Synergistic Killing and Re-Sensitization of Pseudomonas aeruginosa to Antibiotics by Phage-Antibiotic Combination Treatment
- PMID: 33668899
- PMCID: PMC7996583
- DOI: 10.3390/ph14030184
Synergistic Killing and Re-Sensitization of Pseudomonas aeruginosa to Antibiotics by Phage-Antibiotic Combination Treatment
Abstract
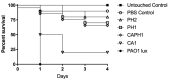
Multidrug-resistant (MDR) Pseudomonas aeruginosa infections pose a serious health threat. Bacteriophage-antibiotic combination therapy is a promising candidate for combating these infections. A 5-phage P. aeruginosa cocktail, PAM2H, was tested in combination with antibiotics (ceftazidime, ciprofloxacin, gentamicin, meropenem) to determine if PAM2H enhances antibiotic activity. Combination treatment in vitro resulted in a significant increase in susceptibility of MDR strains to antibiotics. Treatment with ceftazidime (CAZ), meropenem, gentamicin, or ciprofloxacin in the presence of the phage increased the number of P. aeruginosa strains susceptible to these antibiotics by 63%, 56%, 31%, and 81%, respectively. Additionally, in a mouse dorsal wound model, seven of eight mice treated with a combination of CAZ and PAM2H for three days had no detectable bacteria remaining in their wounds on day 4, while all mice treated with CAZ or PAM2H alone had ~107 colony forming units (CFU) remaining in their wounds. P. aeruginosa recovered from mouse wounds post-treatment showed decreased virulence in a wax worm model, and DNA sequencing indicated that the combination treatment prevented mutations in genes encoding known phage receptors. Treatment with PAM2H in combination with antibiotics resulted in the re-sensitization of P. aeruginosa to antibiotics in vitro and a synergistic reduction in bacterial burden in vivo.
Keywords: Pseudomonas aeruginosa; antimicrobial resistance; phage therapy; phage–antibiotic synergy; re-sensitization.
Conflict of interest statement
The authors declare no conflict of interest.
Figures




References
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

