Application of Polydioxanone Sutures in the Nuss Procedure
- PMID: 33601470
- PMCID: PMC8828300
- DOI: 10.1055/s-0041-1723847
Application of Polydioxanone Sutures in the Nuss Procedure
Abstract
Background/purpose: The Nuss procedure is the most common surgical repair for pectus excavatum (PE). Surgical steel wires are used in some modifications of the Nuss procedure to attach one or both ends of a support bar to the ribs. During follow-up, wire breakage was found in some cases. Patients with wire breakage may undergo prolonged bar removal surgery and may be exposed to excessive radiation.In this study, we had a series of patients who received polydioxanone suture (PDS) fixations instead of steel wires. This retrospective study was conducted to explore the differences between these two fixation materials in the incidence of related complications and efficacies. Furthermore, we attempted to observe whether the two materials lead to similar surgical efficacy in the Nuss procedure, whether they have divergent effects on the bar removal surgery, and whether PDS can reduce the risks due to steel wire breakage as expected.
Methods: We retrospectively studied PDS and surgical steel wires as fixation materials for the Nuss procedure in children with congenital PE and reviewed the outcomes and complications. A total of 75 children who had undergone Nuss procedure repairs and bar removals from January 2013 to December 2019 were recruited to participate in this study. They were divided into three groups: the PDS group, the unbroken wire (UBW) group, and the broken wire (BW) group, according to the fixation materials and whether the wires had broken or not. Moreover, we selected the duration of operation (DO), intraoperative blood loss (BL), bar displacement (BD), postoperative pain score (PPS), and incision infection as the risk indicators and the postrepair Haller index (HI) as the effectiveness indicator. These indicators were statistically compared to determine whether there were differences among the three groups.
Results: One BD occurred in the PDS and BW groups while none took place in the UBW group. No incision infection was found in any of the groups. The PDS group had the shortest DO, while the DO in the UBW group was shorter than that in the BW group (p < 0.05). BL in the PDS group was less than that in the other two groups (p < 0.05). Additionally, no difference was observed in BL between the BW and UBW groups (p > 0.05). The PPS of the PDS group was less than that of the BW group (p < 0.05), whereas no differences were found between the other two groups. No statistical difference emerged in HI among the groups (p > 0.05).
Conclusion: PDS fixation results in a similar repair outcome and shows certain advantages in the DO, BL, and PPS; also, PDSs are safe and effective in the Nuss procedure.
Level of evidence: Level III.
The Author(s). This is an open access article published by Thieme under the terms of the Creative Commons Attribution-NonDerivative-NonCommercial License, permitting copying and reproduction so long as the original work is given appropriate credit. Contents may not be used for commercial purposes, or adapted, remixed, transformed or built upon. (https://creativecommons.org/licenses/by-nc-nd/4.0/).
Conflict of interest statement
None declared.
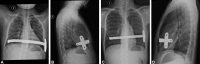
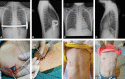
Figures
Similar articles
-
Wire fracture in postoperative Nuss procedure: a problem that cannot be ignored.Transl Pediatr. 2021 Mar;10(3):569-578. doi: 10.21037/tp-20-354. Transl Pediatr. 2021. PMID: 33850815 Free PMC article.
-
Different Nuss procedures and risk management for pectus excavatum after surgery for congenital heart disease.J Pediatr Surg. 2018 Oct;53(10):1964-1969. doi: 10.1016/j.jpedsurg.2018.04.006. Epub 2018 Apr 7. J Pediatr Surg. 2018. PMID: 29716732
-
Experience in 100 cases with the Nuss procedure using a technique for stabilization of the pectus bar.Pediatr Surg Int. 2003 May;19(3):186-9. doi: 10.1007/s00383-002-0915-z. Epub 2003 May 27. Pediatr Surg Int. 2003. PMID: 12768312
-
Recent experiences with minimally invasive pectus excavatum repair "Nuss procedure".Jpn J Thorac Cardiovasc Surg. 2005 Jul;53(7):338-44. doi: 10.1007/s11748-005-0047-1. Jpn J Thorac Cardiovasc Surg. 2005. PMID: 16095232
-
Novel techniques and future developments in minimally invasive pectus repair.J Thorac Dis. 2024 Jul 30;16(7):4807-4815. doi: 10.21037/jtd-23-1676. Epub 2024 Jul 11. J Thorac Dis. 2024. PMID: 39144309 Free PMC article. Review.
Cited by
-
Advancements in Wearable and Implantable BioMEMS Devices: Transforming Healthcare Through Technology.Micromachines (Basel). 2025 Apr 28;16(5):522. doi: 10.3390/mi16050522. Micromachines (Basel). 2025. PMID: 40428648 Free PMC article. Review.
-
A modified suture technique using polydioxanone (PDS II) for capsule closure in total knee arthroplasty: a prospective randomized study compared with traditional suture technique.Arch Orthop Trauma Surg. 2025 Jan 7;145(1):116. doi: 10.1007/s00402-024-05677-9. Arch Orthop Trauma Surg. 2025. PMID: 39775126 Free PMC article. Clinical Trial.
References
-
- Nuss D, Kelly R E, Jr, Croitoru D P, Katz M E. A 10-year review of a minimally invasive technique for the correction of pectus excavatum. J Pediatr Surg. 1998;33(04):545–552. - PubMed
-
- Bodenstein L, Notrica D M. Use of a capture-guidance surgical instrument to minimize muscle stripping during Nuss repair of pectus excavatum. J Laparoendosc Adv Surg Tech A. 2019;29(06):865–868. - PubMed
-
- de Campos J R, Das-Neves-Pereira J C, Lopes K M, Jatene F B. Technical modifications in stabilisers and in bar removal in the Nuss procedure. Eur J Cardiothorac Surg. 2009;36(02):410–412. - PubMed
-
- Li G, Jiang Z, Xiao H. A novel modified Nuss procedure for pectus excavatum: a new steel bar. Ann Thorac Surg. 2015;99(05):1788–1792. - PubMed
-
- Wong D L, Baker C M. Pain in children: comparison of assessment scales. Pediatr Nurs. 1988;14(01):9–17. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

