Therapeutic effect of Low intensity Extracorporeal Shock Wave Therapy (Li-ESWT) on diabetic bladder dysfunction in a rat model
- PMID: 33628099
- PMCID: PMC7893573
- DOI: 10.7150/ijms.55274
Therapeutic effect of Low intensity Extracorporeal Shock Wave Therapy (Li-ESWT) on diabetic bladder dysfunction in a rat model
Abstract
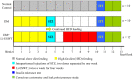
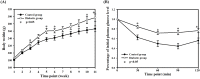
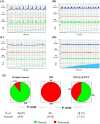
Objectives: Low intensity extracorporeal shock wave therapy (Li-ESWT) has proven to be effective and safe for the treatment of various urological disorders including erectile dysfunction and chronic pelvic pain syndrome. In this study, we elucidated the therapeutic effect and possible mechanisms of Li-ESWT on diabetic bladder dysfunction (DBD) in a rat model. Materials and Methods: In all, thirty-two female Sprague-Dawley rats were divided into three groups: normal control (NC), diabetes mellitus (DM) control, and DM Li-ESWT. The two DM groups were given high fat diets for one month, followed by 2 intraperitoneal injections of streptozotocin (STZ) 30 mg/kg separated by one week. Body weight and fasting blood glucose were monitored every week. Only rats with fasting blood glucose 140 mg/dL or more were considered diabetic and used in the subsequent portions of the study. The Li-ESWTs were applied toward the pelvis of the rats twice a week for 4 weeks with energy flux density (EFD) 0.02 mJ/mm2, 500 shocks, at 3Hz. All rats underwent plasma insulin tolerance test, conscious cystometry, leak-point pressure (LPP) assessment, and immunohistochemical studies. Results: DM groups had significantly lower insulin sensitivity and higher body weight. Conscious cystometry also revealed voiding dysfunctions. In the DM Li-ESWT group, the rats had significantly improved voiding functions that were reflected in longer micturition intervals and higher LPP compared to DM control. Immunofluorescence in DM control groups showed increased tyrosine hydroxylase (TH) expression and decreased neuronal nitric oxide synthase (nNOS) expression in the longitudinal urethral smooth muscles. Besides, rats had dilations and deformities of suburothelium capillary network of the bladder, revealing the deterioration of the nerve function of the urethra and destruction of the vascularization of the bladder. However, the DM Li-ESWT group exhibited recovery of the nerve expression of the urethra and vascularization of bladder. Conclusions: Li-ESWT ameliorates the bladder dysfunction and urinary continence in the DBD rat model, reflected in restoration of the nerve expression of the urethra and the vascularization of the bladder. Non-invasive Li-ESWT could be an alternative therapeutic option for DBD.
Keywords: bladder dysfunction; diabetes mellitus; low intensity extracorporeal shock wave.
© The author(s).
Conflict of interest statement
Competing Interests: The authors have declared that no competing interest exists.
Figures

References
-
- Guariguata L, Whiting DR, Hambleton I. et al. Global estimates of diabetes prevalence for 2013 and projections for 2035. Diabetes Res Clin Pract. 2014;103:137–49. - PubMed
-
- Goldstraw MA, Kirby MG, Bhardwa J. et al. Diabetes and the urologist: a growing problem. BJU Int. 2007;99:513–7. - PubMed
-
- Yoshimura N, Chancellor MB, Andersson KE. et al. Recent advances in understanding the biology of diabetes-associated bladder complications and novel therapy. BJU Int. 2005;95:733–8. - PubMed
-
- Barness LA, Opitz JM, Gilbert-Barness E. Obesity: genetic, molecular, and environmental aspects. Am J Med Genet A. 2007;15:3016–34. - PubMed
-
- Pan FC, Wright C. Pancreas organogenesis: from bud to plexus to gland. Dev Dyn. 2011;240:530–65. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

