Outcomes of Femoral Artery Pseudoaneurysm in Intravenous Drug Abusers Managed at a Tertiary Care Center
- PMID: 33643755
- PMCID: PMC7885738
- DOI: 10.7759/cureus.13350
Outcomes of Femoral Artery Pseudoaneurysm in Intravenous Drug Abusers Managed at a Tertiary Care Center
Abstract
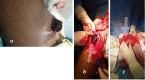
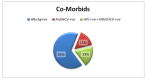
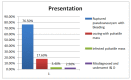
Objectives The aim of this study was to assess the effects of ligation and excision of femoral artery pseudoaneurysm without revascularization in intravenous drug abusers presenting in the tertiary care center. Methods This was a retrospective study conducted at Shaheed Mohtarma Benazir Bhutto Institute, Karachi, Pakistan, and included 119 patients admitted for vascular injuries of the groin between June 2016 and June 2020. Data collected from the hospital's medical records included all intravenous drug addicts presented with mass near or at groin area only, while other pseudoaneurysm locations secondary to vascular trauma, arteriovenous fistula, and hemodialysis were excluded. SPSS Version 20.0 (IBM Corp., Armonk, NY, USA) was used for data analysis. Results This study included 119 patients, all of whom presented and admitted to the Accident and Emergency Department, with a mean age of about 32 years ± 11.34 years and a mean duration of addiction of 2.47 years ± 1.37 years. Males constituted 83.2% of the patients, while females constituted 16.8%. The left femoral artery was affected more commonly than the right femoral artery, with an average of 75.6% and 24.4%, respectively. The most common presentation was bleeding from ruptured pseudoaneurysm (76.5%) and oozing with pulsatile mass (17.6%), while infected pulsatile swelling and misdiagnosis were uncommon. After surgical intervention, limb salvage was 95.8%, whereas mortality and amputation rate were 2.5 % and 1.7%, respectively. Conclusion The optimal management of femoral artery pseudoaneurysm in intravenous drug addicts is ligation and excision of the pseudoaneurysm without revascularization.
Keywords: excision; femoral artery pseudoaneurysm; intravenous drug abusers (ivda); intravenous drug user; ligation; pseudoaneurysm; vascular complication; vascular surgery.
Copyright © 2021, DDin et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
-
- Drug abuse in Pakistan reaches alarming level. [Dec;2020 ];https://nation.com.pk/10-Feb-2018/drug-abuse-in-pakistan-reaches-alarmin... 2018
-
- Outcomes of femoral artery ligation for treatment of infected femoral pseudoaneurysms due to drug injection. Quiroga E, Shalhub S, Tran NT, Starnes BW, Singh N. https://www.sciencedirect.com/science/article/abs/pii/S0741521420314658. J Vasc Surg. 2021;73:635–640. - PubMed
-
- Vascular injuries in intravenous drug addicts—a single-center experience. Ilic A, Stevanovic K, Pejkic S, Markovic M, Dimic A, Sladojevic M, Davidovic L. Ann Vasc Surg. 2020;67:185–191. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources