Risk of Insulin Resistance and Metabolic Syndrome in Women with Hyperandrogenemia: A Comparison between PCOS Phenotypes and Beyond
- PMID: 33670546
- PMCID: PMC7922675
- DOI: 10.3390/jcm10040829
Risk of Insulin Resistance and Metabolic Syndrome in Women with Hyperandrogenemia: A Comparison between PCOS Phenotypes and Beyond
Abstract
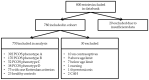
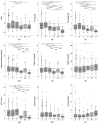
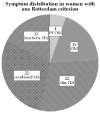
Polycystic ovary syndrome (PCOS) is the most common endocrine disorder in premenopausal women, with a wide spectrum of possible phenotypes, symptoms and sequelae according to the current clinical definition. However, there are women who do not fulfill at least two out of the three commonly used "Rotterdam criteria" and their risk of developing type 2 diabetes or obesity later in life is not defined. Therefore, we addressed this important gap by conducting a retrospective analysis based on 750 women with and without PCOS. We compared four different PCOS phenotypes according to the Rotterdam criteria with women who exhibit only one Rotterdam criterion and with healthy controls. Hormone and metabolic differences were assessed by analysis of variance (ANOVA) as well as logistic regression analysis. We found that hyperandrogenic women have per se a higher risk of developing insulin resistance compared to phenotypes without hyperandrogenism and healthy controls. In addition, hyperandrogenemia is associated with developing insulin resistance also in women with no other Rotterdam criterion. Our study encourages further diagnostic and therapeutic approaches for PCOS phenotypes in order to account for varying risks of developing metabolic diseases. Finally, women with hyperandrogenism as the only symptom should also be screened for insulin resistance to avoid later metabolic risks.
Keywords: PCOS; Rotterdam criteria; free testosterone; hyperandrogenism; insulin resistance.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures
Similar articles
-
Controversy in clinical endocrinology: diagnosis of polycystic ovarian syndrome: the Rotterdam criteria are premature.J Clin Endocrinol Metab. 2006 Mar;91(3):781-5. doi: 10.1210/jc.2005-2153. Epub 2006 Jan 17. J Clin Endocrinol Metab. 2006. PMID: 16418211
-
The Prevalence of Polycystic Ovary Syndrome, Its Phenotypes and Cardio-Metabolic Features in a Community Sample of Iranian Population: Tehran Lipid and Glucose Study.Front Endocrinol (Lausanne). 2022 Mar 1;13:825528. doi: 10.3389/fendo.2022.825528. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 35299965 Free PMC article.
-
A case-control observational study of insulin resistance and metabolic syndrome among the four phenotypes of polycystic ovary syndrome based on Rotterdam criteria.Reprod Health. 2015 Jan 16;12:7. doi: 10.1186/1742-4755-12-7. Reprod Health. 2015. PMID: 25595199 Free PMC article.
-
Metabolic syndrome and its components in different phenotypes of polycystic ovary syndrome.Diabetes Metab Res Rev. 2022 Jan;38(1):e3464. doi: 10.1002/dmrr.3464. Epub 2021 May 14. Diabetes Metab Res Rev. 2022. PMID: 33988288 Review.
-
Polycystic Ovary Syndrome: A Contemporary Clinical Approach.Curr Pharm Des. 2021;27(36):3812-3820. doi: 10.2174/1381612827666210119104721. Curr Pharm Des. 2021. PMID: 33463457 Review.
Cited by
-
Atherogenic Index of Plasma in Metabolic Syndrome-A Systematic Review and Meta-Analysis.Medicina (Kaunas). 2025 Mar 27;61(4):611. doi: 10.3390/medicina61040611. Medicina (Kaunas). 2025. PMID: 40282902 Free PMC article.
-
Integrative regression modeling of insulin sensitivity, resistance, and beta-cell dysfunction in predicting female infertility: a cross-sectional NHANES study.Clin Exp Med. 2025 Jun 30;25(1):224. doi: 10.1007/s10238-025-01755-3. Clin Exp Med. 2025. PMID: 40586983 Free PMC article.
-
Lean mass and associated factors in women with PCOS with different phenotypes.PLoS One. 2023 Oct 5;18(10):e0292623. doi: 10.1371/journal.pone.0292623. eCollection 2023. PLoS One. 2023. PMID: 37796920 Free PMC article.
-
Polycystic Ovary Syndrome: Past, Present and Future.J Clin Med. 2023 Jun 1;12(11):3808. doi: 10.3390/jcm12113808. J Clin Med. 2023. PMID: 37298003 Free PMC article.
-
Therapeutic Potential of Selenium Nanoparticles on Letrozole-Induced Polycystic Ovarian Syndrome in Female Wistar Rats.Biol Trace Elem Res. 2023 Nov;201(11):5213-5229. doi: 10.1007/s12011-023-03579-2. Epub 2023 Jan 25. Biol Trace Elem Res. 2023. PMID: 36694071
References
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

