Challenges and Innovations in Osteochondral Regeneration: Insights from Biology and Inputs from Bioengineering toward the Optimization of Tissue Engineering Strategies
- PMID: 33673516
- PMCID: PMC7931100
- DOI: 10.3390/jfb12010017
Challenges and Innovations in Osteochondral Regeneration: Insights from Biology and Inputs from Bioengineering toward the Optimization of Tissue Engineering Strategies
Abstract
Due to the extremely high incidence of lesions and diseases in aging population, it is critical to put all efforts into developing a successful implant for osteochondral tissue regeneration. Many of the patients undergoing surgery present osteochondral fissure extending until the subchondral bone (corresponding to a IV grade according to the conventional radiographic classification by Berndt and Harty). Therefore, strategies for functional tissue regeneration should also aim at healing the subchondral bone and joint interface, besides hyaline cartilage. With the ambition of contributing to solving this problem, several research groups have been working intensively on the development of tailored implants that could promote that complex osteochondral regeneration. These implants may be manufactured through a wide variety of processes and use a wide variety of (bio)materials. This review aimed to examine the state of the art regarding the challenges, advantages, and drawbacks of the current strategies for osteochondral regeneration. One of the most promising approaches relies on the principles of additive manufacturing, where technologies are used that allow for the production of complex 3D structures with a high level of control, intended and predefined geometry, size, and interconnected pores, in a reproducible way. However, not all materials are suitable for these processes, and their features should be examined, targeting a successful regeneration.
Keywords: additive manufacturing; biomaterials; hyaline cartilage; regenerative medicine; subchondral bone; tissue engineering.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
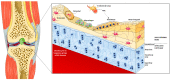
References
-
- Bryant S.J., Davis-Arehart K.A., Luo N., Shoemaker R.K., Arthur J.A., Anseth K.S. Synthesis and characterization of photopolymerized multifunctional hydrogels: Water-soluble poly (vinyl alcohol) and chondroitin sulfate macromers for chondrocyte encapsulation. Macromolecules. 2004;37:6726–6733. doi: 10.1021/ma0499324. - DOI
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

