Posterior Circulation Endovascular Thrombectomy for Large-Vessel Occlusion: Predictors of Favorable Clinical Outcome and Analysis of First-Pass Effect
- PMID: 33664106
- PMCID: PMC8115369
- DOI: 10.3174/ajnr.A7023
Posterior Circulation Endovascular Thrombectomy for Large-Vessel Occlusion: Predictors of Favorable Clinical Outcome and Analysis of First-Pass Effect
Abstract
Background and purpose: Successful vessel recanalization in posterior circulation large-vessel occlusion is considered crucial, though the evidence of clinical usefulness, compared with the anterior circulation, is not still determined. The aim of this study was to evaluate predictors of favorable clinical outcome and to analyze the effect of first-pass thrombectomy.
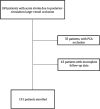
Materials and methods: A retrospective, multicenter, observational study was conducted in 10 high-volume stroke centers in Europe, including the period from January 2016 to July 2019. Only patients with an acute basilar artery occlusion or a single, dominant vertebral artery occlusion ("functional" basilar artery occlusion) who had a 3-month mRS were included. Clinical, procedural, and radiologic data were evaluated, and the association between these parameters and both the functional outcome and the first-pass effect was assessed.
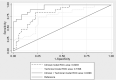
Results: A total of 191 patients were included. A lower baseline NIHSS score (adjusted OR, 0.77; 95% CI, 0.61-0.96; P = .025) and higher baseline MR imaging posterior circulation ASPECTS (adjusted OR, 3.01; 95% CI, 1.03-8.76; P = .043) were predictors of better outcomes. The use of large-bore catheters (adjusted OR, 2.25; 95% CI, 1.08-4.67; P = .030) was a positive predictor of successful reperfusion at first-pass, while the use of a combined technique was a negative predictor (adjusted OR, 0.26; 95% CI, 0.09-0.76; P = .014).
Conclusions: The analysis of our retrospective series demonstrates that a lower baseline NIHSS score and a higher MR imaging posterior circulation ASPECTS were predictors of good clinical outcome. The use of large-bore catheters was a positive predictor of first-pass modified TICI 2b/3; the use of a combined technique was a negative predictor.
© 2021 by American Journal of Neuroradiology.
Figures


Similar articles
-
Mechanical thrombectomy in basilar artery occlusion: influence of reperfusion on clinical outcome and impact of the first-line strategy (ADAPT vs stent retriever).J Neurosurg. 2018 Dec 1;129(6):1482-1491. doi: 10.3171/2017.7.JNS171043. Epub 2018 Jan 12. J Neurosurg. 2018. PMID: 29327997
-
Revascularization Techniques for Acute Basilar Artery Occlusion : Technical Considerations and Outcome in the Setting of Severe Posterior Circulation Steno-Occlusive Disease.Clin Neuroradiol. 2019 Sep;29(3):435-443. doi: 10.1007/s00062-018-0683-3. Epub 2018 Apr 12. Clin Neuroradiol. 2019. PMID: 29651586
-
Predictors of Favorable Outcome after Endovascular Thrombectomy in MRI: Selected Patients with Acute Basilar Artery Occlusion.AJNR Am J Neuroradiol. 2020 Sep;41(9):1670-1676. doi: 10.3174/ajnr.A6741. Epub 2020 Aug 20. AJNR Am J Neuroradiol. 2020. PMID: 32819893 Free PMC article.
-
Predictors of first pass effect and effect on outcomes in mechanical thrombectomy for basilar artery occlusion.J Clin Neurosci. 2022 Aug;102:49-53. doi: 10.1016/j.jocn.2022.06.005. Epub 2022 Jun 17. J Clin Neurosci. 2022. PMID: 35724438 Review.
-
Focused update to guidelines for endovascular therapy for emergent large vessel occlusion: basilar artery occlusion patients.J Neurointerv Surg. 2024 Jul 16;16(8):752-755. doi: 10.1136/jnis-2024-021705. J Neurointerv Surg. 2024. PMID: 38670791 Review.
Cited by
-
Efficacy of Mechanical Thrombectomy using Penumbra ACETM Aspiration Catheter Compared to Stent Retriever SolitaireTM FR in Patients with Acute Ischemic Stroke.Brain Sci. 2021 Apr 16;11(4):504. doi: 10.3390/brainsci11040504. Brain Sci. 2021. PMID: 33923489 Free PMC article.
-
Revascularization Outcome Prediction for A Direct Aspiration-First Pass Technique (ADAPT) from Pre-Treatment Imaging and Machine Learning.Brain Sci. 2021 Oct 5;11(10):1321. doi: 10.3390/brainsci11101321. Brain Sci. 2021. PMID: 34679386 Free PMC article.
-
Prevalence and Associated Factors of Cognitive Impairment Among Stroke Survivors at Comprehensive Specialized Hospitals in Northwest Ethiopia: Multi-Centered Cross-Sectional Study.Vasc Health Risk Manag. 2023 Apr 27;19:265-277. doi: 10.2147/VHRM.S405357. eCollection 2023. Vasc Health Risk Manag. 2023. PMID: 37138791 Free PMC article.
-
What You Always Wanted to Know about Endovascular Therapy in Acute Ischemic Stroke but Never Dared to Ask: A Comprehensive Review.Rev Cardiovasc Med. 2022 Oct 11;23(10):340. doi: 10.31083/j.rcm2310340. eCollection 2022 Oct. Rev Cardiovasc Med. 2022. PMID: 39077121 Free PMC article. Review.
-
A Predictive Model for the Risk of Posterior Circulation Stroke in Patients with Intracranial Atherosclerosis Based on High Resolution MRI.Diagnostics (Basel). 2022 Mar 15;12(4):812. doi: 10.3390/diagnostics12040812. Diagnostics (Basel). 2022. PMID: 35453860 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
