Lymph Node Ratio Is a Strong Prognostic Factor in Patients with Early-Stage Cervical Cancer Undergoing Minimally Invasive Radical Hysterectomy
- PMID: 33635013
- PMCID: PMC7934101
- DOI: 10.3349/ymj.2021.62.3.231
Lymph Node Ratio Is a Strong Prognostic Factor in Patients with Early-Stage Cervical Cancer Undergoing Minimally Invasive Radical Hysterectomy
Abstract
Purpose: To determine whether the prognostic impact of lymph node ratio (LNR), defined as the ratio between the number of positive lymph nodes and removed lymph nodes, differs between open and minimally invasive surgical approaches for radical hysterectomy (RH) in node-positive, early-stage cervical cancer.
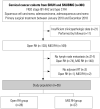
Materials and methods: We retrospectively identified 2009 International Federation of Gynecology and Obstetrics stage IB1-IIA2 patients who underwent primary type C RH between 2010 and 2018. Among them, only those with pathologically proven lymph node metastases who received adjuvant radiation therapy were included. The prognostic significance of LNR was investigated according to open surgery and minimally invasive surgery (MIS).
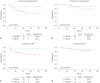
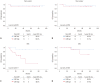
Results: In total, 55 patients were included. The median LNR (%) was 9.524 (range, 2.083-62.500). Based on receiver operating characteristic curve analysis, the cut-off value for LNR (%) was determined as 8.831. Overall, patients with high LNR (≥8.831%; n=29) showed worse disease-free survival (DFS) than those with low LNR (<8.831%, n=26) (p=0.027), whereas no difference in overall survival was observed. Multivariate analyses adjusting for clinicopathologic factors revealed that DFS was adversely affected by both MIS [adjusted hazard ratio (HR), 8.132; p=0.038] and high LNR (adjusted HR, 10.837; p=0.045). In a subgroup of open surgery cases, LNR was not associated with disease recurrence. However, in a subgroup of MIS cases, high LNR was identified as an independent poor prognostic factor for DFS (adjusted HR, 14.578; p=0.034).
Conclusion: In patients with node-positive, early-stage cervical cancer, high LNR was associated with a significantly higher disease recurrence rate. This relationship was further consolidated among patients who received MIS RH.
Keywords: Cervical cancer; laparoscopic surgery; lymph node ratio; minimally invasive surgery; radical hysterectomy; recurrence.
© Copyright: Yonsei University College of Medicine 2021.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures
References
-
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68:394–424. - PubMed
-
- Ramirez PT, Frumovitz M, Pareja R, Lopez A, Vieira M, Ribeiro R, et al. Minimally invasive versus abdominal radical hysterectomy for cervical cancer. N Engl J Med. 2018;379:1895–1904. - PubMed
-
- Kim SI, Cho JH, Seol A, Kim YI, Lee M, Kim HS, et al. Comparison of survival outcomes between minimally invasive surgery and conventional open surgery for radical hysterectomy as primary treatment in patients with stage IB1-IIA2 cervical cancer. Gynecol Oncol. 2019;153:3–12. - PubMed
-
- Uppal S, Gehrig PA, Peng K, Bixel KL, Matsuo K, Vetter MH, et al. Recurrence rates in patients with cervical cancer treated with abdominal versus minimally invasive radical hysterectomy: a multiinstitutional retrospective review study. J Clin Oncol. 2020;38:1030–1040. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

