Impact of a poor functional capacity on the clinical outcomes in patients with a pacemaker implantation -Results from the Japanese Heart Rhythm Society Registry
- PMID: 33664901
- PMCID: PMC7896460
- DOI: 10.1002/joa3.12459
Impact of a poor functional capacity on the clinical outcomes in patients with a pacemaker implantation -Results from the Japanese Heart Rhythm Society Registry
Abstract
Background: Functional capacity (FC) correlates with mortality in various cardiovascular diseases. The aim of this study was to examine whether cardiac pacemaker implantations improve the FC and affect the prognosis.
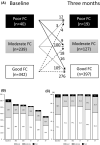
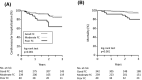
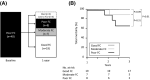
Methods and results: We prospectively enrolled 621 de novo pacemaker recipients (age 76 ± 9 years, 50.7% male). The FC was assessed by metabolic equivalents (METs) during the implantation and periodically thereafter. The patients were a priori classified into poor FC (<2 METs, n = 40), moderate FC (2 ≤ METs < 4, n = 239), and good FC (≥4 METs, n = 342). Three months after the pacemaker implantation, poor FC or moderate FC patients improved to a good FC by 43%. The distribution of the three FCs remained at those levels until after 1 year of follow-up (P = .18). During a median follow-up of 2.4 years, 71 patients (11%) had cardiovascular hospitalizations and 35 (5.6%) all-cause death. A multivariate Cox analysis revealed that a poor FC at baseline was an independent predictor of both cardiovascular hospitalization (hazard ratio [HR] 2.494, P = .012) and all-cause death (HR 3.338, P = .016). One year after the pacemaker implantation, the eight who remained with a poor FC had a high mortality rate of 37.5% (P < .01).
Conclusion: Approximately half of the poor or moderate FC patients improved to good FC 3 months after the pacemaker implantation. The baseline FC predicted the prognosis, and patients with an improved FC after the pacemaker implantation had a better prognosis.
Keywords: functional capacity; pacemaker; prognosis.
© 2020 The Authors. Journal of Arrhythmia published by John Wiley & Sons Australia, Ltd on behalf of the Japanese Heart Rhythm Society.
Conflict of interest statement
EW received a lecture fee from Biotronik Japan, Daiichi‐Sankyo, and Pfizer. RK has an affiliation with the endowed departments of Boston Scientific and Abbott. AN received a lecture fee from Daiichi‐Sankyo and has an affiliation with the endowed department of Boston Scientific and Abbott. KO received a lecture fee from Johnson and Johnson, Medtronic, Daiichi‐Sankyo, and Boehringer‐Ingelheim. None of the other authors have conflicts of interest.
Figures
Similar articles
-
Biventricular pacing (cardiac resynchronization therapy): an evidence-based analysis.Ont Health Technol Assess Ser. 2005;5(13):1-60. Epub 2005 Sep 1. Ont Health Technol Assess Ser. 2005. PMID: 23074464 Free PMC article.
-
Baseline functional capacity and the benefit of cardiac resynchronization therapy in patients with mildly symptomatic heart failure enrolled in MADIT-CRT.Heart Rhythm. 2012 Sep;9(9):1454-9. doi: 10.1016/j.hrthm.2012.04.018. Epub 2012 Apr 17. Heart Rhythm. 2012. PMID: 22521920
-
Prior Pacemaker Implantation and Clinical Outcomes in Patients With Heart Failure and Preserved Ejection Fraction.JACC Heart Fail. 2019 May;7(5):418-427. doi: 10.1016/j.jchf.2018.12.006. Epub 2019 Apr 10. JACC Heart Fail. 2019. PMID: 30981744
-
Association of Clinical and Economic Outcomes With Permanent Pacemaker Implantation After Transcatheter Aortic Valve Replacement.JAMA Netw Open. 2018 May 18;1(1):e180088. doi: 10.1001/jamanetworkopen.2018.0088. JAMA Netw Open. 2018. PMID: 30646053 Free PMC article.
-
Pacing burden and clinical outcomes after transcatheter aortic valve replacement-A real-world registry report.Heart Rhythm. 2022 Sep;19(9):1508-1515. doi: 10.1016/j.hrthm.2022.04.030. Epub 2022 May 4. Heart Rhythm. 2022. PMID: 35525423
Cited by
-
A survey of the implementation rate of cardiac rehabilitation for patients with heart disease undergoing device implantation in Japan.J Arrhythm. 2022 Oct 26;38(6):1049-1055. doi: 10.1002/joa3.12792. eCollection 2022 Dec. J Arrhythm. 2022. PMID: 36524042 Free PMC article.
References
-
- Epstein AE, DiMarco JP, Ellenbogen KA, Estes NA 3rd, Freedman RA, Gettes LS, et al. ACC/AHA/HRS 2008 Guidelines for Device‐Based Therapy of Cardiac Rhythm Abnormalities: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the ACC/AHA/NASPE 2002 Guideline Update for Implantation of Cardiac Pacemakers and Antiarrhythmia Devices): developed in collaboration with the American Association for Thoracic Surgery and Society of Thoracic Surgeons. Circulation. 2008;117:e350–e408. - PubMed
-
- Toff WD, Camm AJ, Skehan JD; United Kingdom Pacing and Cardiovascular Events Trial Investigators . Single‐chamber versus dual‐chamber pacing for high‐grade atrioventricular block. N Engl J Med. 2005;353:145–55. - PubMed
-
- Andersen HR, Nielsen JC, Thomsen PEB, Thuesen L, Mortensen PT, Vesterlund T, et al. Long‐term follow‐up of patients from a randomised trial of atrial versus ventricular pacing for sick‐sinus syndrome. Lancet. 1997;350:1210–6. - PubMed
-
- Tsutsui H, Isobe M, Ito H, Okumura K, Ono M, Kitakaze M, et al. JCS 2017/JHFS 2017 guideline on diagnosis and treatment of acute and chronic heart failure‐ digest version. Circ J. 2019;83:2084–184. - PubMed
-
- Kamiya K, Yamamoto T, Tsuchihashi‐Makaya M, Ikegame T, Takahashi T, Sato Y, et al. Nationwide survey of multidisciplinary care and cardiac rehabilitation for patients with heart failure in Japan ‐ an analysis of the AMED‐CHF study. Circ J. 2019;83:1546–52. - PubMed
LinkOut - more resources
Full Text Sources

