Short- and long-term outcomes of self-expanding metallic stent placement vs. emergency surgery for malignant colorectal obstruction
- PMID: 33680454
- PMCID: PMC7890458
- DOI: 10.3892/mco.2021.2225
Short- and long-term outcomes of self-expanding metallic stent placement vs. emergency surgery for malignant colorectal obstruction
Abstract
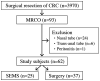
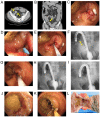
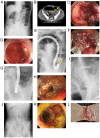
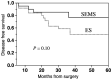
The European Society of Gastrointestinal Endoscopy does not recommend self-expanding metal stent (SEMS) placement as a bridge to surgery (BTS) for malignant colorectal obstruction (MCRO). However, no universally accepted consensus has been determined. The present study aimed to evaluate the short- and long-term outcomes of SEMS placement vs. emergency surgery (ES) for MCRO. Surgical resection of colorectal cancer was performed in 3,840 patients between April 2001 and June 2016. Of these, 93 patients had MCRO requiring emergency decompression. Only patients in whom the colorectal lesion was ultimately resected were included; thus, the present study included 62 patients treated with MCRO via SEMS placement as a BTS (n=25) or via ES (n=37). The rates of laparoscopic surgery, primary anastomosis, stoma formation, lymph node dissection, adverse events, 30-day mortality and disease-free survival were evaluated. The clinical success rate of SEMS placement was 92.0% (23/25). Compared with the ES group, the SEMS group had higher rates of laparoscopic surgery (68.0 vs. 2.7%; P<0.001) and primary anastomosis (88.0 vs. 51.4%; P=0.003), a greater number of dissected lymph nodes (30 vs. 18; P=0.001), and lower incidences of stoma formation (24.0 vs. 67.6%; P=0.002) and overall adverse events (24.0 vs. 62.2%; P=0.004). The 30-day mortality and disease-free survival of the SEMS group were not significantly different to that of the ES group (0 vs. 2.7%; P=1.000; log-rank test; P=0.10). In conclusion, as long as adverse events such as perforation are minimized, SEMS placement as a BTS could be a first treatment option for MCRO. The present study is registered in the University Hospital Medical Network Clinical Trials Registry (UMIN R000034868).
Keywords: colorectal cancer; emergency surgery; malignant colorectal obstruction; self-expanding metallic stent.
Copyright: © Yagawa et al.
Figures
Similar articles
-
Short- and long-term outcomes after colonic self-expandable metal stent placement for malignant large-bowel obstruction as a bridge to surgery focus on the feasibility of the laparoscopic approach: a retrospective, single center study.World J Surg Oncol. 2020 Oct 13;18(1):265. doi: 10.1186/s12957-020-02039-8. World J Surg Oncol. 2020. PMID: 33050929 Free PMC article.
-
[An Analysis of Placement of a Self-Expanding Metallic Stent as Bridge to Surgery for Surgical Resection of StageⅣ Obstructive Colorectal Cancers].Gan To Kagaku Ryoho. 2015 Nov;42(12):1533-6. Gan To Kagaku Ryoho. 2015. PMID: 26805087 Japanese.
-
Bridge to surgery using a self-expandable metallic stent for stages II-III obstructive colorectal cancer.BMC Surg. 2020 Aug 20;20(1):189. doi: 10.1186/s12893-020-00847-z. BMC Surg. 2020. PMID: 32819354 Free PMC article.
-
Obstructing Left-Sided Colonic Cancer: Is Endoscopic Stenting a Bridge to Surgery or a Bridge to Nowhere?Dig Dis Sci. 2020 Oct;65(10):2789-2799. doi: 10.1007/s10620-020-06403-2. Dig Dis Sci. 2020. PMID: 32583222 Review.
-
Which treatment strategy is optimal for acute left-sided malignant colonic obstruction? A Bayesian meta-analysis.Int J Colorectal Dis. 2023 Aug 17;38(1):217. doi: 10.1007/s00384-023-04489-4. Int J Colorectal Dis. 2023. PMID: 37589792 Review.
Cited by
-
Emergency Management of Obstructive Colorectal Cancer - A Retrospective Study of Efficacy and Safety in Self-expanding Metallic Stents and Trans-anal Tubes.In Vivo. 2021 Jul-Aug;35(4):2289-2296. doi: 10.21873/invivo.12502. In Vivo. 2021. PMID: 34182508 Free PMC article.
-
Transforming outcomes: the pivotal role of self-expanding metal stents in right- and left-sided malignant colorectal obstructions-bridge to surgery: a comprehensive review and meta-analysis.Clin Endosc. 2025 Mar;58(2):240-252. doi: 10.5946/ce.2024.120. Epub 2025 Feb 3. Clin Endosc. 2025. PMID: 39895121 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous
