Provider Teams Outperform Solo Providers In Managing Chronic Diseases And Could Improve The Value Of Care
- PMID: 33646870
- PMCID: PMC9166311
- DOI: 10.1377/hlthaff.2020.01580
Provider Teams Outperform Solo Providers In Managing Chronic Diseases And Could Improve The Value Of Care
Abstract
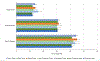
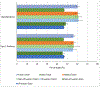
Scope-of-practice regulations, including prescribing limits and supervision requirements, may influence the propensity of providers to form care teams. Therefore, policy makers need to understand the effect of both team-based care and provider type on clinical outcomes. We examined how care management and biomarker outcomes after the onset of three chronic diseases differed both by team-based versus solo care and by physician versus nonphysician (that is, nurse practitioner and physician assistant) care. Using 2013-18 deidentified electronic health record data from US primary care practices, we found that provider teams outperformed solo providers, irrespective of team composition. Among solo providers, physicians and nonphysicians exhibited little meaningful difference in performance. As policy makers contemplate scope-of-practice changes, they should consider the effects of not only provider type but also team-based care on outcomes. Interventions that may encourage provider team formation, including scope-of-practice reforms, may improve the value of care.
Figures


Similar articles
-
Quality of Prescribing by Physicians, Nurse Practitioners, and Physician Assistants in the United States.Pharmacotherapy. 2018 Apr;38(4):417-427. doi: 10.1002/phar.2095. Epub 2018 Mar 26. Pharmacotherapy. 2018. PMID: 29457258
-
Nurse Practitioners, Physician Assistants, and Physicians Are Comparable in Managing the First Five Years of Diabetes.Am J Med. 2018 Mar;131(3):276-283.e2. doi: 10.1016/j.amjmed.2017.08.026. Epub 2017 Sep 8. Am J Med. 2018. PMID: 28893514 Free PMC article.
-
Division of primary care services between physicians, physician assistants, and nurse practitioners for older patients with diabetes.Med Care Res Rev. 2013 Oct;70(5):531-41. doi: 10.1177/1077558713495453. Epub 2013 Jul 17. Med Care Res Rev. 2013. PMID: 23868081 Free PMC article.
-
Nurse practitioners and physician assistants in the intensive care unit: an evidence-based review.Crit Care Med. 2008 Oct;36(10):2888-97. doi: 10.1097/CCM.0b013e318186ba8c. Crit Care Med. 2008. PMID: 18766097 Review.
-
Supervision of Advanced Practice Providers.Emerg Med Clin North Am. 2020 May;38(2):353-361. doi: 10.1016/j.emc.2020.02.007. Emerg Med Clin North Am. 2020. PMID: 32336330 Review.
Cited by
-
Whole Health Revolution: Value-Based Care + Lifestyle Medicine.Am J Lifestyle Med. 2024 Apr 10;18(6):766-778. doi: 10.1177/15598276241241023. eCollection 2024 Nov-Dec. Am J Lifestyle Med. 2024. PMID: 39507921 Free PMC article. Review.
-
Visit and Between-Visit Interaction Frequency Before and After COVID-19 Telehealth Implementation.JAMA Netw Open. 2023 Sep 5;6(9):e2333944. doi: 10.1001/jamanetworkopen.2023.33944. JAMA Netw Open. 2023. PMID: 37713198 Free PMC article.
-
Forecasting the physician assistant/associate workforce: 2020-2035.Future Healthc J. 2022 Mar;9(1):57-63. doi: 10.7861/fhj.2021-0193. Future Healthc J. 2022. PMID: 35372769 Free PMC article.
-
Impact of primary care usual provider type and provider interdependence on outcomes for patients with diabetes: a cohort study.BMJ Open Qual. 2023 Jun;12(2):e002229. doi: 10.1136/bmjoq-2022-002229. BMJ Open Qual. 2023. PMID: 37311623 Free PMC article.
-
Physicians working with physician assistants and nurse practitioners: perceived effects on clinical practice.Health Aff Sch. 2024 Jun 25;2(6):qxae070. doi: 10.1093/haschl/qxae070. eCollection 2024 Jun. Health Aff Sch. 2024. PMID: 38919965 Free PMC article.
References
-
- HHS Secretary Azar’s March 24, 2020 Letter to Governors [Internet] [cited 2020 Aug 6]. Available from: https://www.nga.org/wp-content/uploads/2020/03/Governor-Letter-from-Azar...
-
- COVID-19 State Emergency Response: Temporarily Suspended and Waived Practice Agreement Requirements [Internet] AANP. [cited 2020 Aug 6]. Available from: https://www.aanp.org/advocacy/state/covid-19-state-emergency-response-te...
-
- COVID-19 State Emergency Response [Internet] AAPA. [cited 2020 Aug 6]. Available from: https://www.aapa.org/news-central/covid-19-resource-center/covid-19-stat...
-
- NP Scope of Practice Laws [Internet] Barton Associates. [cited 2020 Aug 6]. Available from: https://www.bartonassociates.com/locum-tenens-resources/nurse-practition...
-
- PA Scope of Practice Laws [Internet] Barton Associates. [cited 2020. Aug 6]. Available from: https://www.bartonassociates.com/locum-tenens-resources/pa-scope-of-prac...
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

