Disparities in pregnancy-related deaths: spatial and Bayesian network analyses of maternal mortality ratio in 54 African countries
- PMID: 33619040
- PMCID: PMC7903077
- DOI: 10.1136/bmjgh-2020-004233
Disparities in pregnancy-related deaths: spatial and Bayesian network analyses of maternal mortality ratio in 54 African countries
Abstract
Background: Maternal mortality remains a public health problem despite several global efforts. Globally, about 830 women die of pregnancy-related death per day, with more than two-third of these cases occurring in Africa. We examined the spatial distribution of maternal mortality in Africa and explored the influence of SDoH on the spatial distribution.
Methods: We used country-level secondary data of 54 African countries collected between 2006 and 2018 from three databases namely, World Development Indicator, WHO's Global Health Observatory Data and Human Development Report. We performed descriptive analyses, presented in tables and maps. The spatial analysis involved local indicator of spatial autocorrelation maps and spatial regression. Finally, we built Bayesian networks to determine and show the strength of social determinants associated with maternal mortality.
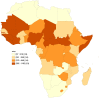
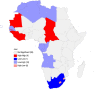
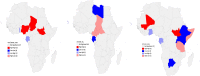
Results: We found that the average prevalence of maternal mortality ratio (MMR) in Africa was 415 per 100 000 live births. Findings from the spatial analyses showed clusters (hotspots) of MMR with seven countries (Guinea-Bissau, Guinea, Sierra Leone, Cote d'Ivoire, Chad and Cameroon, Mauritania), all within the Middle and West Africa. On the other hand, the cold spot clusters were formed by two countries; South Africa and Namibia; eight countries (Algeria, Tunisia, Libya, Ghana, Gabon and Congo, Equatorial Guinea and Cape Verde) formed low-high clusters; thus, indicating that these countries have significantly low MMR but within the neighbourhood of countries with significantly high MMR. The findings from the regression and Bayesian network analysis showed that gender inequities and the proportion of skilled birth attendant are strongest social determinants that drive the variations in maternal mortality across Africa.
Conclusion: Maternal mortality is very high in Africa especially in countries in the middle and western African subregions. To achieve the target 3.1 of the sustainable development goal on maternal health, there is a need to design effective strategies that will address gender inequalities and the shortage of health professionals.
Keywords: child health; epidemiology; health policy; health services research; maternal health.
© Author(s) (or their employer(s)) 2021. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: SY is editorial board member of this journal.
Figures

References
-
- World Health Organisation (WHO) Maternal mortality ratio (per 100 000 live births), 2014. Available: https://www.who.int/healthinfo/statistics/indmaternalmortality/en/ [Accessed 02 Aug 2020].
-
- World Health Organisation Maternal mortality, 2019. Available: https://www.who.int/news-room/fact-sheets/detail/maternal-mortality [Accessed 02 Aug 2020].
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
