Prevalence and clinical, social, and health care predictors of miscarriage
- PMID: 33673832
- PMCID: PMC7936485
- DOI: 10.1186/s12884-021-03682-z
Prevalence and clinical, social, and health care predictors of miscarriage
Abstract
Background: Pregnancy loss is common and several factors (e.g. chromosomal anomalies, parental age) are known to increase the risk of occurrence. However, much existing research focuses on recurrent loss; comparatively little is known about the predictors of a first miscarriage. Our objective was to estimate the population-level prevalence of miscarriages and to assess the contributions of clinical, social, and health care use factors as predictors of the first detected occurrence of these losses.
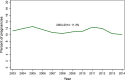
Methods: In this population-based cohort study, we used linked administrative health data to estimate annual rates of miscarriage in the Manitoba population from 2003 to 2014, as a share of identified pregnancies. We compared the unadjusted associations between clinical, social, and health care use factors and first detected miscarriage compared with a live birth. We estimated multivariable generalized linear models to assess whether risk factors were associated with first detected miscarriage controlling for other predictors.
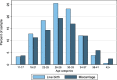
Results: We estimated an average annual miscarriage rate of 11.3%. In our final sample (n = 79,978 women), the fully-adjusted model indicated that use of infertility drugs was associated with a 4 percentage point higher risk of miscarriage (95% CI 0.02, 0.06) and a past suicide attempt with a 3 percentage point higher risk (95% CI -0.002, 0.07). Women with high morbidity were twice as likely to experience a miscarriage compared to women with low morbidity (RD = 0.12, 95% CI 0.09, 0.15). Women on income assistance had a 3 percentage point lower risk (95% CI -0.04, -0.02).
Conclusions: We estimate that 1 in 9 pregnant women in Manitoba experience and seek care for a miscarriage. After adjusting for clinical factors, past health care use and morbidity contribute important additional information about the risk of first detected miscarriage. Social factors may also be informative.
Keywords: Health services; Manitoba; Miscarriage; Women’s health.
Conflict of interest statement
Not applicable
Figures
References
-
- Macklon NS, Geraedts JP, Fauser BC. Conception to ongoing pregnancy: the ‘black box’of early pregnancy loss. Human reproduction update. 2002;8(4):333–43. - PubMed
-
- National Collaborating Centre for Women's and Children's Health (UK). Ectopic Pregnancy and Miscarriage: Diagnosis and Initial Management in EarlyPregnancy of Ectopic Pregnancy and Miscarriage. London: RCOG; 2012. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous