Optimal Complete Rectum Mobilization Focused on the Anatomy of the Pelvic Fascia and Autonomic Nerves: 30 Years of Experience at Severance Hospital
- PMID: 33635008
- PMCID: PMC7934104
- DOI: 10.3349/ymj.2021.62.3.187
Optimal Complete Rectum Mobilization Focused on the Anatomy of the Pelvic Fascia and Autonomic Nerves: 30 Years of Experience at Severance Hospital
Abstract
The primary goal of surgery for rectal cancer is to achieve an oncologically safe resection, i.e., a radical resection with a sufficient safe margin. Total mesorectal excision has been introduced for radical surgery of rectal cancer and has yielded greatly improved oncologic outcomes in terms of local recurrence and cancer-specific survival. Along with oncologic outcomes, functional outcomes, such as voiding and sexual function, have also been emphasized in patients undergoing rectal cancer surgery to improve quality of life. Intraoperative nerve damage or combined excision is the primary reason for sexual and urinary dysfunction. In the past, these forms of damage could be attributed to the lack of anatomical knowledge and poor visualization of the pelvic autonomic nerve. With the adoption of minimally invasive surgery, visualization of nerve structure and meticulous dissection for the mesorectum are now possible. As the leading hospital employing this technique, we have adopted minimally invasive platforms (laparoscopy, robot-assisted surgery) in the field of rectal cancer surgery and standardized this technique globally. Here, we review a standardized technique for rectal cancer surgery based on our experience at Severance Hospital, suggest some practical technical tips, and discuss a couple of debatable issues in this field.
Keywords: Total mesorectal excision; anatomy; rainbow technique; rectal cancer.
© Copyright: Yonsei University College of Medicine 2021.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures
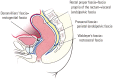

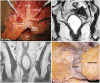
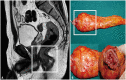
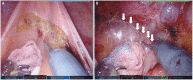


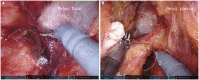

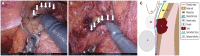
References
-
- Bokey EL, Ojerskog B, Chapuis PH, Dent OF, Newland RC, Sinclair G. Local recurrence after curative excision of the rectum for cancer without adjuvant therapy: role of total anatomical dissection. Br J Surg. 1999;86:1164–1170. - PubMed
-
- Heald RJ. A new approach to rectal cancer. Br J Hosp Med. 1979;22:277–281. - PubMed
-
- Piso P, Dahlke MH, Mirena P, Schmidt U, Aselmann H, Schlitt HJ, et al. Total mesorectal excision for middle and lower rectal cancer: a single institution experience with 337 consecutive patients. J Surg Oncol. 2004;86:115–121. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

