Cervical length distribution and other sonographic ancillary findings of singleton nulliparous patients at midgestation
- PMID: 33617797
- PMCID: PMC8328864
- DOI: 10.1016/j.ajog.2021.02.017
Cervical length distribution and other sonographic ancillary findings of singleton nulliparous patients at midgestation
Abstract
Background: Short cervix at midgestation, the presence of intraamniotic debris, and cervical funneling are risk factors for preterm birth; however, cervical length measurements and cutoffs are not well documented among pregnant patients of different gestational ages and self-reported races and ethnicities.
Objective: This study aimed to describe the distribution of cervical length and frequency of funneling and debris at midgestation in nulliparous women by gestational age and race/ethnicity.
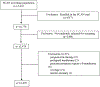
Study design: This secondary analysis of screening data from a multicenter treatment trial of singleton nulliparous patients with short cervix was conducted at 14 geographically distributed, university-affiliated medical centers in the United States. Singleton nulliparous patients with no known risk factors for preterm birth were screened for trial participation and asked to undergo a transvaginal ultrasound to measure cervical length by a certified sonographer. The distribution of cervical length and the frequency of funneling and debris were assessed for each gestational age week (16-22 weeks) and stratified by self-reported race and ethnicity, which for this study were categorized as White, Black, Hispanic, and other. Patients enrolled in the randomized trial were excluded from this analysis.
Results: A total of 12,407 nulliparous patients were included in this analysis. The racial or ethnic distribution of the study participants was as follows: White, 41.6%; Black, 29.6%; Hispanic, 24.2%; and others, 4.6%. The 10th percentile cervical length for the entire cohort was 31.1 mm and, when stratified by race and ethnicity, 31.9 mm for White, 30.2 mm for Black, 31.4 mm for Hispanic, and 31.2 mm for patients of other race and ethnicity (P<.001). At each gestational age, the cervical length corresponding to the tenth percentile was shorter in Black patients. The 25 mm value commonly used to define a short cervix and thought to represent the 10th percentile ranged from 1.3% to 5.4% across gestational age weeks and 1.0% to 3.8% across race and ethnicity groups. Black patients had the highest rate of funneling (2.6%), whereas Hispanic and Black patients had higher rates of intraamniotic debris than White and other patients (P<.001).
Conclusion: Black patients had shorter cervical length and higher rates of debris and funneling than White patients. The racial and ethnic disparities in sonographic midtrimester cervical findings may provide insight into the racial disparity in preterm birth rates in the United States.
Keywords: cervical funneling; ethnicity; intraamniotic debris; preterm birth; race; short cervix.
Copyright © 2021 Elsevier Inc. All rights reserved.
Conflict of interest statement
The authors report no conflict of interest
References
-
- Martin JA, Hamilton BE, Osterman MJK. Births in the United States, 2018. NCHS Data Brief. 2019(346):1–8. - PubMed
-
- Williamson DM, Abe K, Bean C, Ferre C, Henderson Z, Lackritz E. Current research in preterm birth. J Womens Health (Larchmt). 2008;17(10):1545–1549. - PubMed
-
- Societal costs of preterm birth. Washington, D.C.: National Academies Press; 2007.
-
- Saigal S, Doyle LW. An overview of mortality and sequelae of preterm birth from infancy to adulthood. Lancet. 2008;371(9608):261–269. - PubMed
Publication types
MeSH terms
Grants and funding
- UG1 HD027869/HD/NICHD NIH HHS/United States
- UG1 HD040560/HD/NICHD NIH HHS/United States
- UG1 HD053097/HD/NICHD NIH HHS/United States
- UG1 HD027915/HD/NICHD NIH HHS/United States
- U10 HD040485/HD/NICHD NIH HHS/United States
- U10 HD034116/HD/NICHD NIH HHS/United States
- U10 HD027869/HD/NICHD NIH HHS/United States
- U10 HD027917/HD/NICHD NIH HHS/United States
- UG1 HD040485/HD/NICHD NIH HHS/United States
- U10 HD040560/HD/NICHD NIH HHS/United States
- UG1 HD040500/HD/NICHD NIH HHS/United States
- U10 HD040512/HD/NICHD NIH HHS/United States
- U10 HD040545/HD/NICHD NIH HHS/United States
- U10 HD053118/HD/NICHD NIH HHS/United States
- UL1 RR024989/RR/NCRR NIH HHS/United States
- UL1 TR000005/TR/NCATS NIH HHS/United States
- U10 HD040500/HD/NICHD NIH HHS/United States
- U10 HD040544/HD/NICHD NIH HHS/United States
- UL1 TR002548/TR/NCATS NIH HHS/United States
- UL1 RR024153/RR/NCRR NIH HHS/United States
- UL1 RR025764/RR/NCRR NIH HHS/United States
- UG1 HD034116/HD/NICHD NIH HHS/United States
- UG1 HD040544/HD/NICHD NIH HHS/United States
- UG1 HD034208/HD/NICHD NIH HHS/United States
- UG1 HD040512/HD/NICHD NIH HHS/United States
- U10 HD027915/HD/NICHD NIH HHS/United States
- UG1 HD040545/HD/NICHD NIH HHS/United States
- U10 HD034208/HD/NICHD NIH HHS/United States
- U10 HD053097/HD/NICHD NIH HHS/United States
- P2C HD050924/HD/NICHD NIH HHS/United States
- U10 HD021410/HD/NICHD NIH HHS/United States
- U10 HD036801/HD/NICHD NIH HHS/United States
- M01 RR000080/RR/NCRR NIH HHS/United States
- U24 HD036801/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical