Differential effect of malnutrition between patients hospitalized with new-onset heart failure and worsening of chronic heart failure
- PMID: 33655718
- PMCID: PMC8120416
- DOI: 10.1002/ehf2.13279
Differential effect of malnutrition between patients hospitalized with new-onset heart failure and worsening of chronic heart failure
Abstract
Aims: We aimed to investigate the differences in the prevalence, severity, and prognostic impact of malnutrition between patients with new-onset heart failure (HF) and worsening of chronic HF.
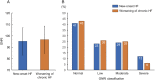
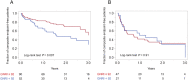
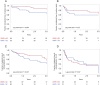
Methods and results: In older (≥60 years) hospitalized patients with acute HF, malnutrition was assessed according to the Geriatric Nutritional Risk Index (GNRI). A score <92 was defined as malnutrition. The primary endpoint was a composite endpoint, including cardiac death or rehospitalization for HF. Among 210 patients, 37% (52/142) of patients with new-onset HF and 31% (21/68) of patients with worsening of chronic HF had malnutrition (P = 0.41). The GNRI classification was comparable between the two groups. Kaplan-Meier analysis revealed a significant difference in the incidence of the composite endpoint in patients with new-onset HF (GNRI < 92 vs. GNRI ≥ 92: 50% vs. 32%, P = 0.007), but not in patients with worsening of chronic HF (GNRI < 92 vs. GNRI ≥ 92: 67% vs. 68%, P = 0.91). The adjusted Cox proportional hazards model demonstrated that a GNRI of <92 was an independent prognostic factor for the composite endpoint in patients with new-onset HF only.
Conclusions: Among older hospitalized patients with acute HF, the prevalence and severity of malnutrition were comparable between the two categories of patients. Malnutrition was an independent prognostic factor in patients with new-onset HF, while clinical prognosis was poor in patients with worsening of HF, irrespective of malnutrition. The prognostic impact of malnutrition differs between new-onset HF and worsening of chronic HF.
Keywords: Acute heart failure; Geriatric Nutritional Risk Index; New-onset heart failure; Worsening of chronic heart failure.
© 2021 The Authors. ESC Heart Failure published by John Wiley & Sons Ltd on behalf of European Society of Cardiology.
Conflict of interest statement
None declared.
Figures
Similar articles
-
Prevalence and prognostic implications of malnutrition as defined by GLIM criteria in elderly patients with heart failure.Clin Nutr. 2021 Jun;40(6):4334-4340. doi: 10.1016/j.clnu.2021.01.014. Epub 2021 Jan 22. Clin Nutr. 2021. PMID: 33551220
-
Geriatric nutritional risk index as a nutritional and survival risk assessment tool in stable outpatients with systolic heart failure.Nutr Metab Cardiovasc Dis. 2017 May;27(5):430-437. doi: 10.1016/j.numecd.2017.02.003. Epub 2017 Feb 22. Nutr Metab Cardiovasc Dis. 2017. PMID: 28438373
-
Prognostic impact of nutrition measures in patients with heart failure varies with coexisting physical frailty.ESC Heart Fail. 2023 Dec;10(6):3364-3372. doi: 10.1002/ehf2.14519. Epub 2023 Sep 7. ESC Heart Fail. 2023. PMID: 37675757 Free PMC article.
-
Geriatric nutritional risk index predicts all-cause mortality in patients with heart failure: A systematic review and meta-analysis.Clinics (Sao Paulo). 2021 Mar 24;76:e2258. doi: 10.6061/clinics/2021/e2258. eCollection 2021. Clinics (Sao Paulo). 2021. PMID: 33787674 Free PMC article.
-
Potential association with malnutrition and allocation of combination medical therapies in hospitalized heart failure patients with reduced ejection fraction.Sci Rep. 2022 May 18;12(1):8318. doi: 10.1038/s41598-022-12357-4. Sci Rep. 2022. PMID: 35585128 Free PMC article. Review.
Cited by
-
Association Between Prognostic Nutritional Index and Prognosis in Patients With Heart Failure: A Meta-Analysis.Front Cardiovasc Med. 2022 Jun 10;9:918566. doi: 10.3389/fcvm.2022.918566. eCollection 2022. Front Cardiovasc Med. 2022. PMID: 35757355 Free PMC article.
-
Diet in Scleroderma: Is There a Need for Intervention?Diagnostics (Basel). 2021 Nov 15;11(11):2118. doi: 10.3390/diagnostics11112118. Diagnostics (Basel). 2021. PMID: 34829464 Free PMC article.
-
Prognostic value of geriatric nutritional risk index for aspiration pneumonia: a retrospective observational cohort study.Aging Clin Exp Res. 2022 Mar;34(3):563-571. doi: 10.1007/s40520-021-01948-2. Epub 2021 Aug 11. Aging Clin Exp Res. 2022. PMID: 34379292
-
Effectiveness of Guideline-Directed Medical Therapy for Acute Heart Failure With Reduced Ejection Fraction in Frail Elderly Patients With Malnutrition.Circ Rep. 2025 Feb 28;7(4):267-274. doi: 10.1253/circrep.CR-25-0003. eCollection 2025 Apr 10. Circ Rep. 2025. PMID: 40213803 Free PMC article.
-
Factors associated with poor prognosis in elderly patients with congestive heart failure with comorbid cognitive impairment: impact of life circumstances.J Geriatr Cardiol. 2025 May 28;22(6):603-608. doi: 10.26599/1671-5411.2025.06.007. J Geriatr Cardiol. 2025. PMID: 40636552 Free PMC article. No abstract available.
References
-
- GBD 2017 Disease and Injury Incidence and Prevalence Collaborators . Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018; 392: 1789–1858. - PMC - PubMed
-
- Mamas MA, Sperrin M, Watson MC, Coutts A, Wilde K, Burton C, Kadam UT, Kwok CS, Clark AB, Murchie P, Buchan I, Hannaford PC, Myint PK. Do patients have worse outcomes in heart failure than in cancer? A primary care‐based cohort study with 10‐year follow‐up in Scotland. Eur J Heart Fail 2017; 19: 1095–1104. - PubMed
-
- Greene SJ, Hernandez AF, Dunning A, Ambrosy AP, Armstrong PW, Butler J, Cerbin LP, Coles A, Ezekowitz JA, Metra M, Starling RC, Teerlink JR, Voors AA, O'Connor CM, Mentz RJ. Hospitalization for recently diagnosed versus worsening chronic heart failure: from the ASCEND‐HF trial. J Am Coll Cardiol 2017; 69: 3029–3039. - PubMed
-
- Butt JH, Fosbøl EL, Gerds TA, Andersson C, McMurray JJV, Petrie MC, Gustafsson F, Madelaire C, Kristensen SL, Gislason GH, Torp‐Pedersen C, Køber L, Schou M. Readmission and death in patients admitted with new‐onset versus worsening of chronic heart failure: insights from a nationwide cohort. Eur J Heart Fail 2020; 22: 1777–1785. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

