Incidence and real-world burden of brain metastases from solid tumors and hematologic malignancies in Ontario: a population-based study
- PMID: 33585818
- PMCID: PMC7872008
- DOI: 10.1093/noajnl/vdaa178
Incidence and real-world burden of brain metastases from solid tumors and hematologic malignancies in Ontario: a population-based study
Abstract
Background: Although intracranial metastatic disease (IMD) is a frequent complication of cancer, most cancer registries do not capture these cases. Consequently, a data-gap exists, which thwarts system-level quality improvement efforts. The purpose of this investigation was to determine the real-world burden of IMD.
Methods: Patients diagnosed with a non-CNS cancer between 2010 and 2018 were identified from the Ontario Cancer Registry. IMD was identified by scanning hospital administrative databases for cranial irradiation or coding for a secondary brain malignancy (ICD-10 code C793).
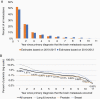
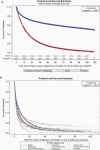
Results: 25,478 of 601,678 (4.2%) patients with a diagnosis of primary cancer were found to have IMD. The median time from primary cancer diagnosis to IMD was 5.2 (0.7, 15.4) months and varied across disease sites, for example, 2.1 months for lung, 7.3 months for kidney, and 22.8 months for breast. Median survival following diagnosis with IMD was 3.7 months. Lung cancer accounted for 60% of all brain metastases, followed by breast cancer (11%) and melanoma (6%). More advanced stage at diagnosis and younger age were associated with a higher likelihood of developing IMD (P < .0001). IMD was also associated with triple-negative breast cancers and ductal histology (P < .001), and with small-cell histology in patients with lung cancer (P < .0001). The annual incidence of IMD was 3,520, translating to 24.2 per 100,000 persons.
Conclusion: IMD represents a significant burden in patients with systemic cancers and is a significant cause of cancer mortality. Our findings support measures to actively capture incidents of brain metastasis in cancer registries.
Keywords: brain imaging; brain metastases; incidence; intracranial metastatic disease.
© The Author(s) 2020. Published by Oxford University Press, the Society for Neuro-Oncology and the European Association of Neuro-Oncology.
Figures



References
-
- Lu-Emerson C, Eichler AF. Brain metastases. Continuum (Minneap Minn). 2012;18(2):295–311. - PubMed
-
- Tabouret E, Chinot O, Metellus P, Tallet A, Viens P, Gonçalves A. Recent trends in epidemiology of brain metastases: an overview. Anticancer Res. 2012;32(11):4655–4662. - PubMed
-
- Gavrilovic IT, Posner JB. Brain metastases: epidemiology and pathophysiology. J Neurooncol. 2005;75(1):5–14. - PubMed
-
- Fox BD, Cheung VJ, Patel AJ, Suki D, Rao G. Epidemiology of metastatic brain tumors. Neurosurg Clin N Am. 2011;22(1):1–6, v. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
