Combined pars plana glaucoma drainage device placement and vitrectomy using a vitrectomy sclerotomy site for tube placement: a case series
- PMID: 33632169
- PMCID: PMC7905981
- DOI: 10.1186/s12886-021-01872-z
Combined pars plana glaucoma drainage device placement and vitrectomy using a vitrectomy sclerotomy site for tube placement: a case series
Abstract
Purpose: The purpose of this study is to report the safety and efficacy of pars plana glaucoma drainage devices with pars plana vitrectomy using one of the vitrectomy sclerotomy sites for tube placement in patients with refractory glaucoma.
Methods: Retrospective case series of 28 eyes of 28 patients who underwent combined pars plana glaucoma drainage device and pars plana vitrectomy between November 2016 and September 2019 at Massachusetts Eye and Ear. Main outcome measures were intraocular pressure (IOP), glaucoma medication burden, best corrected visual acuity, and complications. Statistical tests were performed with R and included Kaplan-Meier analyses, Wilcoxon paired signed-rank tests, and Fisher tests.
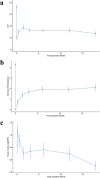
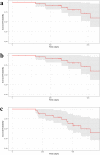
Results: Mean IOP decreased from 22.8 mmHg to 11.8 mmHg at 1.5 years (p = 0.002), and mean medication burden decreased from 4.3 to 2.1 at 1.5 years (p = 0.004). Both IOP and medication burden were significantly lower at all follow-up time points. The probability of achieving 5 < IOP ≤ 18 mmHg with at least 20% IOP reduction from preoperative levels was 86.4% at 1 year and 59.8% at 1.5 years. At their last visit, three eyes (10.7%) achieved complete success with IOP reduction as above without medications, and 14 eyes (50.0%) achieved qualified success with medications. Hypotony was observed in 1 eye (3.6%) prior to 3 months postoperatively and 0 eyes after 3 months. Visual acuity was unchanged or improved in 23 eyes (82.1%) at their last follow-up. Two patients had a visual acuity decrease of > 2 lines. Two eyes required subsequent pars plana vitrectomies for tube obstruction, and one eye had transient hypotony.
Conclusions: The results of pars plana glaucoma drainage device and pars plana vitrectomy using one of the vitrectomy sclerotomy sites for tube placement are promising, resulting in significant IOP and medication-burden reductions through postoperative year 1.5 without additional risk of postoperative complications. Inserting glaucoma drainage devices into an existing vitrectomy sclerotomy site may potentially save surgical time by obviating the need to create another sclerotomy for tube placement and suture one of the vitrectomy ports.
Keywords: Ahmed drainage implant; Baerveldt drainage implant; Efficacy; Glaucoma; Pars plana; Pars plana glaucoma drainage device; Pars plana vitrectomy; Safety.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Combined pars plana vitrectomy and pars plana Baerveldt tube placement in eyes with neovascular glaucoma.Retina. 2015 Jan;35(1):17-28. doi: 10.1097/IAE.0000000000000235. Retina. 2015. PMID: 25046391
-
23-Gauge pars plana vitrectomy with pars plana Baerveldt tube placement for refractory glaucoma.Eur J Ophthalmol. 2012 Jan-Feb;22(1):90-4. doi: 10.5301/ejo.5000027. Eur J Ophthalmol. 2012. PMID: 22167547
-
Pars plana Ahmed implantation combined with 23-gauge vitrectomy for refractory neovascular glaucoma in diabetic retinopathy.Korean J Ophthalmol. 2012 Apr;26(2):92-6. doi: 10.3341/kjo.2012.26.2.92. Epub 2012 Mar 22. Korean J Ophthalmol. 2012. PMID: 22511834 Free PMC article.
-
The Baerveldt Glaucoma Drainage Device: Efficacy, Safety, and Place in Therapy.Clin Ophthalmol. 2020 Sep 24;14:2789-2797. doi: 10.2147/OPTH.S219271. eCollection 2020. Clin Ophthalmol. 2020. PMID: 33061263 Free PMC article. Review.
-
Management of endophthalmitis related to glaucoma drainage devices: review of the literature and our experience.Eye (Lond). 2021 Jul;35(7):1850-1858. doi: 10.1038/s41433-021-01462-9. Epub 2021 Mar 5. Eye (Lond). 2021. PMID: 33674726 Free PMC article. Review.
Cited by
-
Challenges of Secondary Glaucoma Management Following Congenital Cataract Surgery, Penetrating Keratoplasty and Vitreoretinal Surgery.Diagnostics (Basel). 2024 Apr 18;14(8):837. doi: 10.3390/diagnostics14080837. Diagnostics (Basel). 2024. PMID: 38667482 Free PMC article.
-
Safety and efficacy of microinvasive glaucoma surgery with cataract extraction in patients with normal-tension glaucoma.Sci Rep. 2021 Apr 26;11(1):8910. doi: 10.1038/s41598-021-88358-6. Sci Rep. 2021. PMID: 33903701 Free PMC article.
-
Outcomes of a combination of augmented MicroPulse and limited Continuous Wave Cyclophotocoagulation in patients with refractory glaucoma.Graefes Arch Clin Exp Ophthalmol. 2022 May;260(5):1583-1592. doi: 10.1007/s00417-021-05436-1. Epub 2021 Oct 25. Graefes Arch Clin Exp Ophthalmol. 2022. PMID: 34694455 Free PMC article.
-
Surgical Outcomes of Glaucoma Drainage Device Implantation in Refractory Glaucoma Patients in Thailand.Clin Ophthalmol. 2022 Dec 14;16:4163-4178. doi: 10.2147/OPTH.S393730. eCollection 2022. Clin Ophthalmol. 2022. PMID: 36540897 Free PMC article.
-
Commentary: Placement of the tube of a glaucoma drainage device: Different horses for different courses.Indian J Ophthalmol. 2022 Mar;70(3):845-846. doi: 10.4103/ijo.IJO_2877_21. Indian J Ophthalmol. 2022. PMID: 35225527 Free PMC article. No abstract available.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

