Clinical outcomes of bulky parotid gland cancers: need for self-examination and screening program for early diagnosis of parotid tumors
- PMID: 33602169
- PMCID: PMC7890841
- DOI: 10.1186/s12885-021-07902-9
Clinical outcomes of bulky parotid gland cancers: need for self-examination and screening program for early diagnosis of parotid tumors
Abstract
Background: Early detection and diagnosis of parotid gland cancer (PGC) are essential to improve clinical outcomes, because Tumor-Node-Metastasis stage at diagnosis is a very strong indicator of prognosis in PGC. Nevertheless, some patients still present with large parotid mass, maybe due to the unawareness or ignorance of their disease. In this study, we aimed to present the clinical outcomes of bulky PGC (defined by a 4 cm cutoff point for T3-4 versus T1-2 tumors), to emphasize the necessity of a self-examination tool for parotid gland tumor.
Methods: We retrospectively reviewed 60 consecutive cases with bulky (equal to and greater than 4 cm in the longest diameter, determined radiologically) malignant tumors arising from the parotid gland from 1995 to 2016. The clinical and pathological factors were analyzed to identify risk factors for poor outcomes using Cox proportional hazard models. In addition, we designed a self-examination tool for parotid gland tumors, similar to breast self-examination for breast cancer detection.
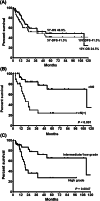
Results: Patients with bulky parotid cancer showed 48.9% 5-year and 24.5% 10-year overall survival rates and a 47.9% risk of high-grade malignancy. The common pathological diagnoses were carcinoma ex pleomorphic adenoma (18.3%), adenocarcinoma (16.7%), mucoepidermoid carcinoma (16.7%), salivary duct carcinoma (16.7%), and adenoid cystic carcinoma (11.7%). Survival analyses revealed that tumor size (hazard ratio, HR = 1.262 upon increase of 1 cm, 95% confidence interval, 95%CI 1.059-1.502), lymph node metastasis (HR = 2.999, 95%CI 1.048-8.583), and high tumor grade (HR = 4.148, 95%CI 1.215-14.154) were independent prognostic factors in multivariable analysis. Functional preservation of the facial nerve was possible only in less than half of patients.
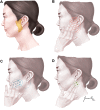
Conclusion: In bulky PGC, lymph node metastasis at diagnosis and high tumor grade indicated poor survival outcomes, and functional outcomes of the facial nerve were suboptimal. Thus, a public effort seems to be necessary to decrease these patients with bulky PGC, and to increase patients' self-awareness of their disease. As a way of early detection, we proposed a parotid self-examination tool to detect parotid gland tumors at an early stage, which is similar to breast self-examination.
Keywords: Advanced stage, prognosis; Parotid gland; Surgery; Tumor.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

Similar articles
-
Patterns of lymph node metastasis of parotid cancer.Auris Nasus Larynx. 2016 Aug;43(4):446-50. doi: 10.1016/j.anl.2015.11.002. Epub 2015 Dec 4. Auris Nasus Larynx. 2016. PMID: 26656731
-
Malignant parotid tumors: natural history and treatment.Cancer. 1977 Jul;40(1):136-44. doi: 10.1002/1097-0142(197707)40:1<136::aid-cncr2820400123>3.0.co;2-a. Cancer. 1977. PMID: 195701
-
The number and ratio of positive lymph nodes are independent prognostic factors for patients with major salivary gland cancer: Results from the surveillance, epidemiology, and End Results dataset.Eur J Surg Oncol. 2019 Jun;45(6):1025-1032. doi: 10.1016/j.ejso.2018.11.008. Epub 2018 Nov 15. Eur J Surg Oncol. 2019. PMID: 30472214
-
Salivary gland tumors in children: a retrospective clinical review.Pediatr Hematol Oncol. 2014 Nov;31(8):681-6. doi: 10.3109/08880018.2014.942936. Epub 2014 Sep 23. Pediatr Hematol Oncol. 2014. PMID: 25247345 Review.
-
Distant metastasis of parotid gland tumors.Acta Otolaryngol. 2006 Apr;126(4):340-5. doi: 10.1080/00016480500401035. Acta Otolaryngol. 2006. PMID: 16608783 Review.
Cited by
-
Comparison of Different Machine Models Based on Multi-Phase Computed Tomography Radiomic Analysis to Differentiate Parotid Basal Cell Adenoma From Pleomorphic Adenoma.Front Oncol. 2022 Jul 12;12:889833. doi: 10.3389/fonc.2022.889833. eCollection 2022. Front Oncol. 2022. PMID: 35903689 Free PMC article.
-
Diagnostic accuracy of ultrasound and MRI in parotid gland tumors: A retrospective study.Exp Ther Med. 2025 Jul 8;30(3):170. doi: 10.3892/etm.2025.12920. eCollection 2025 Sep. Exp Ther Med. 2025. PMID: 40692766 Free PMC article.
-
Deep learning-assisted diagnosis of benign and malignant parotid gland tumors based on automatic segmentation of ultrasound images: a multicenter retrospective study.Front Oncol. 2024 Aug 9;14:1417330. doi: 10.3389/fonc.2024.1417330. eCollection 2024. Front Oncol. 2024. PMID: 39184051 Free PMC article.
-
Pre-treatment quality of life in patients with salivary gland cancer in comparison with those of head and neck cancer patients.Qual Life Res. 2023 May;32(5):1493-1506. doi: 10.1007/s11136-022-03323-8. Epub 2022 Dec 13. Qual Life Res. 2023. PMID: 36512301
-
Quantitative Analysis and Pathological Basis of Signal Intensity on T2-Weighted MR Images in Benign and Malignant Parotid Tumors.Cancer Manag Res. 2021 Jul 7;13:5423-5431. doi: 10.2147/CMAR.S319466. eCollection 2021. Cancer Manag Res. 2021. PMID: 34262350 Free PMC article.
References
-
- Jang JY, Choi N, Ko YH, Chung MK, Son YI, Baek CH, et al. Treatment outcomes in metastatic and localized high-grade salivary gland cancer: high chance of cure with surgery and post-operative radiation in T1-2 N0 high-grade salivary gland cancer. BMC Cancer. 2018;18(1):672. doi: 10.1186/s12885-018-4578-0. - DOI - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

