Outcomes of Operator-Directed Sedation and Anesthesiologist Care in the Pediatric/Congenital Catheterization Laboratory: A Study Utilizing Data From the IMPACT Registry
- PMID: 33602437
- PMCID: PMC7932684
- DOI: 10.1016/j.jcin.2020.10.054
Outcomes of Operator-Directed Sedation and Anesthesiologist Care in the Pediatric/Congenital Catheterization Laboratory: A Study Utilizing Data From the IMPACT Registry
Abstract
Objectives: The objective of this study was to assess contemporary use of operator directed sedation (ODS) and anesthesiologist care (AC) in the pediatric/congenital cardiac catheterization laboratory (PCCL), specifically evaluating whether the use of operator-directed sedation was associated with increased risk of major adverse events.
Background: The safety of ODS relative to AC during PCCL procedures has been questioned.
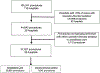
Methods: A multicenter, retrospective cohort study was performed studying procedures habitually performed with ODS or AC at IMPACT (Improving Adult and Congenital Treatment) registry hospitals using ODS for ≥5% of cases. The risks for major adverse events (MAE) for ODS and AC cases were compared, adjusted for case mix. Current recommendations were evaluated by comparing the ratio of observed to expected MAE for cases in which ODS was inappropriate (inconsistent with those guidelines) with those for similar risk AC cases, as well as those in which ODS or AC was appropriate.
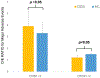
Results: Of the hospitals submitting data to IMPACT, 28 of 101 met inclusion criteria. Of the 7,042 cases performed using ODS at these centers, 88% would be inappropriate. Use of ODS was associated with lower likelihood of MAE both in observed results (p < 0.0001) and after adjusting for case-mix (odds ratio: 0.81; p = 0.006). Use of AC was also associated with longer adjusted fluoroscopy and procedure times (p < 0.0001 for both). The observed/expected ratio for ODS cases with high pre-procedural risk (inappropriate for ODS) was significantly lower than that for AC cases with comparable pre-procedural risk. Across a range of pre-procedural risks, there was no stratum in which risk for MAE was lower for AC than ODS.
Conclusions: Across a range of hospitals, ODS was used safely and with improved efficiency. Clinical judgment better identified cases in which ODS could be used than pre-procedural risk score. This should inform future guidelines for the use of ODS and AC in the catheterization laboratory.
Keywords: congenital heart disease; health services research; outcomes research; pediatrics.
Copyright © 2021 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Funding Support and Author Disclosures Dr. O’Byrne has received research support from the National Institutes of Health/National Heart, Lung, and Blood Institute (grant K23 HL130420-01). Dr. Hill has received research support from the National Centers for Advancing Translational Sciences (grant U01TR-001803-01). Dr. Chamberlain is supported by the National Institute of General Medical Sciences and the Eunice Kennedy Shriver National Institute of Child Health and Human Development of the National Institutes of Health (grant T32GM086330). The specific study was supported by the American College of Cardiology Foundation. It was reviewed by the IMPACT registry research and publications committee during its planning, as was the resulting manuscript. However, the funding agencies had no role in the planning or execution of the study, nor did they edit the paper as presented. The paper represents the opinions of the authors alone. All other authors have reported that they have no relationships relevant to the contents of this paper to disclose.
Figures



Comment in
-
Operator-Directed Sedation in the Pediatric Cardiac Catheterization Laboratory: "The Wheel Has Come Full Circle".JACC Cardiovasc Interv. 2021 Feb 22;14(4):414-416. doi: 10.1016/j.jcin.2020.11.023. JACC Cardiovasc Interv. 2021. PMID: 33602438 No abstract available.
-
What Is the Real IMPACT of an Acronym?JACC Cardiovasc Interv. 2021 Apr 26;14(8):928-929. doi: 10.1016/j.jcin.2021.03.020. JACC Cardiovasc Interv. 2021. PMID: 33888240 No abstract available.
References
-
- Vincent RN, Moore J, Beekman RH, et al. Procedural characteristics and adverse events in diagnostic and interventional catheterisations in paediatric and adult CHD: initial report from the IMPACT Registry. Cardiology in the Young 2016;26:70–78. - PubMed
-
- Moore JW, Vincent RN, Beekman RH, et al. Procedural results and safety of common interventional procedures in congenital heart disease: initial report from the National Cardiovascular Data Registry. J Am Coll Cardiol 2014;64:2439–2451. - PubMed
-
- Lin CH, Desai S, Nicolas R, et al. Sedation and Anesthesia in Pediatric and Congenital Cardiac Catheterization: A Prospective Multicenter Experience. Pediatr Cardiol 2015;36:1363–1375. - PubMed
-
- Odegard KC, Vincent R, Baijal R, et al. SCAI/CCAS/SPA expert consensus statement for anesthesia and sedation practice: Recommendations for patients undergoing diagnostic and therapeutic procedures in the pediatric and congenital cardiac catheterization laboratory. 2016;88:912–922. - PubMed
-
- Nykanen DG, Forbes TJ, Du W, et al. CRISP: Catheterization RISk score for pediatrics: A Report from the Congenital Cardiac Interventional Study Consortium (CCISC). Cathet. Cardiovasc. Intervent 2015. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

