Life Support Limitations in Mechanically Ventilated Stroke Patients
- PMID: 33634264
- PMCID: PMC7901798
- DOI: 10.1097/CCE.0000000000000341
Life Support Limitations in Mechanically Ventilated Stroke Patients
Abstract
Objectives: The determinants of decisions to limit life support (withholding or withdrawal) in ventilated stroke patients have been evaluated mainly for patients with intracranial hemorrhages. We aimed to evaluate the frequency of life support limitations in ventilated ischemic and hemorrhagic stroke patients compared with a nonbrain-injured population and to determine factors associated with such decisions.
Design: Multicenter prospective French observational study.
Setting: Fourteen ICUs of the French OutcomeRea network.
Patients: From 2005 to 2016, we included stroke patients and nonbrain-injured patients requiring invasive ventilation within 24 hours of ICU admission.
Intervention: None.
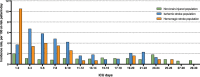
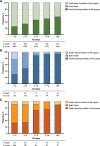
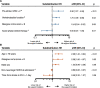
Measurements and main results: We identified 373 stroke patients (ischemic, n = 167 [45%]; hemorrhagic, n = 206 [55%]) and 5,683 nonbrain-injured patients. Decisions to limit life support were taken in 41% of ischemic stroke cases (vs nonbrain-injured patients, subdistribution hazard ratio, 3.59 [95% CI, 2.78-4.65]) and in 33% of hemorrhagic stroke cases (vs nonbrain-injured patients, subdistribution hazard ratio, 3.9 [95% CI, 2.97-5.11]). Time from ICU admission to the first limitation was longer in ischemic than in hemorrhagic stroke (5 [3-9] vs 2 d [1-6] d; p < 0.01). Limitation of life support preceded ICU death in 70% of ischemic strokes and 45% of hemorrhagic strokes (p < 0.01). Life support limitations in ischemic stroke were increased by a vertebrobasilar location (vs anterior circulation, subdistribution hazard ratio, 1.61 [95% CI, 1.01-2.59]) and a prestroke modified Rankin score greater than 2 (2.38 [1.27-4.55]). In hemorrhagic stroke, an age greater than 70 years (2.29 [1.43-3.69]) and a Glasgow Coma Scale score less than 8 (2.15 [1.08-4.3]) were associated with an increased risk of limitation, whereas a higher nonneurologic admission Sequential Organ Failure Assessment score was associated with a reduced risk (per point, 0.89 [0.82-0.97]).
Conclusions: In ventilated stroke patients, decisions to limit life support are more than three times more frequent than in nonbrain-injured patients, with different timing and associated risk factors between ischemic and hemorrhagic strokes.
Keywords: critical care; end-of-life care; intracerebral hemorrhage; ischemic stroke; subarachnoid hemorrhage.
Copyright © 2021 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine.
Conflict of interest statement
Dr. Thiéry has received honoraria from Gilead-Kite. The remaining authors have disclosed that they do not have any conflicts of interest.
Figures
Similar articles
-
One-Year Outcomes in Patients With Acute Stroke Requiring Mechanical Ventilation.Stroke. 2023 Sep;54(9):2328-2337. doi: 10.1161/STROKEAHA.123.042910. Epub 2023 Jul 27. Stroke. 2023. PMID: 37497675
-
Long-Term Mortality Among ICU Patients With Stroke Compared With Other Critically Ill Patients.Crit Care Med. 2020 Oct;48(10):e876-e883. doi: 10.1097/CCM.0000000000004492. Crit Care Med. 2020. PMID: 32931193
-
Patient factors and outcomes associated with the withdrawal or withholding of life-sustaining therapies in mechanically ventilated brain-injured patients: An observational multicentre study.Eur J Anaesthesiol. 2018 Jul;35(7):511-518. doi: 10.1097/EJA.0000000000000783. Eur J Anaesthesiol. 2018. PMID: 29419564
-
Twenty-Year Change in Severity and Outcome of Ischemic and Hemorrhagic Strokes.JAMA Neurol. 2022 Jan 1;79(1):61-69. doi: 10.1001/jamaneurol.2021.4346. JAMA Neurol. 2022. PMID: 34870689 Free PMC article.
-
Nontraumatic Intracranial Hemorrhage.2020 Feb 15. In: Hodler J, Kubik-Huch RA, von Schulthess GK, editors. Diseases of the Brain, Head and Neck, Spine 2020–2023: Diagnostic Imaging [Internet]. Cham (CH): Springer; 2020. Chapter 5. 2020 Feb 15. In: Hodler J, Kubik-Huch RA, von Schulthess GK, editors. Diseases of the Brain, Head and Neck, Spine 2020–2023: Diagnostic Imaging [Internet]. Cham (CH): Springer; 2020. Chapter 5. PMID: 32119243 Free Books & Documents. Review.
Cited by
-
Outcomes of patients admitted to the ICU for acute stroke: a retrospective cohort.BMC Anesthesiol. 2022 Jul 25;22(1):235. doi: 10.1186/s12871-022-01777-4. BMC Anesthesiol. 2022. PMID: 35879652 Free PMC article.
-
Long-Term Outcomes After Severe Acute Brain Injury Requiring Mechanical Ventilation: Recovery Trajectories Among Patients and Mental Health Symptoms of Their Surrogate Decision Makers.Neurocrit Care. 2025 Jun;42(3):896-910. doi: 10.1007/s12028-024-02164-2. Epub 2024 Nov 19. Neurocrit Care. 2025. PMID: 39562389
-
Selective decontamination of the digestive tract: it's all in your mind!Intensive Care Med. 2024 Jan;50(1):128-130. doi: 10.1007/s00134-023-07286-3. Epub 2023 Dec 21. Intensive Care Med. 2024. PMID: 38127144 No abstract available.
References
-
- Santoli F, De Jonghe B, Hayon J, et al. . Mechanical ventilation in patients with acute ischemic stroke: Survival and outcome at one year. Intensive Care Med. 2001; 27:1141–1146 - PubMed
-
- Schielke E, Busch MA, Hildenhagen T, et al. . Functional, cognitive and emotional long-term outcome of patients with ischemic stroke requiring mechanical ventilation. J Neurol. 2005; 252:648–654 - PubMed
-
- Milhaud D, Popp J, Thouvenot E, et al. . Mechanical ventilation in ischemic stroke. J Stroke Cerebrovasc Dis. 2004; 13:183–188 - PubMed
-
- Sonneville R, Gimenez L, Labreuche J, et al. . What is the prognosis of acute stroke patients requiring ICU admission? Intensive Care Med. 2017; 43:271–272 - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

