This is a preprint.
Multinational Prevalence of Neurological Phenotypes in Patients Hospitalized with COVID-19
- PMID: 33655281
- PMCID: PMC7924306
- DOI: 10.1101/2021.01.27.21249817
Multinational Prevalence of Neurological Phenotypes in Patients Hospitalized with COVID-19
Update in
-
Multinational characterization of neurological phenotypes in patients hospitalized with COVID-19.Sci Rep. 2021 Oct 12;11(1):20238. doi: 10.1038/s41598-021-99481-9. Sci Rep. 2021. PMID: 34642371 Free PMC article.
Abstract
Objective: Neurological complications can worsen outcomes in COVID-19. We defined the prevalence of a wide range of neurological conditions among patients hospitalized with COVID-19 in geographically diverse multinational populations.
Methods: Using electronic health record (EHR) data from 348 participating hospitals across 6 countries and 3 continents between January and September 2020, we performed a cross-sectional study of hospitalized adult and pediatric patients with a positive SARS-CoV-2 reverse transcription polymerase chain reaction test, both with and without severe COVID-19. We assessed the frequency of each disease category and 3-character International Classification of Disease (ICD) code of neurological diseases by countries, sites, time before and after admission for COVID-19, and COVID-19 severity.
Results: Among the 35,177 hospitalized patients with SARS-CoV-2 infection, there was increased prevalence of disorders of consciousness (5.8%, 95% confidence interval [CI]: 3.7%-7.8%, p FDR <.001) and unspecified disorders of the brain (8.1%, 95%CI: 5.7%-10.5%, p FDR <.001), compared to pre-admission prevalence. During hospitalization, patients who experienced severe COVID-19 status had 22% (95%CI: 19%-25%) increase in the relative risk (RR) of disorders of consciousness, 24% (95%CI: 13%-35%) increase in other cerebrovascular diseases, 34% (95%CI: 20%-50%) increase in nontraumatic intracranial hemorrhage, 37% (95%CI: 17%-60%) increase in encephalitis and/or myelitis, and 72% (95%CI: 67%-77%) increase in myopathy compared to those who never experienced severe disease.
Interpretation: Using an international network and common EHR data elements, we highlight an increase in the prevalence of central and peripheral neurological phenotypes in patients hospitalized with SARS-CoV-2 infection, particularly among those with severe disease.
Conflict of interest statement
Potential Conflicts of Interests
None.
Figures
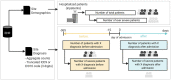



References
-
- Mahase E. Covid-19: WHO declares pandemic because of “alarming levels” of spread, severity, and inaction. BMJ 2020;368:m1036. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous
