Biomarkers associated with periodontitis and peri-implantitis: a systematic review
- PMID: 33634611
- PMCID: PMC7920841
- DOI: 10.5051/jpis.1902840142
Biomarkers associated with periodontitis and peri-implantitis: a systematic review
Abstract
Purpose: The pathology of peri-implantitis is still not fully understood and there have been recent challenges to the consensus on its aetiology and pathology, especially in comparison with periodontitis. The assessment of biomarkers allows a comparison of the pathology of these diseases. The aim of this systematic review was to answer the research question: "Is there a difference in the biomarkers associated with peri-implantitis compared with periodontitis in adult humans?"
Methods: Electronic databases were searched and screened, and a manual search was also undertaken. The inclusion criteria were adults with peri-implantitis who had been compared to adults with periodontitis with the outcome of biomarkers assessed via biopsies or crevicular fluid samples in primary or secondary care settings, as recorded in case-control, case series and retrospective, prospective and cross-sectional observational studies. Two reviewers independently screened titles and abstracts and assessed full text articles for eligibility and inclusion. Both reviewers independently extracted data and assessed risk of bias. Differences in biomarker levels were the primary outcome and a narrative review was undertaken due to the heterogeneity of studies.
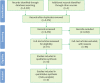
Results: In total, 2,374 articles were identified in the search, of which 111 full-text articles were assessed for eligibility and 13 were included in the qualitative synthesis. Five of the 13 included studies were deemed to be at high risk of bias, with the others having moderate risk. All studies were cross-sectional and performed at university hospitals. Nine of the 13 included studies found significant differences in the levels of biomarkers or their ratios between peri-implantitis and periodontitis. Four of the studies found no significant differences.
Conclusions: Within the limitations of the included studies, it appears that there may be a difference in biomarker levels and ratios between peri-implantitis and periodontitis, suggesting that these disease processes are somewhat distinct.
Keywords: Biomarkers; Cytokines; Peri-implantitis; Periodontitis.
Copyright © 2021. Korean Academy of Periodontology.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
Similar articles
-
Is there a correlation between peri-implantitis and systemic inflammation?Evid Based Dent. 2024 Jun;25(2):69-70. doi: 10.1038/s41432-024-00985-w. Epub 2024 Feb 15. Evid Based Dent. 2024. PMID: 38360889
-
Impact of COVID-19 on Periodontitis and Peri-Implantitis: A Narrative Review.Front Oral Health. 2022 Feb 10;3:822824. doi: 10.3389/froh.2022.822824. eCollection 2022. Front Oral Health. 2022. PMID: 35224542 Free PMC article. Review.
-
Histopathological and microbiological findings associated with retrograde peri-implantitis of extra-radicular endodontic origin: a systematic and critical review.Int J Oral Maxillofac Surg. 2019 Nov;48(11):1475-1484. doi: 10.1016/j.ijom.2019.04.012. Epub 2019 May 11. Int J Oral Maxillofac Surg. 2019. PMID: 31088705
-
Bone loss biomarkers associated with peri-implantitis. A cross-sectional study.Clin Oral Implants Res. 2013 Oct;24(10):1110-6. doi: 10.1111/j.1600-0501.2012.02518.x. Epub 2012 Jun 18. Clin Oral Implants Res. 2013. PMID: 22708989
-
Periodontitis as a risk factor for peri-implantitis: Systematic review and meta-analysis of observational studies.J Dent. 2018 Dec;79:1-10. doi: 10.1016/j.jdent.2018.09.010. Epub 2018 Nov 2. J Dent. 2018. PMID: 30391683
Cited by
-
The Characteristics of Microbiome and Cytokines in Healthy Implants and Peri-Implantitis of the Same Individuals.J Clin Med. 2022 Sep 30;11(19):5817. doi: 10.3390/jcm11195817. J Clin Med. 2022. PMID: 36233685 Free PMC article.
-
Oral Fluid Biomarkers for Peri-Implantitis: A Scoping Review.Int Dent J. 2024 Jun;74(3):387-402. doi: 10.1016/j.identj.2023.11.005. Epub 2023 Dec 8. Int Dent J. 2024. PMID: 38065782 Free PMC article.
-
Increased of IL-18 levels are associated with periodontitis: a systematic review and meta-analysis.BMC Oral Health. 2024 Aug 23;24(1):981. doi: 10.1186/s12903-024-04747-z. BMC Oral Health. 2024. PMID: 39179998 Free PMC article.
-
The role of probiotic therapy on clinical parameters and human immune response in peri-implant diseases: a systematic review and meta-analysis of randomized clinical studies.Front Immunol. 2024 Apr 15;15:1371072. doi: 10.3389/fimmu.2024.1371072. eCollection 2024. Front Immunol. 2024. PMID: 38686378 Free PMC article.
-
Diagnostic value of aMMP-8 and azurocidin in peri-implant sulcular fluid as biomarkers of peri-implant health or disease.Clin Exp Dent Res. 2024 Jun;10(3):e883. doi: 10.1002/cre2.883. Clin Exp Dent Res. 2024. PMID: 38853451 Free PMC article.
References
-
- Derks J, Tomasi C. Peri-implant health and disease. A systematic review of current epidemiology. J Clin Periodontol. 2015;42(Suppl 16):S158–S171. - PubMed
-
- Heitz-Mayfield LJ, Needleman I, Salvi GE, Pjetursson BE. Consensus statements and clinical recommendations for prevention and management of biologic and technical implant complications. Int J Oral Maxillofac Implants. 2014;29(Suppl):346–350. - PubMed
-
- Heitz-Mayfield LJ, Mombelli A. The therapy of peri-implantitis: a systematic review. Int J Oral Maxillofac Implants. 2014;29(Suppl):325–345. - PubMed
-
- Lang NP, Berglundh T Working Group 4 of Seventh European Workshop on Periodontology. Periimplant diseases: Where are we now?--Consensus of the Seventh European Workshop on Periodontology. J Clin Periodontol. 2011;38(Suppl 11):178–181. - PubMed
-
- Berglundh T, Zitzmann NU, Donati M. Are peri-implantitis lesions different from periodontitis lesions? J Clin Periodontol. 2011;38(Suppl 11):188–202. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources