Incidence, clinical characteristics, risk factors and outcomes of meningoencephalitis in patients with COVID-19
- PMID: 33686558
- PMCID: PMC7939927
- DOI: 10.1007/s10096-021-04206-5
Incidence, clinical characteristics, risk factors and outcomes of meningoencephalitis in patients with COVID-19
Abstract
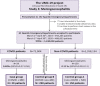
We investigated the incidence, clinical characteristics, risk factors, and outcome of meningoencephalitis (ME) in patients with COVID-19 attending emergency departments (ED), before hospitalization. We retrospectively reviewed all COVID patients diagnosed with ME in 61 Spanish EDs (20% of Spanish EDs, COVID-ME) during the COVID pandemic. We formed two control groups: non-COVID patients with ME (non-COVID-ME) and COVID patients without ME (COVID-non-ME). Unadjusted comparisons between cases and controls were performed regarding 57 baseline and clinical characteristics and 4 outcomes. Cerebrospinal fluid (CSF) biochemical and serologic findings of COVID-ME and non-COVID-ME were also investigated. We identified 29 ME in 71,904 patients with COVID-19 attending EDs (0.40‰, 95%CI=0.27-0.58). This incidence was higher than that observed in non-COVID patients (150/1,358,134, 0.11‰, 95%CI=0.09-0.13; OR=3.65, 95%CI=2.45-5.44). With respect to non-COVID-ME, COVID-ME more frequently had dyspnea and chest X-ray abnormalities, and neck stiffness was less frequent (OR=0.3, 95%CI=0.1-0.9). In 69.0% of COVID-ME, CSF cells were predominantly lymphocytes, and SARS-CoV-2 antigen was detected by RT-PCR in 1 patient. The clinical characteristics associated with a higher risk of presenting ME in COVID patients were vomiting (OR=3.7, 95%CI=1.4-10.2), headache (OR=24.7, 95%CI=10.2-60.1), and altered mental status (OR=12.9, 95%CI=6.6-25.0). COVID-ME patients had a higher in-hospital mortality than non-COVID-ME patients (OR=2.26; 95%CI=1.04-4.48), and a higher need for hospitalization (OR=8.02; 95%CI=1.19-66.7) and intensive care admission (OR=5.89; 95%CI=3.12-11.14) than COVID-non-ME patients. ME is an unusual form of COVID presentation (<0.5‰ cases), but is more than 4-fold more frequent than in non-COVID patients attending the ED. As the majority of these MEs had lymphocytic predominance and in one patient SARS-CoV-2 antigen was detected in CSF, SARS-CoV-2 could be the cause of most of the cases observed. COVID-ME patients had a higher unadjusted in-hospital mortality than non-COVID-ME patients.
Keywords: COVID-19; Clinical characteristics; Incidence; Meningoencephalitis; Outcome; Risk factors; SARS-Cov-2.
© 2021. The Author(s), under exclusive licence to Springer-Verlag GmbH Germany, part of Springer Nature.
Conflict of interest statement
The authors declare no competing interests.
Figures
References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous