the severity of alcoholic acute pancreatitis.PLoS One. 2021 Nov 22;16(11):e0260309. doi: 10.1371/journal.pone.0260309. eCollection 2021. PLoS One. 2021. PMID: 34807958 Free PMC article.
-
Automated Machine Learning for the Early Prediction of the Severity of Acute Pancreatitis in Hospitals.Front Cell Infect Microbiol. 2022 Jun 10;12:886935. doi: 10.3389/fcimb.2022.886935. eCollection 2022. Front Cell Infect Microbiol. 2022. PMID: 35755847 Free PMC article.
-
Analysis of the clinical profile and treatment efficiency of hyperlipidemic acute pancreatitis.Lipids Health Dis. 2024 Mar 8;23(1):70. doi: 10.1186/s12944-024-02057-5. Lipids Health Dis. 2024. PMID: 38459563 Free PMC article.
-
A systematic review of the epidemiology and risk factors for severity and recurrence of hypertriglyceridemia-induced acute pancreatitis.BMC Gastroenterol. 2025 May 15;25(1):374. doi: 10.1186/s12876-025-03954-4. BMC Gastroenterol. 2025. PMID: 40375154 Free PMC article.
-
The challenge of prognostic markers in acute pancreatitis: internist's point of view.J Genet Eng Biotechnol. 2021 May 25;19(1):77. doi: 10.1186/s43141-021-00178-3. J Genet Eng Biotechnol. 2021. PMID: 34036463 Free PMC article.
References
-
- Pothoulakis I, Paragomi P, Archibugi L, Tuft M, Talukdar R, Kochhar R, et al. Clinical features of hypertriglyceridemia-induced acute pancreatitis in an international, multicenter, prospective cohort (APPRENTICE consortium) Pancreatology. 2020;20:325–330. doi: 10.1016/j.pan.2020.02.010. - DOI - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

