Outcomes of bicanalicular nasal stent inserted by sheath-guided dacryoendoscope in patients with lacrimal passage obstruction: a retrospective observational study
- PMID: 33632167
- PMCID: PMC7905860
- DOI: 10.1186/s12886-020-01678-5
Outcomes of bicanalicular nasal stent inserted by sheath-guided dacryoendoscope in patients with lacrimal passage obstruction: a retrospective observational study
Abstract
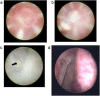
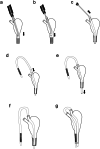
Background: The dacryoendoscope is the only instrument that can observe the luminal side of the lacrimal passage with minimal invasiveness. It was developed to treat lacrimal passage obstructions by inserting a bicanalicular nasal stent with sheath-guided bicanalicular intubation (SG-BCI). The purpose of this study was to determine the outcomes of SG-BCI to treat lacrimal passage obstructions. In addition, to determine the effects of SG-BCI treatment on the quality of life.
Methods: This was a retrospective observational study of 128 patients (mean age 70.9 ± 11.0 years, range 28-93 years) diagnosed with a unilateral lacrimal passage obstruction. There were 73 patients with a nasolacrimal duct obstruction, 37 with a lacrimal canaliculus obstruction, 7 with a lacrimal punctum obstruction, and 11 with common lacrimal canaliculus and nasolacrimal duct obstructions. They were all treated with SG-BCI. The postoperative subjective outcomes were assessed by the answers to the Glasgow Benefit Inventory (GBI) questionnaire and to an ocular specific questionnaire on 6 symptoms including tearing, ocular discharges, swelling, pain, irritation, and blurred vision. The objective assessments were the surgical success rates and the patency at 6 months after the bicanalicular nasal stent was removed. The patients were divided into those with a pre-saccal obstruction, Group 1, and with a post-saccal obstruction, Group 2. The subjective and objective outcomes were compared between the two groups.
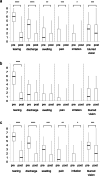
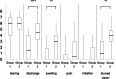
Results: One hundred twenty-four sides (96.9%) had a successful probing and intubation of the lacrimal passage obstruction by SG-BCI. Of the 124 sides, 110 sides (88.7%) retained the patency after the stent was removed for at least 6 months. The GBI total, general subscale, social support, and physical health scores were + 37.1 ± 29.0, + 41.5 ± 30.0, + 28.0 ± 39.4, and + 24.1 ± 37.7, respectively, postoperatively. All of the 6 ocular specific symptom scores improved significantly postoperatively. The postoperative score of tearing improved in Group 1 (P < 0.0001), while the postoperative scores of all symptoms improved significantly in Group 2.
Conclusions: The relatively high surgical success rates and positive GBI scores, and improved ocular symptom scores indicate that SG-BCI is a good minimally invasive method to treat lacrimal passage obstructions.
Keywords: Bicanalicular intubation; Dacryoendoscope; Glasgow benefit inventory; Lacrimal passage obstruction; Lacrimal stent.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
-
- Toti A. Nuovo metodo conservatore di cura radicale delle suppurazioni croniche del sacco lacrimale (dacriocistorinostomia) Clin Mod. 1904;10:385–387.
-
- Killian J. Diskussion zu seiferts vortrag. Verhandlungen des Vereins Süddeutscher Laryngologen. 1899;6.
-
- Caldwell GW. Two new operations for obstructions of the nasal duct with preservation of canaliculi and an incidental description of a new lacrimal probe. New York MJ. 1893;57:581–582.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

