Association of Serum Aldosterone and Plasma Renin Activity With Ambulatory Blood Pressure in African Americans: The Jackson Heart Study
- PMID: 33605160
- PMCID: PMC8789344
- DOI: 10.1161/CIRCULATIONAHA.120.050896
Association of Serum Aldosterone and Plasma Renin Activity With Ambulatory Blood Pressure in African Americans: The Jackson Heart Study
Abstract
Background: The renin-angiotensin-aldosterone system (RAAS) is an important driver of blood pressure (BP), but the association of the RAAS with ambulatory BP (ABP) and ABP monitoring phenotypes among African Americans has not been assessed.
Methods: ABP and ABP monitoring phenotypes were assessed in 912 Jackson Heart Study participants with aldosterone and plasma renin activity (PRA). Multivariable linear and logistic regression analyses were used to analyze the association of aldosterone and PRA with clinic, awake, and asleep systolic BP and diastolic BP (DBP) and ABP monitoring phenotypes, adjusting for important confounders.
Results: The mean age of participants was 59±11 years and 69% were female. In fully adjusted models, lower log-PRA was associated with higher clinic, awake, and asleep systolic BP and DBP (all P<0.05). A higher log-aldosterone was associated with higher clinic, awake, and asleep DBP (all P<0.05). A 1-unit higher log-PRA was associated with lower odds of daytime hypertension (odds ratio [OR] 0.59 [95% CI, 0.49-0.71]), nocturnal hypertension (OR, 0.68 [95% CI, 0.58-0.79]), daytime and nocturnal hypertension (OR, 0.59 [95% CI, 0.48-0.71]), sustained hypertension (OR, 0.52 [95% CI, 0.39-0.70]), and masked hypertension (OR 0.75 [95% CI, 0.62-0.90]). A 1-unit higher log-aldosterone was associated with higher odds of nocturnal hypertension (OR, 1.38 [95% CI, 1.05-1.81]). Neither PRA nor aldosterone was associated with percent dipping, nondipping BP pattern, or white-coat hypertension. Patterns for aldosterone:renin ratio were similar to patterns for PRA.
Conclusions: Suppressed renin activity and higher aldosterone:renin ratios were associated with higher systolic BP and DBP in the office and during the awake and asleep periods as evidenced by ABP monitoring. Higher aldosterone levels were associated with higher DBP, but not systolic BP, in the clinic and during the awake and asleep periods. Further clinical investigation of novel and approved medications that target low renin physiology such as epithelial sodium channel inhibitors and mineralocorticoid receptor antagonists may be paramount in improving hypertension control in African Americans.
Keywords: African Americans; aldosterone; blood pressure monitoring, ambulatory; hypertension; longitudinal studies.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures


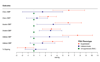

Comment in
-
Physiological Treatment of Hypertension in Black Patients: Time for Action.Circulation. 2021 Jun 15;143(24):2367-2369. doi: 10.1161/CIRCULATIONAHA.121.053880. Epub 2021 Jun 14. Circulation. 2021. PMID: 34125569 No abstract available.
References
-
- Wong MD, Shapiro MF, Boscardin WJ, Ettner SL. Contribution of Major Diseases to Disparities in Mortality. New England Journal of Medicine. 2002;347:1585–1592. - PubMed
-
- Benjamin EJ, Muntner P, Alonso A, Bittencourt MS, Callaway CW, Carson AP, Chamberlain AM, Chang AR, Cheng S, Das SR, et al. Heart Disease and Stroke Statistics—2019 Update: A Report From the American Heart Association. Circulation. 2019;139:e56–e528. - PubMed
-
- Murphy SL, Xu J, Kochanek KD, Arias E. Mortality in the United States, 2017. NCHS Data Brief. 2018;National Center for Health Statistics:8. - PubMed
-
- Feinstein M, Ning H, Kang J, Bertoni A, Carnethon M, Lloyd-Jones DM. Racial Differences in Risks for First Cardiovascular Events and Noncardiovascular Death: The Atherosclerosis Risk in Communities Study, the Cardiovascular Health Study, and the Multi-Ethnic Study of Atherosclerosis. Circulation. 2012;126:50–59. - PMC - PubMed
-
- Thomas KL, Honeycutt E, Shaw LK, Peterson ED. Racial differences in long-term survival among patients with coronary artery disease. American Heart Journal. 2010;160:744–751. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- HHSN268201100011I/HL/NHLBI NIH HHS/United States
- HHSN268201800014I/HB/NHLBI NIH HHS/United States
- R01 HL135622/HL/NHLBI NIH HHS/United States
- K23 DK117041/DK/NIDDK NIH HHS/United States
- HHSN261201800010I/CA/NCI NIH HHS/United States
- K23 HL141682/HL/NHLBI NIH HHS/United States
- HHSN268201800013I/MD/NIMHD NIH HHS/United States
- HHSN268201800011C/HL/NHLBI NIH HHS/United States
- HHSN268201800015I/HB/NHLBI NIH HHS/United States
- HHSN268201800010I/HB/NHLBI NIH HHS/United States
- HHSN268201800011I/HB/NHLBI NIH HHS/United States
- HHSN261201800014I/CA/NCI NIH HHS/United States
- HHSN268201800012I/HB/NHLBI NIH HHS/United States
- HHSN268201800012C/HL/NHLBI NIH HHS/United States
- HHSN261201800012I/CA/NCI NIH HHS/United States
- HHSN268201800014C/HL/NHLBI NIH HHS/United States
- UL1 TR002733/TR/NCATS NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

