Five-Year Survival Outcomes of Hybrid Minimally Invasive Esophagectomy in Esophageal Cancer: Results of the MIRO Randomized Clinical Trial
- PMID: 33595631
- PMCID: PMC7890455
- DOI: 10.1001/jamasurg.2020.7081
Five-Year Survival Outcomes of Hybrid Minimally Invasive Esophagectomy in Esophageal Cancer: Results of the MIRO Randomized Clinical Trial
Abstract
Importance: Available data comparing the long-term results of hybrid minimally invasive esophagectomy (HMIE) with that of open esophagectomy are conflicting, with similar or even better results reported for the minimally invasive esophagectomy group.
Objective: To evaluate the long-term, 5-year outcomes of HMIE vs open esophagectomy, including overall survival (OS), disease-free survival (DFS), and pattern of disease recurrence, and the potential risk factors associated with these outcomes.
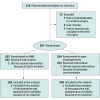
Design, setting, and participants: This randomized clinical trial is a post hoc follow-up study that analyzes the results of the open-label Multicentre Randomized Controlled Phase III Trial, which enrolled patients from 13 different centers in France and was conducted from October 26, 2009, to April 4, 2012. Eligible patients were 18 to 75 years of age and were diagnosed with resectable cancer of the middle or lower third of the esophagus. After exclusions, patients were randomized to either the HMIE group or the open esophagectomy group. Data analysis was performed on an intention-to-treat basis from November 19, 2019, to December 4, 2020.
Interventions: Hybrid minimally invasive esophagectomy (laparoscopic gastric mobilization with open right thoracotomy) was compared with open esophagectomy.
Main outcomes and measures: The primary end points of this follow-up study were 5-year OS and DFS. The secondary end points were the site of disease recurrence and potential risk factors associated with DFS and OS.
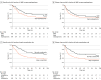
Results: A total of 207 patients were randomized, of whom 175 were men (85%), and the median (range) age was 61 (23-78) years. The median follow-up duration was 58.2 (95% CI, 56.5-63.8) months. The 5-year OS was 59% (95% CI, 48%-68%) in the HMIE group and 47% (95% CI, 37%-57%) in the open esophagectomy group (hazard ratio [HR], 0.71; 95% CI, 0.48-1.06). The 5-year DFS was 52% (95% CI, 42%-61%) in the HMIE group vs 44% (95% CI, 34%-53%) in the open esophagectomy group (HR, 0.81; 95% CI, 0.55-1.17). No statistically significant difference in recurrence rate or location was found between groups. In a multivariable analysis, major intraoperative and postoperative complications (HR, 2.21; 95% CI, 1.41-3.45; P < .001) and major pulmonary complications (HR, 1.94; 95% CI, 1.21-3.10; P = .005) were identified as risk factors associated with decreased OS. Similarly, multivariable analysis of DFS identified overall intraoperative and postoperative complications (HR, 1.93; 95% CI, 1.28-2.90; P = .002) and major pulmonary complications (HR, 1.85; 95% CI, 1.19-2.86; P = .006) as risk factors.
Conclusions and relevance: This study found no difference in long-term survival between the HMIE and open esophagectomy groups. Major postoperative overall complications and pulmonary complications appeared to be independent risk factors in decreased OS and DFS, providing additional evidence that HMIE may be associated with improved oncological results compared with open esophagectomy primarily because of a reduction in postoperative complications.
Trial registration: ClinicalTrials.gov Identifier: NCT00937456.
Conflict of interest statement
Figures
Comment in
-
True, True, and Unrelated-Complications and Survival After Hybrid Minimally Invasive Esophagectomy.JAMA Surg. 2021 Apr 1;156(4):332-333. doi: 10.1001/jamasurg.2020.7082. JAMA Surg. 2021. PMID: 33595626 No abstract available.
References
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous