Cardiovascular Magnetic Resonance Imaging and Heart Failure
- PMID: 33686516
- PMCID: PMC7939452
- DOI: 10.1007/s11886-021-01464-9
Cardiovascular Magnetic Resonance Imaging and Heart Failure
Abstract
Purpose of review: The purpose of this review is to summarize the application of cardiac magnetic resonance (CMR) in the diagnostic and prognostic evaluation of patients with heart failure (HF).
Recent findings: CMR is an important non-invasive imaging modality in the assessment of ventricular volumes and function and in the analysis of myocardial tissue characteristics. The information derived from CMR provides a comprehensive evaluation of HF. Its unique ability of tissue characterization not only helps to reveal the underlying etiologies of HF but also offers incremental prognostic information. CMR is a useful non-invasive tool for the diagnosis and assessment of prognosis in patients suffering from heart failure.
Keywords: Cardiomyopathy; Cardiovascular magnetic resonance; Heart failure; Late gadolinium enhancement.
Conflict of interest statement
Chuanfen Liu declares no conflicts of interest.
Victor A. Ferrari reports grant support from the NIH; he is on the Senior Advisory Board for the
Yuchi Han reports grant support from the NIH and Pfizer and personal fees from GE, and she is also an Associate Editor for the
Figures
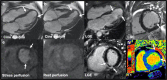
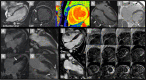


References
-
- Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE, Jr, Drazner MH, et al. (2013) ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013;62(16):e147–e239. doi: 10.1016/j.jacc.2013.05.019. - DOI - PubMed
-
- Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, et al. (2016) ESC guidelines for the diagnosis and treatment of acute and chronic heart failure: the task force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2016;37(27):2129–2200. doi: 10.1093/eurheartj/ehw128. - DOI - PubMed
-
- Virani SS, Alonso A, Benjamin EJ, Bittencourt MS, Callaway CW, Carson AP, et al. Heart disease and stroke statistics-2020 update: a report from the American Heart Association. Circulation. 2020; CIR0000000000000757. 10.1161/CIR.0000000000000757 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

