Prevalence of Sleep Disturbances and Sleep Quality in Chinese Healthcare Workers During the COVID-19 Pandemic: A Systematic Review and Meta-Analysis
- PMID: 33679493
- PMCID: PMC7930820
- DOI: 10.3389/fpsyt.2021.646342
Prevalence of Sleep Disturbances and Sleep Quality in Chinese Healthcare Workers During the COVID-19 Pandemic: A Systematic Review and Meta-Analysis
Abstract
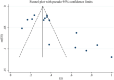
Objectives: Healthcare workers (HWs) experienced high levels of work stress during the COVID-19 pandemic, leading to a high risk of sleep disturbances. This meta-analysis aimed to explore the prevalence of sleep disturbances and sleep quality in Chinese HWs during the COVID-19 pandemic. Methods: English (PubMed, EMBASE, PsycINFO, Web of Science, and the Cochrane Library) and Chinese databases (WanFang, Chinese National Knowledge Infrastructure, and SinoMed) were systematically and independently searched for relevant studies published from December 1, 2019, to May 20, 2020. The pooled prevalence of sleep disturbances and sleep quality were calculated using a random-effects model. Results: A total of 17 studies involving 12,682 Chinese HWs were included in the meta-analysis. The pooled prevalence of sleep disturbances in Chinese HWs was 45.1% (95% CI: 37.2-53.1%). We found that the prevalence of sleep disturbances varied among frontline, infected, and non-frontline HWs (Q = 96.96, p < 0.001); females and males (Q = 9.10, p = 0.003); studies using different assessment instruments (Q = 96.05, p < 0.001); and studies with different sample sizes (Q = 5.77, p = 0.016) and cut-off values (Q = 62.28, p < 0.001). The pooled mean total score of the Pittsburgh Sleep Quality Index (PSQI) was 9.83 (95% CI: 8.61-11.04). HWs in Wuhan had a higher total PSQI score than those in other regions (Q = 9.21, p = 0.002). Conclusion: Sleep disturbances were common in Chinese HWs during the COVID-19 pandemic, particularly in frontline and infected HWs. Our results indicate the heavy mental health burden on HWs during the COVID-19 pandemic in China and can provide other countries with valuable information to assist HWs during the crisis.
Keywords: COVID-19; China; healthcare workers; meta-analysis; sleep disturbances.
Copyright © 2021 Xia, Chen, Liu, Luo, Guo, Liu, Zhang and Liu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Immediate Psychosocial Impact on Healthcare Workers During COVID-19 Pandemic in China: A Systematic Review and Meta-Analysis.Front Psychol. 2021 May 28;12:645460. doi: 10.3389/fpsyg.2021.645460. eCollection 2021. Front Psychol. 2021. PMID: 34122233 Free PMC article.
-
The Prevalence of Sleep Disturbances and Sleep Quality in Older Chinese Adults: A Comprehensive Meta-Analysis.Behav Sleep Med. 2019 Nov-Dec;17(6):683-697. doi: 10.1080/15402002.2018.1469492. Epub 2018 May 31. Behav Sleep Med. 2019. PMID: 29851516
-
Prevalence of sleep disturbances in Chinese healthcare professionals: a systematic review and meta-analysis.Sleep Med. 2020 Mar;67:258-266. doi: 10.1016/j.sleep.2019.01.047. Epub 2019 Mar 6. Sleep Med. 2020. PMID: 31040078
-
Prevalence of sleep disturbances in Chinese adolescents: A systematic review and meta-analysis.PLoS One. 2021 Mar 4;16(3):e0247333. doi: 10.1371/journal.pone.0247333. eCollection 2021. PLoS One. 2021. PMID: 33661914 Free PMC article.
-
Prevalence of sleep disturbances in Chinese university students: a comprehensive meta-analysis.J Sleep Res. 2018 Jun;27(3):e12648. doi: 10.1111/jsr.12648. Epub 2018 Jan 31. J Sleep Res. 2018. PMID: 29383787 Review.
Cited by
-
Prevalence and influencing factors of sleep disturbance among medical students under the COVID-19 pandemic.Eur Arch Psychiatry Clin Neurosci. 2025 Feb;275(1):89-98. doi: 10.1007/s00406-023-01707-6. Epub 2023 Nov 26. Eur Arch Psychiatry Clin Neurosci. 2025. PMID: 38007404
-
Subjective sleep alterations in healthy subjects worldwide during COVID-19 pandemic: A systematic review, meta-analysis and meta-regression.Sleep Med. 2022 Dec;100:89-102. doi: 10.1016/j.sleep.2022.07.012. Epub 2022 Aug 10. Sleep Med. 2022. PMID: 36029756 Free PMC article.
-
Relationship of Problematic Smartphone Use, Sleep Quality, and Daytime Fatigue Among Quarantined Medical Students During the COVID-19 Pandemic.Front Psychiatry. 2021 Nov 10;12:755059. doi: 10.3389/fpsyt.2021.755059. eCollection 2021. Front Psychiatry. 2021. PMID: 34858229 Free PMC article.
-
The prevalence and severity of insomnia symptoms during COVID-19: A global systematic review and individual participant data meta-analysis.Sleep Med. 2022 Dec;100:7-23. doi: 10.1016/j.sleep.2022.06.020. Epub 2022 Aug 8. Sleep Med. 2022. PMID: 36030616 Free PMC article.
-
Sleep quality and associated factors in the context of COVID-19, among prehospital emergency personnel, in North-Eastern Greece.Hippokratia. 2021 Jul-Sep;25(3):126-133. Hippokratia. 2021. PMID: 36683904 Free PMC article.
References
-
- WHO . Coronavirus disease 2019 (COVID-19) Situation Report-132. Geneva: World Health Organization; (2020). Available online at: https://www.who.int/docs/default-source/coronaviruse/situation-reports/2... (accessed August 25, 2020).
-
- Beijing Daily. A Total of 3387 Medical Workers were Infected With COVID-19 in China. (2020). Available online at: https://baijiahao.baidu.com/s?id=1659420394069577730&wfr=spider&for=pc (accessed September 1, 2020).
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources