Association between cumulative blood pressure and long-term risk of cardiovascular disease: findings from the 26-year Chinese Multi-provincial Cohort Study-Beijing Project
- PMID: 33655897
- PMCID: PMC8078343
- DOI: 10.1097/CM9.0000000000001383
Association between cumulative blood pressure and long-term risk of cardiovascular disease: findings from the 26-year Chinese Multi-provincial Cohort Study-Beijing Project
Abstract
Background: Cumulative blood pressure (BP), a measure incorporating the level and duration of BP exposure, is associated with the risk of cardiovascular disease (CVD). However, the level at which cumulative BP could significantly increase the risk remains unclear. This study aimed to investigate the association of 15-year cumulative BP levels with the long-term risk of CVD, and to examine whether the association is independent of BP levels at one examination.
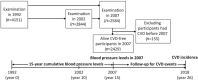
Methods: Data from a 26-year follow-up of the Chinese Multi-provincial Cohort Study-Beijing Project were analyzed. Cumulative BP levels between 1992 and 2007 were calculated among 2429 participants free of CVD in 2007. Cardiovascular events (including coronary heart disease and stroke) occurring from 2007 to 2018 were registered. Adjusted hazard ratios (HRs) for CVD incidence associated with quartiles of cumulative systolic blood pressure (SBP) and diastolic blood pressure (DBP) were calculated.
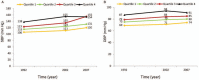
Results: Of the 2429 participants, 42.9% (1042) were men, and the mean age in 2007 was 62.1 ± 7.9 years. Totally, 207 CVD events occurred during the follow-up from 2007 to 2018. Participants with higher levels of cumulative SBP or DBP exhibited a higher incidence rate of CVD (P < 0.001). Compared with the lowest quartile of cumulative SBP, the HR for CVD was 1.03 (95% confidence interval [CI]: 0.59-1.81), 1.69 (95% CI: 0.99-2.87), and 2.20 (95% CI: 1.21-3.98) for the second to the fourth quartile of cumulative SBP, and 1.46 (95% CI: 0.86-2.48), 1.99 (95% CI: 1.18-3.35), and 2.08 (95% CI: 1.17-3.71) for the second to the fourth quartile of cumulative DBP, respectively. In further cross-combined group analyses with BP measurements in 2007, 15-year cumulative BP levels higher than the median, that is, 1970.8/1239.9 mmHg·year for cumulative SBP/DBP, which were equivalent to maintaining SBP/DBP levels of 131/83 mmHg or above on average in 15 years, were associated with higher risk of CVD in subsequent years independent of BP measurements at one-time point.
Conclusion: Cumulative exposure to moderate elevation of BP is independently associated with increased future cardiovascular risk.
Copyright © 2021 The Chinese Medical Association, produced by Wolters Kluwer, Inc. under the CC-BY-NC-ND license.
Conflict of interest statement
None.
Figures

References
-
- GBD 2017 Risk Factor Collaborators. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990-2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018; 392:1923–1994. doi: 10.1016/S0140-6736(18)32225-6. - PMC - PubMed
-
- Lewington S, Clarke R, Qizilbash N, Peto R, Collins R. Prospective Studies Collaboration. Age-specific relevance of usual blood pressure to vascular mortality: A meta-analysis of individual data for one million adults in 61 prospective studies. Lancet 2002; 360:1903–1913. doi: 10.1016/s0140-6736(02)11911-8. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

