Daily Morning Blue Light Therapy for Post-mTBI Sleep Disruption: Effects on Brain Structure and Function
- PMID: 33633674
- PMCID: PMC7901882
- DOI: 10.3389/fneur.2021.625431
Daily Morning Blue Light Therapy for Post-mTBI Sleep Disruption: Effects on Brain Structure and Function
Abstract
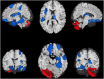
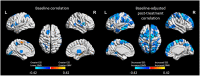
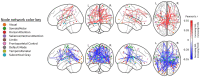
Background: Mild traumatic brain injuries (mTBIs) are associated with novel or worsened sleep disruption. Several studies indicate that daily morning blue light therapy (BLT) is effective for reducing post-mTBI daytime sleepiness and fatigue. Studies demonstrating changes in brain structure and function following BLT are limited. The present study's purpose is to identify the effect of daily morning BLT on brain structure and functional connectivity and the association between these changes and self-reported change in post-mTBI daytime sleepiness. Methods: A total of 62 individuals recovering from a mTBI were recruited from two US cities to participate in a double-blind placebo-controlled trial. Eligible individuals were randomly assigned to undergo 6 weeks of 30 min daily morning blue or placebo amber light therapy (ALT). Prior to and following treatment all individuals completed a comprehensive battery that included the Epworth Sleepiness Scale as a measure of self-reported daytime sleepiness. All individuals underwent a multimodal neuroimaging battery that included anatomical and resting-state functional magnetic resonance imaging. Atlas-based regional change in gray matter volume (GMV) and region-to-region functional connectivity from baseline to post-treatment were the primary endpoints for this study. Results: After adjusting for pre-treatment GMV, individuals receiving BLT had greater GMV than those receiving amber light in 15 regions of interest, including the right thalamus and bilateral prefrontal and orbitofrontal cortices. Improved daytime sleepiness was associated with greater GMV in 74 ROIs, covering many of the same general regions. Likewise, BLT was associated with increased functional connectivity between the thalamus and both prefrontal and orbitofrontal cortices. Improved daytime sleepiness was associated with increased functional connectivity between attention and cognitive control networks as well as decreased connectivity between visual, motor, and attention networks (all FDR corrected p < 0.05). Conclusions: Following daily morning BLT, moderate to large increases in both gray matter volume and functional connectivity were observed in areas and networks previously associated with both sleep regulation and daytime cognitive function, alertness, and attention. Additionally, these findings were associated with improvements in self-reported daytime sleepiness. Further work is needed to identify the personal characteristics that may selectively identify individuals recovering from a mTBI for whom BLT may be optimally beneficial.
Keywords: concussion; daytime sleepiness; fatigue; functional connectivity; gray matter volume; phototherapy.
Copyright © 2021 Raikes, Dailey, Forbeck, Alkozei and Killgore.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
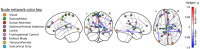
Similar articles
-
A randomized, double-blind, placebo-controlled trial of blue wavelength light exposure on sleep and recovery of brain structure, function, and cognition following mild traumatic brain injury.Neurobiol Dis. 2020 Feb;134:104679. doi: 10.1016/j.nbd.2019.104679. Epub 2019 Nov 18. Neurobiol Dis. 2020. PMID: 31751607 Clinical Trial.
-
Daily Morning Blue Light Therapy Improves Daytime Sleepiness, Sleep Quality, and Quality of Life Following a Mild Traumatic Brain Injury.J Head Trauma Rehabil. 2020 Sep/Oct;35(5):E405-E421. doi: 10.1097/HTR.0000000000000579. J Head Trauma Rehabil. 2020. PMID: 32472836 Clinical Trial.
-
Treatment with morning blue light increases left amygdala volume and sleep duration among individuals with posttraumatic stress disorder.Front Behav Neurosci. 2022 Sep 12;16:910239. doi: 10.3389/fnbeh.2022.910239. eCollection 2022. Front Behav Neurosci. 2022. PMID: 36172470 Free PMC article.
-
Sleep in children with neoplasms of the central nervous system: case review of 14 children.Pediatrics. 2003 Jul;112(1 Pt 1):e46-54. doi: 10.1542/peds.112.1.e46. Pediatrics. 2003. PMID: 12837905 Review.
-
[Bright light therapy for elderly].Nihon Rinsho. 2015 Jun;73(6):997-1005. Nihon Rinsho. 2015. PMID: 26065132 Review. Japanese.
Cited by
-
Effectiveness of biomedical interventions on the chronic stage of traumatic brain injury: a systematic review of randomized controlled trials.Front Neurol. 2024 Mar 18;15:1321239. doi: 10.3389/fneur.2024.1321239. eCollection 2024. Front Neurol. 2024. PMID: 38562423 Free PMC article.
-
Traumatic brain injury and sleep in military and veteran populations: A literature review.NeuroRehabilitation. 2024;55(3):245-270. doi: 10.3233/NRE-230380. NeuroRehabilitation. 2024. PMID: 39121144 Free PMC article. Review.
-
Effects of docosahexaenoic acid and eicosapentaoic acid supplementation on white matter integrity after repetitive sub-concussive head impacts during American football: Exploratory neuroimaging findings from a pilot RCT.Front Neurol. 2022 Sep 15;13:891531. doi: 10.3389/fneur.2022.891531. eCollection 2022. Front Neurol. 2022. PMID: 36188406 Free PMC article.
-
Concussion and the Autonomic, Immune, and Endocrine Systems: An Introduction to the Field and a Treatment Framework for Persisting Symptoms.J Pers Med. 2025 Jan 17;15(1):33. doi: 10.3390/jpm15010033. J Pers Med. 2025. PMID: 39852225 Free PMC article. Review.
-
Feasibility and acceptability for LION, a fully remote, randomized clinical trial within the VA for light therapy to improve sleep in Veterans with and without TBI: An MTBI2 sponsored protocol.medRxiv [Preprint]. 2024 May 31:2024.05.30.24308195. doi: 10.1101/2024.05.30.24308195. medRxiv. 2024. Update in: PLoS One. 2025 Jan 7;20(1):e0305305. doi: 10.1371/journal.pone.0305305. PMID: 38853958 Free PMC article. Updated. Preprint.
References
-
- Faul M, Xu L, Wald MM, Coronado VG. Traumatic Brain Injury in the United States: Emergency Department Visits, Hospitalizations and Deaths 2002-2006. Atlanta (GA): Centers for Disease Control and Prevention, National Center for Injury Prevention and Control; (2010). Available online at: https://www.cdc.gov/traumaticbraininjury/tbi_ed.html (accessed April 25, 2015). 10.15620/cdc.5571 - DOI
-
- Kerr Z, Roos K, Dompier T, Dalton S, Djoko A, Broglio S, et al. Estimating concussion incidence in college sports: rates, risks, average per team and proportion of teams with concussions. In: Brain Injury. Philadelphia, PA: Taylor & Francis Inc; (2016), p. 504.
-
- Defense and Veterans Brain Injury Center DoD Worldwide TBI Numbers 2000-2018 Q1. (2018). Available online at: https://health.mil/Reference-Center/Publications/2020/09/30/2000-2019-Do... (accessed August 27, 2019).
-
- Pattinson CL, Meier TB, Guedes VA, Lai C, Devoto C, Haight T, et al. . Plasma biomarker concentrations associated with return to sport following sport-related concussion in collegiate athletes—A Concussion Assessment, Research, and Education (CARE) Consortium Study. JAMA Netw Open. (2020) 3:e2013191. 10.1001/jamanetworkopen.2020.13191 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

